Arie Zainul Fatoni 1 , Indy Zahrotul Firdaus 2 , Dearisa Surya Yudhantara 3 , Frilya Rachma Putri 4 , Ratri Istiqomah 5 , Winarni Dian 6 , Zuhrotun Ulya 7
Author affiliations:
Background & objective: The Coronavirus Disease 2019 (COVID-19) pandemic has imposed significant stress on health workers adversely affecting their mental health and reducing their quality of life leading to impaired cognitive and emotional capacity, leading to suboptimal decision-making. This study examined the psychological status in health workers providing services in the COVID-19 ICU at tertiary hospital RSUD Dr. Saiful Anwar Malang and to identify groups at high risk.
Methodology: The method used was a cross-sectional research method using an online form containing five forms to assess depression scores (PHQ-9), anxiety (GAD-7), burnout (MBI), spirituality (DSES), and self-compassion (SCS) and distributed to ICU health workers in COVID-19 ICU and those in regular ICU at RSUD Dr. Saiful Anwar Malang.
Results: The results demonstrated a significant difference in anxiety levels between health workers in COVID-19 ICU and those in regular ICU (P = 0.024). Additionally, the sociodemographic group identified as being at significant risk for psychological distress was the resident group (P < 0.05).
Conclusion: The COVID-19 pandemic influences the psychological status of health workers, especially in the resident group, and indicates a high urgency to overcome problems to improve the performance of health workers. The study recommends further investigation and effective management of healthcare workers' mental health.
Abbreviations: DSES: Daily Spiritual Experience Scale, GAD-7: Generalized Anxiety Disorder-7, ICU: Intensive Care Unit, MBI: Maslach Burnout Inventory, PHQ-9: Patient Health Questionnaire-9, SCS: Self-Compassion Scale
Keywords: Burnout; COVID-19; Health Personnel; Intensive Care Unit; Psychological Distress; Self-Compassion
Citation: Fatoni AZ, Firdaus IZ, Yudhantara DS, Putri FR, Istiqomah R, Dian W, Ulya Z. Psychological status among health workers in a COVID-19 and a regular intensive care unit of an Indonesian tertiary hospital. Anaesth. pain intensive care 2026;30(2):224-231. DOI: 10.35975/apic.v30i2.3130
Received: May 09, 2025; Revised: October 26, 2025; Accepted: January 01, 2026
1. INTRODUCTION
Healthcare professionals in the Intensive Care Unit (ICU) faced unprecedented challenges during the COVID-19 pandemic, as they provided care while facing extraordinary difficulties.1 Tertiary hospitals, which offer comprehensive health care services at provincial or national levels, experienced significant surges in patient admission especially in COVID-19. The increase in the number of critical care patients in the ICU has been reported to cause fear, anxiety, and uncertainty among ICU staff. Increased workload, limited autonomy in the work environment, and the emotional burden of caring for critically ill patient that have been intensified by the COVID-19 pandemic and are significant contributors to poor mental health among healthcare workers, particulary those in the ICUs, including moral injury and psychological disorders (depression, anxiety, burnout, and decreased quality of life).2,3
Research conducted by Liu et al. (2020) showed that the incidence of depression and anxiety in epidemiologists and health workers was 50.7% and 44.7%, respectively. Another study showed an increased incidence of burnout in health workers who worked in the ICU and experienced trauma related to COVID-19. Another study showed an approximately four-fold risk of decreased quality of life in health workers who experienced moderate-severe depression and moderate-severe anxiety.4 The level of spirituality of the healthcare worker also had influence to this. Additional research had demonstrated that increases in life quality were impossible without spiritual well-being because it is necessary for the effective functioning of other facets of human existence, including the mental and social ones. This condition impairs the cognitive and emotional capacity of medical personnel, leading to suboptimal decision-making during critical medical interventions.2 Therefore, the psychological condition of health workers who work in the ICU, both COVID-19 ICU and regular ICU needs to be studied
The COVID-19 pandemic placed unprecedented psychological demands on healthcare workers (HCWs), with consistently elevated rates of anxiety, depression, post-traumatic stress symptoms, and burnout—particularly among ICU teams and nurses. Large early surveys reported that ~45% of ICU staff met thresholds for probable mental health disorders, with nurses showing higher distress than doctors, underscoring an urgent need for protective strategies at individual and organizational levels.5 Evidence from LMIC and regional settings echoes this burden. An Indonesian cross-sectional study one month after the national outbreak found significantly higher odds of depressive symptoms and burnout among HCWs with direct COVID-19 exposure, highlighting the compounded risks of frontline work, workload, and resource constraints.6
Beyond symptom prevalence, spirituality and religiosity emerged as salient coping resources during the pandemic. An integrative review concluded that spiritual care and spiritual well-being were associated with reduced stress, anxiety, and depression among both patients and HCWs, and recommended structured inclusion of spiritual assessment and support in clinical practice.7 In Indonesia, hospital-based data linked higher workplace spirituality with lower nurse anxiety during COVID-19, suggesting culturally consonant organizational practices (e.g., meaning-centered work, community, alignment of values) may buffer distress.8 Self-compassion has also been identified as a protective factor for HCW resilience. In palliative care providers, higher self-compassion and mindful self-care explained substantial variance in resilience, supporting their role as modifiable targets. Correlational work among mental health professionals similarly links greater self-compassion with lower burnout and better professional quality of life.9 Intervention studies, though fewer, are promising. Short, online mindfulness programs for HCWs have been feasible and associated with improvements in resilience and stress; scalable skill-based approaches may fit surge conditions and staffing constraints.10 Early post-pandemic pilots of bite-sized self-compassion tools for HCWs report gains in resilience and well-being, pointing to pragmatic, low-burden formats that can be layered onto routine work.11
The purpose of this study was to examine the comparison of psychological status in health workers who provide services in the COVID-19 ICU and the regular ICU at tertiary hospital RSUD Dr. Saiful Anwar Malang and to identify groups with high risk and expected to be a reference in determining policies related to rotation and screening for mental disorders, especially regarding depression, burnout, anxiety, self-compassion, and spirituality in health workers in the COVID-19 ICU and regular ICU. We hypotisized that health workers in the COVID-19 ICU have significantly higher levels of anxiety, burnout and depression compared to those in regular ICUs due to increased exposure to critically ill patients and higher workloads. Additionally, we hypotisized sociodemographic factors, such as employment status, age, and gender, significantly influence the psychological status (burnout, depression, anxiety, spirituality, and self-compassion) of ICU health workers.
The study followed the Equator Network recommendations with the STROBE Statement for observational studies. The research to be carried out was analytic observational descriptive quantitative research with a cross-sectional study design. This research was conducted in November 2021 and was conducted online within the scope of the ICU of Saiful Anwar Hospital Malang.
This study included health workers who provide health services in the regular ICU and ICU COVID-19 of Saiful Anwar Hospital Malang, actively providing services in the COVID-19 ICU and the regular ICU of RSSA and agree to conduct research. Some of the exclusion criteria for respondents include (1) not filling out the questionnaire completely, (2) being absent or absent due to illness or specific reasons when the research was conducted, and (3) having a history of emotional and behavioral disorders. A total of 107 respondents initially agreed to participate and provided informed consent. After excluding 7 respondents with a history of emotional and behavioral disorders prior to the COVID-19 pandemic, 100 respondents were included in the final analysis: 48 assigned to the COVID-19 ICU group and 52 to the regular ICU group.
The instrument used in this study was an online form questionnaire consisting of three parts, namely the consent form, personal data, and scoring the psychological status of health workers.
Several questionnaires to measure the psychological status of health workers were used :
Univariate analysis was conducted on sociodemographic characteristics data to describe the characteristics of respondents. The level of psychological status of regular ICU health workers and ICU COVID-19 were correlated, and the level of psychological status and respondents' sociodemographic characteristics were correlated, according to Kruskal Wallis andMannWhitney analyses.
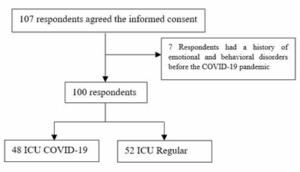
Figure 1. Flow diagram of participant selection.
In this study, 107 respondents agreed to informed consent and filled in completely. All characteristics of the respondents are attached in Table 1. Male responders made up 53% of the total. In addition, at least 78% of the respondents were married in their marital status. Respondents with contract employment status (44%) made up most of the respondents. Nurses were the most numerous health worker type group in this study (67%) and most health workers had been working for 1-3 years (36%).
The comparison of psychological status between health workers in the COVID-19 ICU and regular ICU shown in Table 2, that the status of burnout, depression, spirituality, and self-compassion did not show significant differences (p > 0.05). Overall, 98% experienced moderate burnout, and 73% minimal depression. However, the average of depression score in the COVID-19 ICU group was higher than in the regular ICU group. A total of 76% of the respodents demonstrated a high level of spirituality. Health workers in the COVID-19 ICU exhibited a lower mean level of self-compassion compared to those in the regular ICU. Significant results were seen in the comparison of anxiety scores where the anxiety score value of COVID-19 ICU health workers was higher than regular ICU health workers (P < 0.05).
The correlation analysis of psychological status scores and sociodemographic characteristics is presented in Table 3. The level of burnout in the self-esteem dimension was significantly correlated with the sociodemographic characteristics of health worker type (P = 0.04) and employment status (P = 0.005). The level of depression showed a significant correlation with age (P = 0.03), health workers (P = 0.039), and employment status (P = 0.005). Anxiety levels were significantly correlated with employment status (P = 0.013) and gender (P = 0.046). The spiritual level had significant correlation with gender (P = 0.033), employment status (P = 0.028), and health worker type (P = 0.019). Additionally, the level of self-compassion with health worker type (P = 0.004) and employment status (P = 0.004).
Based on the results of the sociodemographic study, more than half of the health workers who provide services in the ICU were male, aged 26-35 years (early adulthood), and married. The most common type of health worker was nurse. Most of the health workers in the ICU had contract status and worked for 1-3 years. The COVID-19 ICU had a larger number of health workers when compared to health workers who provide services in the regular ICU. According to data analysis, the results of the psychological status assessment in this study showed that only anxiety status had significant differences between the COVID-19 ICU and regular ICU groups. Anxiety status in COVID-19 ICU health workers showed a higher level when compared to health workers in regular ICUs. This was consistent with the findings of research conducted by Deni (2021), where groups with high risk, namely groups that have higher exposure to COVID-19 patients, have higher levels of anxiety12. Other psychological status did not have a significant difference, possibly because health workers have adapted to the COVID-19 pandemic and the level of fluctuation in cases during the COVID-19 pandemic.13 This could be correlate to higher risk of exposure to the virus, and mostly concerned to transmit the virus to their relatives14. In contrast, keeping close with the love ones may reduce anxiety and distress during working in COVID-19 pandemic.15 This might one of factors influencing the psychological status among the health workers during COVID-19 pandemic.
In addition, the correlation of anxiety levels in health workers showed significant correlation results in the employment status variable. The resident group had a higher level of anxiety than the other groups. This might relate to the increase/change in service time of residents and also the fear of getting or transmitting the disease to those closest to them16. Additionally most residents are younger than specialists or senior nurses, which also correlates with clinical experience and the level of adaptation to new things. Other results show that the mean anxiety score of male health workers tends to be higher when compared to female health workers. This is because men usually have more anxiety about their work than women.17 In burnout status, a significant correlation was found with the variables of type of health worker and
The spirituality status of health workers showed a significant relationship with the variables of gender, employment status, and type of health worker. In this study, the correlation study showed that the female group had a higher level of spirituality than the male group. The most likely explanation is that women basically have the biological state of giving birth and breastfeeding children, so women are easier in having a particular connection with the surrounding environment. In addition, residents showed lower level of spirituality when compared to the other groups. High workload with low clinical experience in dealing with clinical cases that are charged has an effect on poor stress management which leads to low spiritual health.8 In addition, the resident group had the lowest level of self-compassion. The correlation between the level of burnout and self-compassion is the opposite correlation, the higher the burnout, the lower the self-compassion.22 The level of self-compassion in a person will certainly illustrate how a person copes with his daily problems. Someone with a high level of self-compassion will find it easier to cope with anxiety and work pressure.23
The analysis results in this study showed significant values in resident in burnout status, anxiety, depression, spirituality to self-compassion. In research conducted by Rushing (2020), found that resident is a group that is very vulnerable to stressors, both internal and external stressors.24 The high expectations of themselves, the many tasks that must be done during the long working hours of resident are sometimes not supported with clinical knowledge that is needed in daily clinical practice, so that most resident feel embarrassed when discussing with specialists as supervisors. This feeling of shame will have a dramatic effect in every activity carried out, especially when in the hospital and lead to low sensitivity and understanding of other health workers, resulting in low empathy and self-compassion.25
Health workers in COVID-19 ICUs experienced significantly higher levels of anxiety compared to those in regular ICUs, with residents identified as the most vulnerable group. These findings underscore the need for early psychological screening, targeted interventions, and supportive policies to protect the mental health of ICU personnel. Enhancing self-compassion and spirituality may further strengthen resilience and improve both staff well-being and patient care. Future multi-center and longitudinal studies are warranted to confirm these results and evaluate effective interventions.
6. Data availability
The numerical data generated in this research is available with the authors and can be provided on request.
7. Source(s) of Support and Funding
The authors received no specific funding for this work.
8. Conflict of Interest statement
The authors declare no conflict of interest
9. Consent to Participate
All participants who met the inclusion criteria provided written consent to participate in this study through an informed consent form integrated into the questionere form. This process was conducted in accordance with ethical research guidelines and approved by the relevant institutional ethics committee
10. Ethical considerations
The ethical review for this study was approved by the Health Research Ethics Committee of Dr. Saiful Anwar Regional General Hospital Malang with approval number 400/145/K.3/302/2021
11. Authors contributions
The manuscript has been read and approved by all authors. Conceptualization: AZF and DSY, Data curation: AZF, FRP, and DSY, Formal analysis: WD, DSY, and AZF, Methodology: AZF and IZF, Software: ZU, Supervision: AZF, Validation: DSY and IZF, Visualization: FRP, RI, ZU, Writing – Original Draft: IZF and RI, Writing – Review and Editing: AZF and WD.
Author affiliations:
- Arie Zainul Fatoni, MD, Department of Anesthesiology & Intensive Therapy, Dr. Saiful Anwar Hospital–Faculty of Medicine, Brawijaya University, Jl. Jaksa Agung Suprapto No.2, Malang 65111, Indonesia; Email: ariezainulfatoni@ub.ac.id | ORCID: 0000-0002-3314-5586
- Indy Zahrotul Firdaus, MD, Faculty of Medicine, Brawijaya University, Jl. Veteran, Malang 65145, Indonesia; Email: rocyndyfirda@gmail.com | ORCID: 0000-0002-8182-9843
- Dearisa Surya Yudhantara, MD, Department of Psychiatry, Dr. Saiful Anwar Hospital–Faculty of Medicine, Brawijaya University, Jl. Jaksa Agung Suprapto No.2, Malang 65111, Indonesia; Email: drdsyudhantara.fk@ub.ac.id | ORCID: 0000-0003-2941-5077
- Frilya Rachma Putri, MD, Department of Psychiatry, Dr. Saiful Anwar Hospital–Faculty of Medicine, Brawijaya University, Jl. Jaksa Agung Suprapto No.2, Malang 65111, Indonesia; Email: frilya.yudi@ub.ac.id | ORCID: 0000-0003-4695-1349
- Ratri Istiqomah, MD, Department of Psychiatry, Dr. Saiful Anwar Hospital–Faculty of Medicine, Brawijaya University, Jl. Jaksa Agung Suprapto No.2, Malang 65111, Indonesia; Email: ratri.istiqomah@ub.ac.id | ORCID: 0009-0003-0406-6007
- Winarni Dian, MD, Department of Psychiatry, Dr. Saiful Anwar Hospital–Faculty of Medicine, Brawijaya University, Jl. Jaksa Agung Suprapto No.2, Malang 65111, Indonesia; Email: winarni.dian@ub.ac.id | ORCID: 0009-0000-4441-1213
- Zuhrotun Ulya, MD, Department of Psychiatry, Dr. Saiful Anwar Hospital–Faculty of Medicine, Brawijaya University, Jl. Jaksa Agung Suprapto No.2, Malang 65111, Indonesia; Email: dr.zulya@ub.ac.id | ORCID: 0000-0002-3701-8250
ABSTRACT
Background & objective: The Coronavirus Disease 2019 (COVID-19) pandemic has imposed significant stress on health workers adversely affecting their mental health and reducing their quality of life leading to impaired cognitive and emotional capacity, leading to suboptimal decision-making. This study examined the psychological status in health workers providing services in the COVID-19 ICU at tertiary hospital RSUD Dr. Saiful Anwar Malang and to identify groups at high risk.
Methodology: The method used was a cross-sectional research method using an online form containing five forms to assess depression scores (PHQ-9), anxiety (GAD-7), burnout (MBI), spirituality (DSES), and self-compassion (SCS) and distributed to ICU health workers in COVID-19 ICU and those in regular ICU at RSUD Dr. Saiful Anwar Malang.
Results: The results demonstrated a significant difference in anxiety levels between health workers in COVID-19 ICU and those in regular ICU (P = 0.024). Additionally, the sociodemographic group identified as being at significant risk for psychological distress was the resident group (P < 0.05).
Conclusion: The COVID-19 pandemic influences the psychological status of health workers, especially in the resident group, and indicates a high urgency to overcome problems to improve the performance of health workers. The study recommends further investigation and effective management of healthcare workers' mental health.
Abbreviations: DSES: Daily Spiritual Experience Scale, GAD-7: Generalized Anxiety Disorder-7, ICU: Intensive Care Unit, MBI: Maslach Burnout Inventory, PHQ-9: Patient Health Questionnaire-9, SCS: Self-Compassion Scale
Keywords: Burnout; COVID-19; Health Personnel; Intensive Care Unit; Psychological Distress; Self-Compassion
Citation: Fatoni AZ, Firdaus IZ, Yudhantara DS, Putri FR, Istiqomah R, Dian W, Ulya Z. Psychological status among health workers in a COVID-19 and a regular intensive care unit of an Indonesian tertiary hospital. Anaesth. pain intensive care 2026;30(2):224-231. DOI: 10.35975/apic.v30i2.3130
Received: May 09, 2025; Revised: October 26, 2025; Accepted: January 01, 2026
1. INTRODUCTION
Healthcare professionals in the Intensive Care Unit (ICU) faced unprecedented challenges during the COVID-19 pandemic, as they provided care while facing extraordinary difficulties.1 Tertiary hospitals, which offer comprehensive health care services at provincial or national levels, experienced significant surges in patient admission especially in COVID-19. The increase in the number of critical care patients in the ICU has been reported to cause fear, anxiety, and uncertainty among ICU staff. Increased workload, limited autonomy in the work environment, and the emotional burden of caring for critically ill patient that have been intensified by the COVID-19 pandemic and are significant contributors to poor mental health among healthcare workers, particulary those in the ICUs, including moral injury and psychological disorders (depression, anxiety, burnout, and decreased quality of life).2,3
Research conducted by Liu et al. (2020) showed that the incidence of depression and anxiety in epidemiologists and health workers was 50.7% and 44.7%, respectively. Another study showed an increased incidence of burnout in health workers who worked in the ICU and experienced trauma related to COVID-19. Another study showed an approximately four-fold risk of decreased quality of life in health workers who experienced moderate-severe depression and moderate-severe anxiety.4 The level of spirituality of the healthcare worker also had influence to this. Additional research had demonstrated that increases in life quality were impossible without spiritual well-being because it is necessary for the effective functioning of other facets of human existence, including the mental and social ones. This condition impairs the cognitive and emotional capacity of medical personnel, leading to suboptimal decision-making during critical medical interventions.2 Therefore, the psychological condition of health workers who work in the ICU, both COVID-19 ICU and regular ICU needs to be studied
The COVID-19 pandemic placed unprecedented psychological demands on healthcare workers (HCWs), with consistently elevated rates of anxiety, depression, post-traumatic stress symptoms, and burnout—particularly among ICU teams and nurses. Large early surveys reported that ~45% of ICU staff met thresholds for probable mental health disorders, with nurses showing higher distress than doctors, underscoring an urgent need for protective strategies at individual and organizational levels.5 Evidence from LMIC and regional settings echoes this burden. An Indonesian cross-sectional study one month after the national outbreak found significantly higher odds of depressive symptoms and burnout among HCWs with direct COVID-19 exposure, highlighting the compounded risks of frontline work, workload, and resource constraints.6
Beyond symptom prevalence, spirituality and religiosity emerged as salient coping resources during the pandemic. An integrative review concluded that spiritual care and spiritual well-being were associated with reduced stress, anxiety, and depression among both patients and HCWs, and recommended structured inclusion of spiritual assessment and support in clinical practice.7 In Indonesia, hospital-based data linked higher workplace spirituality with lower nurse anxiety during COVID-19, suggesting culturally consonant organizational practices (e.g., meaning-centered work, community, alignment of values) may buffer distress.8 Self-compassion has also been identified as a protective factor for HCW resilience. In palliative care providers, higher self-compassion and mindful self-care explained substantial variance in resilience, supporting their role as modifiable targets. Correlational work among mental health professionals similarly links greater self-compassion with lower burnout and better professional quality of life.9 Intervention studies, though fewer, are promising. Short, online mindfulness programs for HCWs have been feasible and associated with improvements in resilience and stress; scalable skill-based approaches may fit surge conditions and staffing constraints.10 Early post-pandemic pilots of bite-sized self-compassion tools for HCWs report gains in resilience and well-being, pointing to pragmatic, low-burden formats that can be layered onto routine work.11
The purpose of this study was to examine the comparison of psychological status in health workers who provide services in the COVID-19 ICU and the regular ICU at tertiary hospital RSUD Dr. Saiful Anwar Malang and to identify groups with high risk and expected to be a reference in determining policies related to rotation and screening for mental disorders, especially regarding depression, burnout, anxiety, self-compassion, and spirituality in health workers in the COVID-19 ICU and regular ICU. We hypotisized that health workers in the COVID-19 ICU have significantly higher levels of anxiety, burnout and depression compared to those in regular ICUs due to increased exposure to critically ill patients and higher workloads. Additionally, we hypotisized sociodemographic factors, such as employment status, age, and gender, significantly influence the psychological status (burnout, depression, anxiety, spirituality, and self-compassion) of ICU health workers.
2. METHODOLOGY
The study followed the Equator Network recommendations with the STROBE Statement for observational studies. The research to be carried out was analytic observational descriptive quantitative research with a cross-sectional study design. This research was conducted in November 2021 and was conducted online within the scope of the ICU of Saiful Anwar Hospital Malang.
This study included health workers who provide health services in the regular ICU and ICU COVID-19 of Saiful Anwar Hospital Malang, actively providing services in the COVID-19 ICU and the regular ICU of RSSA and agree to conduct research. Some of the exclusion criteria for respondents include (1) not filling out the questionnaire completely, (2) being absent or absent due to illness or specific reasons when the research was conducted, and (3) having a history of emotional and behavioral disorders. A total of 107 respondents initially agreed to participate and provided informed consent. After excluding 7 respondents with a history of emotional and behavioral disorders prior to the COVID-19 pandemic, 100 respondents were included in the final analysis: 48 assigned to the COVID-19 ICU group and 52 to the regular ICU group.
The instrument used in this study was an online form questionnaire consisting of three parts, namely the consent form, personal data, and scoring the psychological status of health workers.
Several questionnaires to measure the psychological status of health workers were used :
- Patient Health Questionnaire-9 (PHQ-9) to measure the subject's level of depression.
- Generalized Anxiety Disorder-7 (GAD-7) to measure the subject's anxiety level.
- Maslach Burnout Inventory (MBI) to measure the subject's burnout level.
- Daily Spiritual Experience Scale (DSES) to measure the spiritual level of the subject.
- Self-Compassion Scale (SCS) to measure the subject's level of compassion.
Univariate analysis was conducted on sociodemographic characteristics data to describe the characteristics of respondents. The level of psychological status of regular ICU health workers and ICU COVID-19 were correlated, and the level of psychological status and respondents' sociodemographic characteristics were correlated, according to Kruskal Wallis andMannWhitney analyses.

Figure 1. Flow diagram of participant selection.
3. RESULTS
In this study, 107 respondents agreed to informed consent and filled in completely. All characteristics of the respondents are attached in Table 1. Male responders made up 53% of the total. In addition, at least 78% of the respondents were married in their marital status. Respondents with contract employment status (44%) made up most of the respondents. Nurses were the most numerous health worker type group in this study (67%) and most health workers had been working for 1-3 years (36%).
| Table 1: Sociodemographic characteristics of respondents | |||
| Characteristics | Total | ICU COVID | Regular ICU |
| Gender | |||
| · Men | 53 (53) | 26 (54.17) | 27(51.9) |
| · Women | 47 (47) | 22 (45.83) | 25 (48.1) |
| Age (years) | |||
| · Early Elderly (46-55) | 3 (3) | 0 (0) | 3 (5.77) |
| · Late Adult (36-45) | 15 (15) | 7 (14.58) | 8 (15.38) |
| · Early Adult (26-35) | 75 (75) | 36 (75) | 39 (75) |
| · Late Teens (17-25) | 7 (7) | 5 (10.42) | 2 (3.85) |
| Marriage Status | |||
| · Unmarried/Not Married | 20 (20) | 13 (27.08) | 7 (13.46) |
| · Married | 78 (78) | 33 (68.75) | 45 (86.53) |
| · Divorced/Widowed | 2 (2) | 2 (4.17) | 0 (0) |
| Last Education | |||
| · D3 / Equivalent | 47 (47) | 19 (39.58) | 28 (53.85) |
| · S1 / General Doctor / Equivalent | 47 (47) | 24 (50) | 23 (44.23) |
| · Master / Specialist / Equivalent | 6 (6) | 5 (10.42) | 1 (1.92) |
| Employment Status | |||
| · Civil servant | 27 (27) | 9 (18.75) | 18 (34.61) |
| · Contract | 44 (44) | 16 (33.33) | 28 (53.85) |
| · Volunteer | 11 (11) | 11 (22.92) | 0 (0) |
| · Resident | 18 (18) | 12 (25) | 6 (11.54) |
| Type of Health Worker | |||
| · Specialist Doctors | 4 (4) | 3 (6.25) | 1 (1.92) |
| · Resident | 21 (21) | 13 (27.08) | 8 (15.38) |
| · Midwife | 1 (1) | 0 (0) | 1 (1.92) |
| · Nurse | 67 (67) | 27 (56.25) | 40 (76.92) |
| · Pharmacist | 5 (5) | 4 (8.33) | 1 (1.92) |
| · Nutrisionist | 2 (2) | 1 (2) | 1 (1.92) |
| Years of Service | |||
| · < 1 year | 27 (27) | 15 (31.25) | 12 (23.08) |
| · 1-3 years | 36 (36) | 15 (31.25) | 21 (40.38) |
| · 3-5 years | 13 (13) | 9 (18.75) | 4 (7.69) |
| · > 5 years | 24 (24) | 9 (18.75) | 15 (28.85) |
| Data presented as n (%) | |||
The comparison of psychological status between health workers in the COVID-19 ICU and regular ICU shown in Table 2, that the status of burnout, depression, spirituality, and self-compassion did not show significant differences (p > 0.05). Overall, 98% experienced moderate burnout, and 73% minimal depression. However, the average of depression score in the COVID-19 ICU group was higher than in the regular ICU group. A total of 76% of the respodents demonstrated a high level of spirituality. Health workers in the COVID-19 ICU exhibited a lower mean level of self-compassion compared to those in the regular ICU. Significant results were seen in the comparison of anxiety scores where the anxiety score value of COVID-19 ICU health workers was higher than regular ICU health workers (P < 0.05).
| Table 2: Comparative psychological status between health workers in COVID-19 ICU and regular ICU | |||
| Psychological Status | ICU COVID | Regular ICU | P-value |
| Burnout | |||
| 1. Emotional Fatigue | |||
| Weight | 6 (12.5) | 6 (11.54) | 0.347 |
| Medium | 14 (29.17) | 8 (15.38) | |
| Lightweight | 28 (58.33) | 38 (73.08) | |
| Average score | 18.7 (Mild) | 16.62 (Mild) | |
| 2. Loss of Empathy | |||
| Weight | 6 (12.5) | 5 (9.62) | 0.66 |
| Medium | 22 (45.83) | 16 (30.77) | |
| Lightweight | 20 (41.67) | 31 (59.62) | |
| Average score | 7.4 (Medium) | 6.25 (Medium) | |
| 3. Self-esteem | |||
| High | 17 (35.42) | 12 (23.08) | 0.203 |
| Medium | 4 (8.33) | 1 (1.92) | |
| Low | 27 (56.25) | 39 (75) | |
| Average score | 39.4 (Medium) | 42.6 (Low) | |
| 4. Overall | |||
| High | 1 (2.08) | 1 (1.92) 0.954 51 (98.08) 0 (0) |
|
| Medium | 47 (97.92) | ||
| Low | 0 (0) | ||
| 5. Depression | |||
| Weight | 1 (2.08) | 0 (0) | 0.224 |
| Medium-Heavy | 1 (2.08) | 0 (0) | |
| Medium | 1 (2.08) | 1 (1.92) | |
| Lightweight | 11 (22.92) | 12 (23.08) | |
| Minimal | 34 (70.83) | 39 (75) | |
| Average score | 3.7 (Minimum) | 2.6 (Minimum) | |
| 6. Anxiety | |||
| Weight | 1 (2) | 0 (0) | 0.024 |
| Medium | 3 (6) | 0 (0) | |
| Lightweight | 11 (23) | 7 (13) | |
| Minimal | 33 (69) | 45 (87) | |
| Average score | 3.9 (Minimum) | 1.9 (Minimum) | |
| 7. Spiritual | |||
| High | 34 (70.83) | 42 (80.77) | 0.685 |
| Medium | 9 (18.75) | 8 (15.38) | |
| Low | 5 (10.42) | 2 (3.85) | |
| Average score | 71.3 (High) | 74.65 (High) | |
| 8. Self-Compassion | |||
| High | 23 (47.92) | 27 (51.92) | 0.354 |
| Medium | 25 (52.08) | 25 (48.08) | |
| Low | 0 | 0 | |
| Average score | 3.52 (High) | 3.65 (High) | |
The correlation analysis of psychological status scores and sociodemographic characteristics is presented in Table 3. The level of burnout in the self-esteem dimension was significantly correlated with the sociodemographic characteristics of health worker type (P = 0.04) and employment status (P = 0.005). The level of depression showed a significant correlation with age (P = 0.03), health workers (P = 0.039), and employment status (P = 0.005). Anxiety levels were significantly correlated with employment status (P = 0.013) and gender (P = 0.046). The spiritual level had significant correlation with gender (P = 0.033), employment status (P = 0.028), and health worker type (P = 0.019). Additionally, the level of self-compassion with health worker type (P = 0.004) and employment status (P = 0.004).
| Table 3: Significant associations between psychological domains and sociodemographic characteristics. | |||||||
| Psychological domain | Socio-
demographic variable |
Subgroup (n) | Median (IQR) | Test (stat) | p | Effect size r | Direction / note |
| Burnout — Self-esteem | Type of health worker | Specialist (4), Resident (21), Nurse (67), Pharmacist (5), Nutritionist (2), Midwife (1) | 49.3 (45–52); 30.7 (26–35); 43.4 (38–48); 43.6 (39–46); 48.5 (47–50); 45 (45–45) | Kruskal–Wallis H = X (df = 5) | 0.040 | r = 0.12 | Residents had the lowest self-esteem (highest burnout) |
| Burnout — Self-esteem | Employment status | Civil servant (27), Contract (44), Volunteer (11), Resident (18) | 39.7 (36–44); 46.2 (40–50); 38.7 (34–42); 31.9 (28–36) | Kruskal–Wallis H = X (df = 3) | 0.005 | r = 0.20 | Residents / contract lower self-esteem |
| Anxiety (GAD-7) | Employment status | Civil (27), Contract (44), Volunteer (11), Resident (18) | 2.8 (1–5); 1.9 (0–4); 3.6 (1–6); 4.8 (3–7) | Kruskal–Wallis H = X | 0.013 | r = 0.15 | Residents highest anxiety |
| Anxiety (GAD-7) | Gender | Men (53), Women (47) | 3.4 (2–6); 2.3 (1–4) | Mann–Whitney U = X, Z = X | 0.046 | r = 0.09 | Men higher anxiety |
| Spirituality (DSES) | Gender | Men (53), Women (47) | 70.1 (60–80); 76.3 (68–82) | Mann–Whitney U = X, Z = X | 0.033 | r = 0.10 | Women higher spirituality |
| Self-compassion (SCS) | Type of health worker / Employment | Specialist (4), Resident (21), Nurse (67), Pharmacist (5), Nutritionist (2), Midwife (1) | 3.65 (3.4-3.97); 3.17 (3-3.29); 3.68 (3.13-3.65); 3.74 (3.08-4.35); 4.12 (3.09-4.35); 4.03(3.55-4.68); | Kruskal–Wallis H = X | 0.004 | r = 0.18 | Residents lowest self-compassion |
| Self-compassion (SCS) | Type of health worker / Employment | Civil (27), Contract (44), Volunteer (11), Resident (18) | 3.59 (3.11-4.03); 3.72 (3.19-4.12); 3.66 (3.02-4.23); 3.2 (3-3.34) | Kruskal–Wallis H = X | 0.004 | r = 0.15 | Residents lowest self-compassion |
| Note : Medians (IQR) reported; Kruskal–Wallis (KW) or Mann–Whitney U tests used. Effect size r = Z/√N_total. Significant p-values in bold. | |||||||
3. DISCUSSION
Based on the results of the sociodemographic study, more than half of the health workers who provide services in the ICU were male, aged 26-35 years (early adulthood), and married. The most common type of health worker was nurse. Most of the health workers in the ICU had contract status and worked for 1-3 years. The COVID-19 ICU had a larger number of health workers when compared to health workers who provide services in the regular ICU. According to data analysis, the results of the psychological status assessment in this study showed that only anxiety status had significant differences between the COVID-19 ICU and regular ICU groups. Anxiety status in COVID-19 ICU health workers showed a higher level when compared to health workers in regular ICUs. This was consistent with the findings of research conducted by Deni (2021), where groups with high risk, namely groups that have higher exposure to COVID-19 patients, have higher levels of anxiety12. Other psychological status did not have a significant difference, possibly because health workers have adapted to the COVID-19 pandemic and the level of fluctuation in cases during the COVID-19 pandemic.13 This could be correlate to higher risk of exposure to the virus, and mostly concerned to transmit the virus to their relatives14. In contrast, keeping close with the love ones may reduce anxiety and distress during working in COVID-19 pandemic.15 This might one of factors influencing the psychological status among the health workers during COVID-19 pandemic.
In addition, the correlation of anxiety levels in health workers showed significant correlation results in the employment status variable. The resident group had a higher level of anxiety than the other groups. This might relate to the increase/change in service time of residents and also the fear of getting or transmitting the disease to those closest to them16. Additionally most residents are younger than specialists or senior nurses, which also correlates with clinical experience and the level of adaptation to new things. Other results show that the mean anxiety score of male health workers tends to be higher when compared to female health workers. This is because men usually have more anxiety about their work than women.17 In burnout status, a significant correlation was found with the variables of type of health worker and
The spirituality status of health workers showed a significant relationship with the variables of gender, employment status, and type of health worker. In this study, the correlation study showed that the female group had a higher level of spirituality than the male group. The most likely explanation is that women basically have the biological state of giving birth and breastfeeding children, so women are easier in having a particular connection with the surrounding environment. In addition, residents showed lower level of spirituality when compared to the other groups. High workload with low clinical experience in dealing with clinical cases that are charged has an effect on poor stress management which leads to low spiritual health.8 In addition, the resident group had the lowest level of self-compassion. The correlation between the level of burnout and self-compassion is the opposite correlation, the higher the burnout, the lower the self-compassion.22 The level of self-compassion in a person will certainly illustrate how a person copes with his daily problems. Someone with a high level of self-compassion will find it easier to cope with anxiety and work pressure.23
The analysis results in this study showed significant values in resident in burnout status, anxiety, depression, spirituality to self-compassion. In research conducted by Rushing (2020), found that resident is a group that is very vulnerable to stressors, both internal and external stressors.24 The high expectations of themselves, the many tasks that must be done during the long working hours of resident are sometimes not supported with clinical knowledge that is needed in daily clinical practice, so that most resident feel embarrassed when discussing with specialists as supervisors. This feeling of shame will have a dramatic effect in every activity carried out, especially when in the hospital and lead to low sensitivity and understanding of other health workers, resulting in low empathy and self-compassion.25
5. CONCLUSION
Health workers in COVID-19 ICUs experienced significantly higher levels of anxiety compared to those in regular ICUs, with residents identified as the most vulnerable group. These findings underscore the need for early psychological screening, targeted interventions, and supportive policies to protect the mental health of ICU personnel. Enhancing self-compassion and spirituality may further strengthen resilience and improve both staff well-being and patient care. Future multi-center and longitudinal studies are warranted to confirm these results and evaluate effective interventions.
6. Data availability
The numerical data generated in this research is available with the authors and can be provided on request.
7. Source(s) of Support and Funding
The authors received no specific funding for this work.
8. Conflict of Interest statement
The authors declare no conflict of interest
9. Consent to Participate
All participants who met the inclusion criteria provided written consent to participate in this study through an informed consent form integrated into the questionere form. This process was conducted in accordance with ethical research guidelines and approved by the relevant institutional ethics committee
10. Ethical considerations
The ethical review for this study was approved by the Health Research Ethics Committee of Dr. Saiful Anwar Regional General Hospital Malang with approval number 400/145/K.3/302/2021
11. Authors contributions
The manuscript has been read and approved by all authors. Conceptualization: AZF and DSY, Data curation: AZF, FRP, and DSY, Formal analysis: WD, DSY, and AZF, Methodology: AZF and IZF, Software: ZU, Supervision: AZF, Validation: DSY and IZF, Visualization: FRP, RI, ZU, Writing – Original Draft: IZF and RI, Writing – Review and Editing: AZF and WD.
12. REFERENCES
- Akgün KM, Collett D, Feder SL, Shamas T, Schulman-Green D. Sustaining frontline ICU healthcare workers during the COVID-19 pandemic and beyond. Hear Lung [Internet]. 2020 Jul 1 [cited 2022 Feb 16];49(4):346. Available from: /pmc/articles/PMC7256543/
- Suryavanshi N, Kadam A, Dhumal G, Nimkar S, Mave V, Gupta A, et al. Mental health and quality of life among healthcare professionals during the COVID-19 pandemic in India. Brain Behav. 2020 Nov;10(11).
- Greenberg N, Weston D, Hall C, Caulfield T, Williamson V, Fong K. Mental health of staff working in intensive care during Covid-19. Occup Med (Lond) [Internet]. 2021 Apr 9 [cited 2021 Jul 6];71(2):62–7. Available from: https://www.limesurvey.org/
- Lasalvia A, Amaddeo F, Porru S, Carta A, Tardivo S, Bovo C, et al. Levels of burn-out among healthcare workers during the COVID-19 pandemic and their associated factors: A cross-sectional study in a tertiary hospital of a highly burdened area of north-east Italy. BMJ Open [Internet]. 2021 Jan 17 [cited 2021 Jul 6];11(1). Available from: https://pubmed.ncbi.nlm.nih.gov/33455940/
- Greenberg N, Weston D, Hall C, Caulfield T, Williamson V, Fong K. Mental health of staff working in intensive care during Covid-19. Occup Med (Chic Ill) [Internet]. 2021 Apr 9 [cited 2025 Aug 5];71(2):62–7. Available from: https://dx.doi.org/10.1093/occmed/kqaa220
- Sunjaya DK, Herawati DMD, Siregar AY. Depressive , Anxiety , and Burnout Symptoms on Health Care Personnel at a Month After COVID-19 Outbreak in Indonesia : A Documentary Research Using Rasch Model Analysis. Res Sq. 2020;1–13.
- de Diego-Cordero R, Ávila-Mantilla A, Vega-Escaño J, Lucchetti G, Badanta B. The Role of Spirituality and Religiosity in Healthcare During the COVID-19 Pandemic: An Integrative Review of the Scientific Literature. J Relig Health [Internet]. 2022 Jun 1 [cited 2025 Aug 29];61(3):2168. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC8960681
- Putri P, Maurida N, Novitasari F, Rosalini W, Elyas M, Budiman A, et al. Workplace Spirituality with Nurse Anxiety During The Covid 19 Pandemic in Indonesia. 2021 [cited 2025 Aug 29];15(10). Available from: https://doi.org/10.53350/pjmhs2115103204
- Lyon TR, Galbraith A. Mindful Self-Compassion as an Antidote to Burnout for Mental Health Practitioners. Healthc 2023, Vol 11, Page 2715 [Internet]. 2023 Oct 12 [cited 2025 Aug 29];11(20):2715. Available from: https://www.mdpi.com/2227-9032/11/20/2715/htm
- Kim S, Crawford J, Hunter S. Role of an Online Skill-Based Mindfulness Program for Healthcare Worker’s Resiliency During the COVID-19 Pandemic: A Mixed-Method Study. Front Public Heal [Internet]. 2022 Jul 14 [cited 2025 Aug 29];10:907528. Available from: www.frontiersin.org
- Adair KC, Powell M, Sexton JB. Bite-sized self-compassion: a pilot cohort study of a well-being tool for healthcare workers. Sci Rep [Internet]. 2025 Dec 1 [cited 2025 Aug 29];15(1):30271. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC12361568/
- Sunjaya DK, Herawati DMD, Siregar AYM. Depressive, anxiety, and burnout symptoms on health care personnel at a month after COVID-19 outbreak in Indonesia. BMC Public Health. 2021;21(1):1–12.
- Liu CY, Yang YZ, Zhang XM, Xu X, Dou QL, Zhang WW, et al. The prevalence and influencing factors in anxiety in medical workers fighting COVID-19 in China: A cross-sectional survey [Internet]. Vol. 148, Epidemiology and Infection. Cambridge University Press; 2020 [cited 2022 Oct 14]. p. e98. Available from: https://www.cambridge.org/core/journals/epidemiology-and-infection/article/prevalence-and-influencing-factors-in-anxiety-in-medical-workers-fighting-covid19-in-china-a-crosssectional-survey/D493886C34C350A01D3D0501AC89B9CB
- Sunil R, Bhatt MT, Bhumika TV, Thomas N, Puranik A, Chaudhuri S, et al. Weathering the storm: Psychological impact of covid-19 pandemic on clinical and nonclinical healthcare workers in india. Indian J Crit Care Med. 2021;25(1):16–20.
- Chanchalani G, Arora N, Nasa P, Sodhi K, Bahrani MJA, Tayar A Al, et al. Visiting and Communication Policy in Intensive Care Units during COVID-19 Pandemic: A Cross-sectional Survey from South Asia and the Middle East. Indian J Crit Care Med. 2022;26(3):268–75.
- Collins C, Mahuron K, Bongiovanni T, Lancaster E, Sosa JA, Wick E. Stress and the Surgical Resident in the COVID-19 Pandemic. J Surg Educ [Internet]. 2021;78(2):422–30. Available from: https://doi.org/10.1016/j.jsurg.2020.07.031
- Luceño-Moreno L, Talavera-Velasco B, García-Albuerne Y, Martín-García J. Symptoms of posttraumatic stress, anxiety, depression, levels of resilience and burnout in spanish health personnel during the COVID-19 pandemic. Int J Environ Res Public Health [Internet]. 2020 Jul 30 [cited 2022 Oct 17];17(15):1–29. Available from: https://www.mdpi.com/1660-4601/17/15/5514/htm
- Elghazally SA, Alkarn AF, Elkhayat H, Ibrahim AK, Elkhayat MR. Burnout impact of covid-19 pandemic on health-care professionals at Assiut University Hospitals, 2020. Int J Environ Res Public Health. 2021;18(10):5368.
- Muhammad Alfareed Zafar S, Junaid Tahir M, Malik M, Irfan Malik M, Kamal Akhtar F, Ghazala R. Awareness, anxiety, and depression in healthcare professionals, medical students, and general population of Pakistan during COVID-19 Pandemic: A cross sectional online survey. Med J Islam Repub Iran [Internet]. 2020;2020. Available from: http://mjiri.iums.ac.ir34.131.https//doi.org/10.47176/mjiri.34.131
- Hawes MT, Szenczy AK, Klein DN, Hajcak G, Nelson BD. Increases in Depression and Anxiety Symptoms in Adolescents and Young Adults during the COVID-19 Pandemic. Psychol Med [Internet]. 2021 [cited 2022 Mar 3];1–9. Available from: https://www.cambridge.org/core/journals/psychological-medicine/article/increases-in-depression-and-anxiety-symptoms-in-adolescents-and-young-adults-during-the-covid19-pandemic/F10C068F4D7A7AEDF2699A517904C1EB
- Al-Humadi S, Bronson B, Muhlrad S, Paulus M, Hong H, Cáceda R. Depression, Suicidal Thoughts, and Burnout Among Physicians During the COVID-19 Pandemic: a Survey-Based Cross-Sectional Study. Acad Psychiatry. 2021;45(5):557–65.
- Hashem Z, Zeinoun P. Self-Compassion Explains Less Burnout Among Healthcare Professionals. Mindfulness (N Y) [Internet]. 2020;11(11):2542–51. Available from: https://doi.org/10.1007/s12671-020-01469-5
- Kavaklı M, Ak M, Uğuz F, Türkmen OO. The mediating role of self-compassion in the relationship between perceived COVID-19 threat and death anxiety. Klin Psikiyatr Derg. 2020;23:15–23.
- Rushing CJ, Casciato DJ, Ead JK, Spinner SM. Perceptions of Burnout, Personal Achievement, and Anxiety Among US Podiatric Medicine and Surgery Residents: A Cross-Sectional Pilot Study. J Foot Ankle Surg. 2020;59(5):953–6.
- Ruiz-Fernández MD, Ramos-Pichardo JD, Ibáñez-Masero O, Cabrera-Troya J, Carmona-Rega MI, Ortega-Galán ÁM. Compassion fatigue, burnout, compassion satisfaction and perceived stress in healthcare professionals during the COVID-19 health crisis in Spain. J Clin Nurs. 2020;29(21–22):4321–30.