Eka Satrio Putra 1 , Rachmatria Luthfiani Khaerunnissya 2
Authors affiliations:
Expanded Dengue Syndrome (EDS) can cause severe multi-organ involvement, especially in geriatric patients. This report details a 91-year-old woman whose dengue fever progressed to shock and EDS, affecting multiple organs. Hemodynamic instability prompted Sustained Low-Efficiency Dialysis (SLED) for Acute Kidney Injury (AKI), which provided renal support without further compromise. Intravenous Immunoglobulin (IVIG) was also administered. The patient improved, with stabilized hemodynamics and resolved organ dysfunction, leading to discharge without sequelae. This case report is of utmost importance as it highlights the potential utility of SLED and IVIG in managing complex EDS in geriatric patients. However, further research is needed to establish standardized protocols for management of EDS.
Abbreviations: AKI: Acute Kidney Injury, EDS: Expanded Dengue Syndrome, IVIG: Intravenous Immunoglobulin, SLED: Sustained Low-Efficiency Dialysis
Keywords: Expanded dengue syndrome; Geriatric; Sustained low-efficiency dialysis; Intravenous immunoglobulin; Multi-organ involvement
Citation: Putra ES, Khaerunnissya RL. Sustained low-efficiency dialysis and intravenous immunoglobulin in geriatric expanded dengue syndrome: A case study. Anaesth. pain intensive care 2025;29(8):1032-1036. DOI: 10.35975/apic.v29i8.3035
Received: May 17, 2025; Revised: August 26, 2025; Accepted: September 04, 2025
Dengue is currently the fastest-growing mosquito-borne viral disease worldwide. The clinical presentation of dengue varies widely, ranging from cases with no symptoms to severe forms such as dengue shock syndrome, which is characterized by critical plasma leakage.1 Furthermore, it may also present with uncommon clinical presentations defined as expanded dengue syndrome.1
The World Health Organization (WHO) introduced the term EDS in 2011 to describe rare dengue manifestations involving serious injury to organs such as the liver, kidneys, bone marrow, heart, brain, and other isolated organ involvement. Geriatric, pregnant women, infants, and individuals with chronic diseases are particularly vulnerable to developing EDS.1 The prevalence of dengue–related Acute Kidney Injury (AKI) varies between 0.9-13.3% depending on the definition of AKI, age group, and severity.2 14.1% of dengue-related AKI require dialysis. The rate of need for dialysis increases up to 70% in patients with severe dengue admitted to the ICU. AKI is linked to prolonged hospitalization and increased mortality in dengue cases.2
Besides ensuring proper fluid therapy and avoiding nephrotoxic medications, there is currently no specific management for dengue-related AKI. RRT may become essential in some cases, particularly AKI with the presence of persistent uremia and hypercatabolism, hyperkalemia, hypervolemia, and metabolic acidosis. However, conventional intermittent hemodialysis may carry a significant risk of further hemodynamic deterioration in patients with unstable hemodynamics.2 The KDIGO 2012 guideline moderately recommends continuous renal replacement therapy (CRRT) over IHD for acute kidney injury (AKI) with hemodynamic instability. Still, it acknowledges sustained low-efficiency dialysis (SLED) as a viable alternative.3 SLED delivers renal replacement therapy over an extended period with lower solute clearance and ultrafiltration rates than IHD, aiming to combine CRRT’s hemodynamic stability with IHD’s efficacy.3
The pathophysiology of severe and atypical dengue presentations remains unclear but it is thought to involve both direct viral effects and immune-mediated damage to various organs.4 The immune-related mechanisms underlying the atypical and severe presentations of dengue, along with the potential positive immunomodulatory effects of intravenous immunoglobulins (IVIG), indicate that this treatment might have a role in managing the disease.5 An observational study in India demonstrated that IVIG can be used as rescue therapy in critically ill patients with complicated dengue.6 However, there was a conflicting result from another study showing IVIG is ineffective in treating selected dengue cases.7 The available evidence is quite limited, highlighting the need for well-structured randomized controlled trials to explore the potential benefits of IVIG in treating the severe and life-threatening complications of dengue.5 We report such a complicated, multi-organ involvement in geriatric patient with expanded dengue syndrome receiving SLED and IVIG therapy.
A 91-year-old woman presented with a sudden onset of fever, joint pain, anorexia, and moderate abdominal pain. There were no hemorrhagic manifestations. Past illness includes congestive heart failure (decreased left ventricular contractility with global hypokinesis and an ejection fraction of 31%), controlled with medications. Upon physical examination, vitals were stable except for elevated temperature. There was an epigastric and a slight upper right quadrant tenderness, bowel sound was normal, liver was not palpable, and other examinations were unremarkable. Complete blood counts were within normal limits, and an NS-1 test was conducted with a positive result. She was initially diagnosed to have dengue fever, and fluid management was done with a maintenance rate to avoid volume overload.
Within 12 hours of presentation, she had a decreased level of consciousness with abdominal distension, hyperactive bowel sound, and hematuria. Vitals were unstable with signs of shock. Fluid resuscitation was carried out along with blood product transfusion, but she was unresponsive to them. Norepinephrine was required to maintain her blood pressure. Abdominal X-ray showed a suggestive finding of paralytic ileus (Figure I). She was assessed for dengue shock syndrome and was transferred to the intensive care unit.
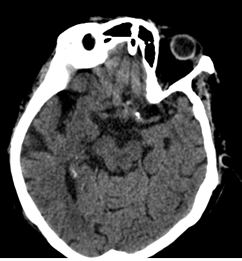
Figure 1: CT scan of head shows multiple cerebral infarction areas
On day 3 of hospitalization, the level of consciousness continued to decline; she was anuric for 6 hours with a sudden, almost four-times increase of serum creatinine and urea, and a ten-times increase of liver function tests. She was suspected of having expanded dengue syndrome with intestinal, liver, and kidney involvement. Given her unstable hemodynamics, which carried a significant risk of further decline in hemodynamics during conventional hemodialysis, a SLED was performed, with a blood flow rate of 200 mL/ minute, dialysate flow rate of 250 mL/ minute, and 8 hours of total duration. A re-evaluation of serum urea and creatinine was done with a half-time decline. 12 hours after undergoing SLED, she had severe dyspnea. Arterial blood gas analysis was carried out due to acute hypoxemic respiratory failure. She had to put on mechanical ventilation. A satisfactory blood gas analysis result was seen on re-evaluation after 2 hours. Lung involvement was likely, and considering a wide range of organ involvement, an intravenous immunoglobulin was started at 0.5 g/kg given daily.
On day 4 of hospitalization, sedation was weaned off, but an increase in the level of consciousness was not observed. Upon neurological examination, there was nystagmus and vertical gaze palsy. A non-contrast head CT scan was performed, with a result of an infarct (Figure 1). Hemodynamic parameters gradually improved, with a decreased need for norepinephrine dose required to maintain blood pressure.
On day 5 of hospitalization, her level of consciousness gradually increased. Her hemodynamics remained stable using only a minimal dose of norepinephrine. The next day, she was extubated and transferred from the intensive care unit to a regular ward. SLED and IVIG were discontinued. Her condition continuously improved, and she was discharged home after 14 days of hospitalization with no significant residual sequelae.
As dengue infections spread geographically, there has been a rise in reports of dengue with atypical presentations coined by the WHO as expanded dengue syndrome.1 Despite being uncommon, EDS exhibits a wide range of symptoms that need to be thoroughly studied to enable prompt identification and start targeted therapy. Our case presented a multifaceted organ involvement in a woman with dengue infection.
Numerous studies have assessed different factors related to atypical or severe presentation of dengue, including secondary infection, viral strain, and advanced age (> 65 years). The geriatric population is prone to developing severe dengue signs, likely because of the presence of other comorbidities such as cardiovascular diseases, diabetes mellitus, and chronic kidney disease.4 Our patient was 91 years old, with a history of congestive heart failure; thus, a severe presentation was very likely.
Acute Kidney Injury (AKI) is the most common renal issue in expanded dengue syndrome, with mechanisms including shock-induced hypotension, direct viral damage, immune responses, and rhabdomyolysis.2 Dialysis method selection depends on the patient's condition and hemodynamic stability. Dengue-related AKI often occurs with unstable hemodynamics, making conventional intermittent dialysis risky.2,8
Continuous Renal Replacement Therapy (CRRT) is better tolerated in unstable patients but is complex and costly. Sustained Low-Efficiency Dialysis (SLED), a hybrid modality, offers hemodynamic stability and effective solute clearance using slower flow rates over xtended sessions, unlike conventional IHD.8 Studies show SLED is a feasible alternative to CRRT for critically ill, hemodynamically unstable patients requiring dialysis, with comparable safety and efficacy.8,9 In our center, where CRRT was unavailable, SLED was successfully used for 8-hour sessions over three days without causing hemodynamic deterioration
Severe dengue presentation is characterized by immune system dysregulation, leading to vascular endothelial damage, increased capillary permeability, and thrombocytopenia. These effects arise from cytokine-mediated pathways involving tumor necrosis factor-α (TNF-α), interleukin-1 (IL-1), interleukin-6 (IL-6), and interferon gamma (IFN-γ), which disrupt endothelial cell function. Additionally, the dengue virus's non-structural protein 1 (NS1) exacerbates vascular leakage by interacting with Toll-like receptor 4 (TLR4) on immune cells, further compromising endothelial integrity. Specific organ damage-including kidney and hepatic injury, myositis, neurological impairment, and cardiac involvement-results from both direct viral effects and immune-driven processes such as cytokine storms. Antibody-dependent enhancement (ADE), where preexisting antibodies facilitate viral entry into host cells, also contributes to severe manifestations by amplifying immune activation and vascular dysfunction. The management of atypical and severe dengue presentations is largely supportive with careful fluid therapy. There is no current guideline that recommend specific therapy in multiorgan involvement in expanded dengue syndrome.4
cytokine cascade triggered by the dengue virus. It also promotes the production of the anti-inflammatory cytokine IL-1 receptor antagonist (IL-1ra). Additionally, IVIG prevents the formation of the complement membrane attack complex (C5b-9) by neutralizing activated complement components. These immune-regulating effects of IVIG may provide therapeutic benefits by modulating the disrupted immune response seen in severe presentations of dengue.5,6 Our patient experienced a refractory shock with multiorgan involvement. IVIG was initiated to reduce inflammatory responses and capillary leakage, thus enhancing the patient's overall clinical status.
Some studies have shown the benefit of IVIG in particular cases of dengue. A case series in Brazil involved five patients with dengue and severe thrombocytopenia who were treated with IVIG at a dose of 500 mg/kg per day, administered over 3-hour infusions for 5 days. This treatment led to both clinical
improvement and an increase in the platelet counts.10 An observational study in India involving 13 critically ill dengue patients, 9 with refractory shock, 2 with encephalitis, and 2 with HLH, that received IVIG therapy concluded that IVIG can be used as rescue therapy in critically ill patients with complicated dengue.6 However, a conflicting result came from a randomized controlled trial (RCT) conducted by Dimaano et al. evaluating the effect of IVIG on thrombocytopenia in dengue patients, which showed no benefit of IVIG treatment in accelerating platelet recovery. However, critically ill patients were not involved in this study.7 Since the efficacy of IVIG in
We successfully managed a geriatric patient with expanded dengue syndrome using sustained low-efficiency dialysis and intravenous immunoglobulins. While intravenous immunoglobulins have shown effectiveness in certain cases, their use has been limited to a small number of patients, reinforcing the need for further studies and standard treatment protocols.
6. Conflict of interest
All authors declare that there was no conflict of interest.
7. Funding
The study utilized the hospital resources only, and no external or industry funding was involved.
8. Authors’ contribution
ESP: attending physician, conduction of the study work, manuscript editing
RLK: conduction of the study work, manuscript editing
Authors affiliations:
- Eka Satrio Putra, 45 General Hospital, Kuningan, West Java, Indonesia; Email: ekasatrio@gmail.com; {ORCID:0000-0002-8906-0012}
- Rachmatria Luthfiani Khaerunnissya, 45 General Hospital, Kuningan, West Java, Indonesia; Email: luthfianirachmatria@gmail.com; {ORCID:0009-0005-1353-7020}
ABSTRACT
Expanded Dengue Syndrome (EDS) can cause severe multi-organ involvement, especially in geriatric patients. This report details a 91-year-old woman whose dengue fever progressed to shock and EDS, affecting multiple organs. Hemodynamic instability prompted Sustained Low-Efficiency Dialysis (SLED) for Acute Kidney Injury (AKI), which provided renal support without further compromise. Intravenous Immunoglobulin (IVIG) was also administered. The patient improved, with stabilized hemodynamics and resolved organ dysfunction, leading to discharge without sequelae. This case report is of utmost importance as it highlights the potential utility of SLED and IVIG in managing complex EDS in geriatric patients. However, further research is needed to establish standardized protocols for management of EDS.
Abbreviations: AKI: Acute Kidney Injury, EDS: Expanded Dengue Syndrome, IVIG: Intravenous Immunoglobulin, SLED: Sustained Low-Efficiency Dialysis
Keywords: Expanded dengue syndrome; Geriatric; Sustained low-efficiency dialysis; Intravenous immunoglobulin; Multi-organ involvement
Citation: Putra ES, Khaerunnissya RL. Sustained low-efficiency dialysis and intravenous immunoglobulin in geriatric expanded dengue syndrome: A case study. Anaesth. pain intensive care 2025;29(8):1032-1036. DOI: 10.35975/apic.v29i8.3035
Received: May 17, 2025; Revised: August 26, 2025; Accepted: September 04, 2025
1. INTRODUCTION
Dengue is currently the fastest-growing mosquito-borne viral disease worldwide. The clinical presentation of dengue varies widely, ranging from cases with no symptoms to severe forms such as dengue shock syndrome, which is characterized by critical plasma leakage.1 Furthermore, it may also present with uncommon clinical presentations defined as expanded dengue syndrome.1
The World Health Organization (WHO) introduced the term EDS in 2011 to describe rare dengue manifestations involving serious injury to organs such as the liver, kidneys, bone marrow, heart, brain, and other isolated organ involvement. Geriatric, pregnant women, infants, and individuals with chronic diseases are particularly vulnerable to developing EDS.1 The prevalence of dengue–related Acute Kidney Injury (AKI) varies between 0.9-13.3% depending on the definition of AKI, age group, and severity.2 14.1% of dengue-related AKI require dialysis. The rate of need for dialysis increases up to 70% in patients with severe dengue admitted to the ICU. AKI is linked to prolonged hospitalization and increased mortality in dengue cases.2
Besides ensuring proper fluid therapy and avoiding nephrotoxic medications, there is currently no specific management for dengue-related AKI. RRT may become essential in some cases, particularly AKI with the presence of persistent uremia and hypercatabolism, hyperkalemia, hypervolemia, and metabolic acidosis. However, conventional intermittent hemodialysis may carry a significant risk of further hemodynamic deterioration in patients with unstable hemodynamics.2 The KDIGO 2012 guideline moderately recommends continuous renal replacement therapy (CRRT) over IHD for acute kidney injury (AKI) with hemodynamic instability. Still, it acknowledges sustained low-efficiency dialysis (SLED) as a viable alternative.3 SLED delivers renal replacement therapy over an extended period with lower solute clearance and ultrafiltration rates than IHD, aiming to combine CRRT’s hemodynamic stability with IHD’s efficacy.3
The pathophysiology of severe and atypical dengue presentations remains unclear but it is thought to involve both direct viral effects and immune-mediated damage to various organs.4 The immune-related mechanisms underlying the atypical and severe presentations of dengue, along with the potential positive immunomodulatory effects of intravenous immunoglobulins (IVIG), indicate that this treatment might have a role in managing the disease.5 An observational study in India demonstrated that IVIG can be used as rescue therapy in critically ill patients with complicated dengue.6 However, there was a conflicting result from another study showing IVIG is ineffective in treating selected dengue cases.7 The available evidence is quite limited, highlighting the need for well-structured randomized controlled trials to explore the potential benefits of IVIG in treating the severe and life-threatening complications of dengue.5 We report such a complicated, multi-organ involvement in geriatric patient with expanded dengue syndrome receiving SLED and IVIG therapy.
2. CASE PRESENTATION
A 91-year-old woman presented with a sudden onset of fever, joint pain, anorexia, and moderate abdominal pain. There were no hemorrhagic manifestations. Past illness includes congestive heart failure (decreased left ventricular contractility with global hypokinesis and an ejection fraction of 31%), controlled with medications. Upon physical examination, vitals were stable except for elevated temperature. There was an epigastric and a slight upper right quadrant tenderness, bowel sound was normal, liver was not palpable, and other examinations were unremarkable. Complete blood counts were within normal limits, and an NS-1 test was conducted with a positive result. She was initially diagnosed to have dengue fever, and fluid management was done with a maintenance rate to avoid volume overload.
Within 12 hours of presentation, she had a decreased level of consciousness with abdominal distension, hyperactive bowel sound, and hematuria. Vitals were unstable with signs of shock. Fluid resuscitation was carried out along with blood product transfusion, but she was unresponsive to them. Norepinephrine was required to maintain her blood pressure. Abdominal X-ray showed a suggestive finding of paralytic ileus (Figure I). She was assessed for dengue shock syndrome and was transferred to the intensive care unit.

Figure 1: CT scan of head shows multiple cerebral infarction areas
On day 3 of hospitalization, the level of consciousness continued to decline; she was anuric for 6 hours with a sudden, almost four-times increase of serum creatinine and urea, and a ten-times increase of liver function tests. She was suspected of having expanded dengue syndrome with intestinal, liver, and kidney involvement. Given her unstable hemodynamics, which carried a significant risk of further decline in hemodynamics during conventional hemodialysis, a SLED was performed, with a blood flow rate of 200 mL/ minute, dialysate flow rate of 250 mL/ minute, and 8 hours of total duration. A re-evaluation of serum urea and creatinine was done with a half-time decline. 12 hours after undergoing SLED, she had severe dyspnea. Arterial blood gas analysis was carried out due to acute hypoxemic respiratory failure. She had to put on mechanical ventilation. A satisfactory blood gas analysis result was seen on re-evaluation after 2 hours. Lung involvement was likely, and considering a wide range of organ involvement, an intravenous immunoglobulin was started at 0.5 g/kg given daily.
On day 4 of hospitalization, sedation was weaned off, but an increase in the level of consciousness was not observed. Upon neurological examination, there was nystagmus and vertical gaze palsy. A non-contrast head CT scan was performed, with a result of an infarct (Figure 1). Hemodynamic parameters gradually improved, with a decreased need for norepinephrine dose required to maintain blood pressure.
On day 5 of hospitalization, her level of consciousness gradually increased. Her hemodynamics remained stable using only a minimal dose of norepinephrine. The next day, she was extubated and transferred from the intensive care unit to a regular ward. SLED and IVIG were discontinued. Her condition continuously improved, and she was discharged home after 14 days of hospitalization with no significant residual sequelae.
3. DISCUSSION
As dengue infections spread geographically, there has been a rise in reports of dengue with atypical presentations coined by the WHO as expanded dengue syndrome.1 Despite being uncommon, EDS exhibits a wide range of symptoms that need to be thoroughly studied to enable prompt identification and start targeted therapy. Our case presented a multifaceted organ involvement in a woman with dengue infection.
Numerous studies have assessed different factors related to atypical or severe presentation of dengue, including secondary infection, viral strain, and advanced age (> 65 years). The geriatric population is prone to developing severe dengue signs, likely because of the presence of other comorbidities such as cardiovascular diseases, diabetes mellitus, and chronic kidney disease.4 Our patient was 91 years old, with a history of congestive heart failure; thus, a severe presentation was very likely.
Acute Kidney Injury (AKI) is the most common renal issue in expanded dengue syndrome, with mechanisms including shock-induced hypotension, direct viral damage, immune responses, and rhabdomyolysis.2 Dialysis method selection depends on the patient's condition and hemodynamic stability. Dengue-related AKI often occurs with unstable hemodynamics, making conventional intermittent dialysis risky.2,8
Continuous Renal Replacement Therapy (CRRT) is better tolerated in unstable patients but is complex and costly. Sustained Low-Efficiency Dialysis (SLED), a hybrid modality, offers hemodynamic stability and effective solute clearance using slower flow rates over xtended sessions, unlike conventional IHD.8 Studies show SLED is a feasible alternative to CRRT for critically ill, hemodynamically unstable patients requiring dialysis, with comparable safety and efficacy.8,9 In our center, where CRRT was unavailable, SLED was successfully used for 8-hour sessions over three days without causing hemodynamic deterioration
Severe dengue presentation is characterized by immune system dysregulation, leading to vascular endothelial damage, increased capillary permeability, and thrombocytopenia. These effects arise from cytokine-mediated pathways involving tumor necrosis factor-α (TNF-α), interleukin-1 (IL-1), interleukin-6 (IL-6), and interferon gamma (IFN-γ), which disrupt endothelial cell function. Additionally, the dengue virus's non-structural protein 1 (NS1) exacerbates vascular leakage by interacting with Toll-like receptor 4 (TLR4) on immune cells, further compromising endothelial integrity. Specific organ damage-including kidney and hepatic injury, myositis, neurological impairment, and cardiac involvement-results from both direct viral effects and immune-driven processes such as cytokine storms. Antibody-dependent enhancement (ADE), where preexisting antibodies facilitate viral entry into host cells, also contributes to severe manifestations by amplifying immune activation and vascular dysfunction. The management of atypical and severe dengue presentations is largely supportive with careful fluid therapy. There is no current guideline that recommend specific therapy in multiorgan involvement in expanded dengue syndrome.4
cytokine cascade triggered by the dengue virus. It also promotes the production of the anti-inflammatory cytokine IL-1 receptor antagonist (IL-1ra). Additionally, IVIG prevents the formation of the complement membrane attack complex (C5b-9) by neutralizing activated complement components. These immune-regulating effects of IVIG may provide therapeutic benefits by modulating the disrupted immune response seen in severe presentations of dengue.5,6 Our patient experienced a refractory shock with multiorgan involvement. IVIG was initiated to reduce inflammatory responses and capillary leakage, thus enhancing the patient's overall clinical status.
Some studies have shown the benefit of IVIG in particular cases of dengue. A case series in Brazil involved five patients with dengue and severe thrombocytopenia who were treated with IVIG at a dose of 500 mg/kg per day, administered over 3-hour infusions for 5 days. This treatment led to both clinical
improvement and an increase in the platelet counts.10 An observational study in India involving 13 critically ill dengue patients, 9 with refractory shock, 2 with encephalitis, and 2 with HLH, that received IVIG therapy concluded that IVIG can be used as rescue therapy in critically ill patients with complicated dengue.6 However, a conflicting result came from a randomized controlled trial (RCT) conducted by Dimaano et al. evaluating the effect of IVIG on thrombocytopenia in dengue patients, which showed no benefit of IVIG treatment in accelerating platelet recovery. However, critically ill patients were not involved in this study.7 Since the efficacy of IVIG in
| vTable 1: Summary of key events, laboratory profile, imaging studies, and associated managements | |||
| Day | Physical Findings / Key Events | CBC | Other Laboratory and Imaging Profile |
| Day 1 | Features of classic dengue fever 1-day sudden onset of fever, joint pain, anorexia, abdominal pain Ringer’s Acetate Solution with maintenance rate (2000 mL in 24 hours) |
Hb 12.2 Ht 35 L 6.399 Tr 124.000 |
Ur 58 Cr 1.4 NS-1 : Positive |
| Day 2 | Decreased level of consciousness with features of paralytic ileus (distended abdomen and decreased bowel sound), hematuria, followed by shock Fluid resuscitation (Ringer’s Acetate Solution 20 mL/kg within 30 minutes) PRC Transfusion Persistent shock continued despite fluid resuscitation and administration of blood product Norepinephrine started 0.6 mcg/kg/min and was titrated according to the response |
Hb 8.7 Ht 24.6 L 9.900 Tr 86.000 |
Abdominal X-ray: suggestive finding of ileus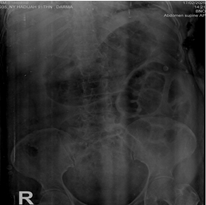 |
| Day 3 | Features of AKI, liver involvement, unstable hemodynamic (maintained by norepinephrine 0.3 mcg/kg/min) SLED Acute Respiratory Failure Endotracheal intubation and mechanical ventilation / IVIG was started (0.5 g/kg daily) |
Pre-SLED
Hb 10.5 Ht 30.0 L 9.200 Tr 80.000 Post-SLED Hb 11.2 Ht 32.2 L 12.000 Tr 110.000 |
Pre-SLED
Ur 218; Cr 5.4; SGOT 409; SGPT 349 Post-SLED Ur 139; Cr 2.7; SGOT 95; SGPT 106 Blood gas analysis pH 7.448; pO2 52 mmHg; pCO2 19.3 mmHg; Base Deficit -11 mmol/L; HCO3 13.4 mmol/L; Lactate 4.2 mmol/L; SO2 89% Post mechanical ventilation pH 7.454; O2 144 mmHg; pCO2 25.2 mmHg; Base Deficit -6 mmol/L; HCO3 17.6 mmol/L Lactate 3.9 mmol/L; SO2 99% |
| Day 4 | Sedation weaned off LoC not improving, nystagmus and vertical gaze palsy Hemodynamic continued improving, norepinephrine 0.1 mcg/kg/min SLED and IVIG continued |
Hb 9.7 Ht 26.2 L 13.400 Tr 133.000 |
Non-contrast head CT-scan: infarct at mesencephalon Pre-SLED Ur 207; Cr 5.0 Post-SLED Ur 121; Cr 2.8 |
| Day 5 | Gradual increase of LoC, ventilation weaned off Soft abdomen, normal bowel sound Stable hemodynamic, norepinephrine on minimal dose (0.05 mcg/kg/min) SLED and IVIG continued |
Hb 10.1 Ht 28.9 L 12.000 Tr 273.000 |
Blood gas analysis
pH 7.481; pO2 121 mmHg; pCO2 32.6 mmHg Base Excess 1 mmol/L; HCO3 24.4; Lactate 1.8 mmol/L; SO2 99% Pre-SLED Ur 218; Cr 4.8 Post-SLED Ur 242; Cr 2.4 |
| Day 6 | Extubation Stable hemodynamics without vasopressor SLED and IVIG discontinued |
Hb 10.6 Ht 31.2 L 12.300 Tr 362.000 |
Ur 85; r 2.4 |
| Footnotes: Hb = Hemoglobin; Ht = Hematocrit; L = Leukosit; Tr = Trombosit; Ur = Ureum; Cr = Creatinine; SLED = Sustained Low-Efficiency Dialysis; IVIG = Intravenous Immunoglobulin | |||
5. CONCLUSION
We successfully managed a geriatric patient with expanded dengue syndrome using sustained low-efficiency dialysis and intravenous immunoglobulins. While intravenous immunoglobulins have shown effectiveness in certain cases, their use has been limited to a small number of patients, reinforcing the need for further studies and standard treatment protocols.
6. Conflict of interest
All authors declare that there was no conflict of interest.
7. Funding
The study utilized the hospital resources only, and no external or industry funding was involved.
8. Authors’ contribution
ESP: attending physician, conduction of the study work, manuscript editing
RLK: conduction of the study work, manuscript editing
9. REFERENCES
- World Health Organization. Comprehensive Guideline for Prevention and Control of Dengue and Dengue Haemorrhagic Fever [Internet]. 2011. [cited 2025 May 9]. Available from: https://iris.who.int/handle/10665/204894
- Bignardi PR, Pinto GR, Letícia M, Boscarioli N, Lima RAA, Delfino VDA. Acute kidney injury associated with dengue virus infection: a review Injúria renal aguda associada à infecção pelo vírus da dengue: uma revisão. 2021; PMCID: PMC11210537 DOI: 10.1590/2175-8239-JBN-2022-0150eren
- Vicente R, Santos R, Coelho S. The Role of Sustained Low-Efficiency Dialysis (SLED) in the Intensive Care Unit. Port J Nephrol Hypert [Internet]. 2022;36(x).
- Tejo AM, Hamasaki DT, Menezes LM, Ho YL. Severe dengue in the intensive care unit. J Intensive Med 2023 Sep 28;4(1):16-33. PMCID: PMC10800775 DOI: 10.1016/j.jointm.2023.07.007
- Rajapakse S. Intravenous immunoglobulins in the treatment of dengue illness. Trans R Soc Trop Med Hyg 2009 Sep;103(9):867-70. DOI: 10.1016/j.trstmh.2008.12.011
- Padmaprakash K V., Jha VK, Sowmya Karantha C, Anurag Singh C, Kamal D, Jambunathan P. Rescue therapy with intravenous immunoglobulin in severe refractory dengue: A pilot study. Med J Armed Forces India. 2022 Apr 1;78(2):204–12. PMCID: PMC9023533 DOI: 10.1016/j.mjafi.2020.12.036
- Dimaano EM, Saito M, Honda S, Miranda EA, Alonzo MTG, Valerio MD, et al. Lack of Efficacy of High-Dose Intravenous Immunoglobulin Treatment of Severe Thrombocytopenia in Patients with Secondary Dengue Virus Infection. Am J Trop Med Hyg [Internet]. 2007 Dec 1 [cited 2025 May 5];77(6):1135–8. Available from: https://www.ajtmh.org/view/journals/tpmd/77/6/article-p1135.xmL
- Sharieff S, Rafai W, Manzoor A, Idrees A, Ahmad B, Ghulam M, et al. Experience of Sustained Low-Efficiency Dialysis (SLED) in an Intensive Care Unit of a Quaternary Care Hospital. Cureus. 2024 Feb 18; doi: 10.7759/cureus.70789.
- Al Dalbhi S, Alorf R, Alotaibi M, Altheaby A, Alghamdi Y, Ghazal H, et al. Sustained low efficiency dialysis is non-inferior to continuous renal replacement therapy in critically ill patients with acute kidney injury: A comparative meta-analysis. Vol. 100, Medicine (United States). Lippincott Williams and Wilkins; 2021. p. E28118.
- Ostronoff M, Ostronoff F, Florêncio R, Florêncio M, Domingues MC, Calixto R, et al. Serious thrombocytopenia due to dengue hemorrhagic fever treated with high dosages of immunoglobulin [1]. Clinical Infectious Diseases [Internet]. 2003 Jun 15 [cited 2025 May 5];36(12):1623–4. Available from: https://dx.doi.org/10.1086/374870