Muhammad Omer Afzal Bhatti 1 , Mujeeb Ur Rehman Parrey 2 , Pakeeza Shafiq 3 , Maha M. Abdul-Latif 4 , Haider Osman Elmisbah 5
Authors affiliations:
Background and objective: Radiology plays a vital role in modern medicine, yet many new graduates face challenges in selecting the appropriate imaging studies and interpreting their findings. This study seeks to examine medical students’ perspectives on their undergraduate radiology curriculum in order to identify existing gaps and suggest areas for improvement.
Methodology: This mixed-methods study, conducted at the Faculty of Medicine, Northern Border University, from November 2024 to March 2025, used a structured questionnaire with quantitative and open-ended questions. A convenience sample of 150 students from the 3rd, 4th, 5th, and 6th years participated.
Results: The majority of students agreed or strongly agreed that the curriculum was effective (P < 0.001). However, they noted limited radiology integration in preclinical years, though it improved in clinical years (P = 0.041). A hundred percent of students agreed that hands-on training was lacking. The most preferred educational methods were lectures (96.7%) and case-based learning (94%). Notably, 98% of students believe radiology should be introduced earlier, and 93% were interested in more learning opportunities.
Conclusion: Students highlighted that better integration of radiology in both preclinical and clinical settings would boost their confidence and preparedness for clinical practice. They strongly recommended hands-on and case-based sessions to improve education and emphasized the need to focus on foundational radiology knowledge at the undergraduate level.
Abbreviations: ESR: European Society of Radiology, OSCE: Objective Structured Clinical Examinations
Keywords: Clinical Practice; Curriculum Enhancement; Medical Education; Mixed-methods study; Radiology
Citation: Bhatti MOA, Parrey MUR, Shafiq P, Abdul-Latif MM, Elmisbah HO. Bridging the gaps: medical students' perspectives on undergraduate radiology education and curriculum enhancement. Anaesth. pain intensive care 2025;29(8):955-961. DOI: 10.35975/apic.v29i8.3024
Received: August 25, 2025; Revised: August 29, 2025; Accepted: September 01, 2025
Radiology's diagnostic and therapeutic applications are crucial in almost every medical field, giving it a vital role in medical education. However, despite its importance and rapid integration into clinical practice, many curricula still dedicate minimal time to its teaching. Surveys by the European Society of Radiology (ESR) and other studies suggest the need for curriculum reform and increased dedicated teaching hours to better prepare future physicians.1, 2
Numerous studies show that while medical curricula are constantly evolving to meet healthcare demands, radiology is often inconsistently or restrictively taught. In the UK, for instance, only 15% of medical schools offer a dedicated radiology program, and many schools worldwide still teach it informally through clinicians, leading to a lack of structured goals and continuity from preclinical to clinical years.3-5 In contrast, universities with well-established programs, such as the Australian National University and the University of British Columbia, have shown significant improvements in students' diagnostic and interpretive skills.6, 7
A documented educational gap exists, as recent graduates often struggle with selecting and interpreting imaging studies.7, 8 Research suggests that interactive, case-based teaching and e-learning modules can enhance student engagement and critical thinking, improving the quality of radiology education.9, 10
At Northern Border University, radiology is introduced gradually over the six-year medical program. It begins with basic system-based modules in the second and third years, followed by a three-week course in the fourth year that covers technical and clinical aspects. Radiology concepts are then integrated into subsequent clinical rotations, with advanced training in the final year. While our program takes an integrated approach with dedicated faculty, continuous improvement is essential to ensure students develop the skills needed for effective, patient-centred imaging use. This study aims to explore students' perspectives on their radiology course to identify curriculum gaps and suggest ways to improve.
This was a mixed-methods study using a structured questionnaire with both quantitative and open-ended questions to evaluate students' radiology teaching experiences and preferences. The study was conducted at the Faculty of Medicine, Northern Border University, Arar, Saudi Arabia, from November 2024 to March 2025 after obtaining ethical approval (17/25/H) from Local Committee of Bio Ethics at Northern Border University.
A convenience sampling approach was used to recruit participants. The calculated sample size was 150 students, which was based on a 50% proportion of the total medical student population with a 95% confidence interval. Students from the 3rd, 4th, 5th, and 6th years who provided consent were included in the study. Data were analyzed using SPSS version 24. Chi-square tests were used to determine associations, and qualitative data were analyzed by grouping responses into different themes.
The mean age of the 150 participants was 23.41 ± 2.18 years; 93 (62%) were male and 57 (38%) were female. Of the total participants, 121 (80.6%) reported receiving formal radiology education, while 29 (19.3%) had not. Figure 1 depicts the year’s wise distribution of recruited participants.
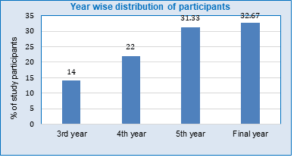
Figure 1: Year wide distribution of study participants
When asked about curriculum effectiveness, a majority of students either agreed or strongly agreed (P = 0.001). However, responses were inconsistent regarding the adequacy of the curriculum (P = 0.162). There was limited integration of radiology in preclinical years, but integration in clinical years was considered satisfactory (P = 0.041) (Table 1).
A full 100% of students agreed that hands-on training was lacking, with interventional radiology also noted as an underrepresented area.
Hands-on training is the most underrepresented area in the curriculum, with 100% of students agreeing that it's lacking. Interventional radiology was also identified as an underrepresented area. Figure 2 highlights the areas of the radiology curriculum that students feel are lacking.
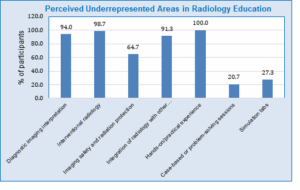
Figure 2: Underrepresented areas of radiology curriculum
The most popular teaching methods were lectures (145 or 96.7%) and case-based learning (141 or 94%). Only 30 students (20%) reported having hands-on exposure, which they acquired primarily through final-year internships (Figure 3). Study participants found hands-on sessions to be the most effective teaching strategy for the radiology curriculum, followed by case-based and problem-based sessions. Online sessions were reported as the least popular strategy (Table 2). The majority of participants (123 or 82%) felt that hands-on training was insufficient, and they needed more opportunities, while only 19 (12.2%) thought it was sufficient.
Hands-on/practical sessions Students were highly satisfied with their assessment methods, with 94% satisfied with written exams and 94.67% with Objective Structured Clinical Examinations (OSCEs).
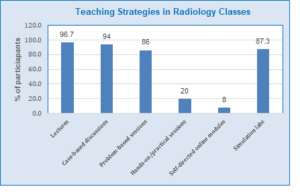
Figure 3. Common teaching strategies used for radiology classes
Regarding curriculum timing, 147 (98%) of students believed radiology should be introduced earlier. A high number of students (140 or 93%) were interested in learning more through various approaches, such as online modules and simulation labs. When asked about confidence in applying radiology knowledge in clinical practice, 103 (68.3%) felt confident, while 38 (25.3%) did not. Furthermore, 110 students (73.3%) felt prepared to interpret radiology findings for patient management, while 40 (26.6%) felt unprepared. A significant majority 146 (96.3%) highlighted that radiology reporting and communication skills needed more emphasis. Figure 4 shows the responses of students regarding emphasis on further implementation.
Qualitative responses showed a strong preference among students to focus on foundational knowledge at the undergraduate level. Comments such as "special attention should be given to basic knowledge of radiology" and "hands-on for the basic procedures should be promoted" highlight the desire to build a solid base in core techniques. Students consistently suggested that subspecialty topics should be reserved for postgraduate studies, where training could be tailored to meet individual career needs.
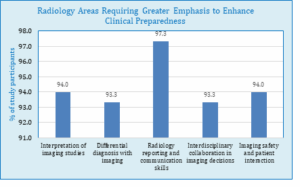
Figure 4: Aspects of radiology that need emphasis to improve clinical readiness
The study's findings align with existing literature, showing that most participants had a positive view of their formal radiology education, with 80.6% having received it and most agreeing the curriculum was effective. This supports research that highlights the value of structured radiology instruction in improving students' diagnostic abilities and confidence, especially when integrated well into clinical years.11, 12 However, the inconsistent responses on curriculum adequacy (P = 0.162) echo a broader debate in the literature about whether current curricula provide sufficient depth.
Our finding of minimal integration during early preclinical years is supported by studies that contend many medical schools still offer subpar radiology teaching at this crucial stage, potentially hindering foundational knowledge acquisition.13 Furthermore, the unanimous agreement on the lack of hands-on training is consistent with research highlighting that practical, experiential learning is a major deficit in many curricula, despite being crucial for skill development.14 While some programs have successfully incorporated hands-on modules, these discrepancies likely stem from variations in curriculum design and institutional resources.15, 16
Students' strong preference for case-based learning and traditional lectures is also well-documented in the literature, as these methods are valued for their structured delivery and clinical relevance.17, 18 Our study found that only 12.2% of students considered practical training sufficient, reflecting previous research indicating that this shortfall adversely affects confidence and competence in image interpretation.19 In contrast, some schools using simulation-based workshops offer substantial hands-on experience, which students find highly beneficial.20
Interestingly, participants' strong dissatisfaction with online sessions as a learning strategy contrast with other studies that found well-designed virtual modules to be effective supplements to traditional teaching.21 This difference might be due to variations in implementation quality or student familiarity with digital learning. The high satisfaction with written and OSCE exams aligns with research that values objective assessments for measuring radiological competence.22
The strong student consensus that radiology should be introduced earlier (98%) and their interest in various learning modalities (93%) are consistent with trends supporting early radiological exposure to improve clinical reasoning.23 However, the noted discrepancy between high interest and lower confidence in applying this knowledge highlights a key issue: without sufficient practical experience and clinical integration, students' readiness remains hampered. The emphasis on communication skills by 96.3% of respondents further underscores the need for a curriculum that goes beyond technical interpretation to include professional communication.24, 25
Qualitative feedback, which showed a preference for a strong foundation in core concepts over early sub specialization, aligns with educational frameworks that support a phased approach to training. This ensures students develop a solid diagnostic skill set before moving on to more complex topics, promoting better knowledge retention and clinical usefulness.26,27
5. Strengths
The combination of quantitative data with open-ended responses provided both statistical evidence and richer insights. Focusing on clinical-year medical students with a statistically calculated sample of 150 further strengthened the reliability and relevance of the findings.
6. Limitations
Convenience sampling may have introduced bias, reducing representativeness of the broader student body. In addition, reliance on self-reported data is prone to recall and social desirability bias, which may create discrepancies between reported and actual experiences.
Medical students underscored the need for a more cohesive radiology curriculum that bridges both preclinical and clinical training, noting that such integration would markedly enhance their confidence and clinical preparedness. They strongly recommended the implementation of case-based learning and hands-on image interpretation sessions to cultivate practical competencies. Furthermore, students emphasized that a structured undergraduate curriculum focused on essential radiology concepts is critical for developing a solid foundation, ultimately supporting informed clinical decision-making and improving patient care outcomes.
Authors affiliations:
- Muhammad Omer Afzal Bhatti, MCPS, Department of Surgery, Faculty of Medicine; Northern Border University, Arar, Kingdom of Saudi Arabia; Email: omer666afzal@hotmail.com
- Mujeeb Ur Rehman Parrey, Ph.D, Department of Surgery, Faculty of Medicine; Northern Border University, Arar, Kingdom of Saudi Arabia; Email: drparrey@gmail.com
- Pakeeza Shafiq, FCPS, Assistant Professor of Radiology, Department of Surgery, Faculty of Medicine; Northern Border University, Arar, Kingdom of Saudi Arabia; Email: pakeezashafiq@gmail.com
- Maha M. Abdul-Latif, MS, Department of Surgery, Faculty of Medicine; Northern Border University, Arar, Kingdom of Saudi Arabia; Email: mahamlatif79@gmail.com
- Haider Osman Elmisbah, MD, Department of Surgery, Faculty of Medicine; Northern Border University, Arar, Kingdom of Saudi Arabia; Email: haidermisbah2002@yahoo.com
ABSTRACT
Background and objective: Radiology plays a vital role in modern medicine, yet many new graduates face challenges in selecting the appropriate imaging studies and interpreting their findings. This study seeks to examine medical students’ perspectives on their undergraduate radiology curriculum in order to identify existing gaps and suggest areas for improvement.
Methodology: This mixed-methods study, conducted at the Faculty of Medicine, Northern Border University, from November 2024 to March 2025, used a structured questionnaire with quantitative and open-ended questions. A convenience sample of 150 students from the 3rd, 4th, 5th, and 6th years participated.
Results: The majority of students agreed or strongly agreed that the curriculum was effective (P < 0.001). However, they noted limited radiology integration in preclinical years, though it improved in clinical years (P = 0.041). A hundred percent of students agreed that hands-on training was lacking. The most preferred educational methods were lectures (96.7%) and case-based learning (94%). Notably, 98% of students believe radiology should be introduced earlier, and 93% were interested in more learning opportunities.
Conclusion: Students highlighted that better integration of radiology in both preclinical and clinical settings would boost their confidence and preparedness for clinical practice. They strongly recommended hands-on and case-based sessions to improve education and emphasized the need to focus on foundational radiology knowledge at the undergraduate level.
Abbreviations: ESR: European Society of Radiology, OSCE: Objective Structured Clinical Examinations
Keywords: Clinical Practice; Curriculum Enhancement; Medical Education; Mixed-methods study; Radiology
Citation: Bhatti MOA, Parrey MUR, Shafiq P, Abdul-Latif MM, Elmisbah HO. Bridging the gaps: medical students' perspectives on undergraduate radiology education and curriculum enhancement. Anaesth. pain intensive care 2025;29(8):955-961. DOI: 10.35975/apic.v29i8.3024
Received: August 25, 2025; Revised: August 29, 2025; Accepted: September 01, 2025
1. INTRODUCTION
Radiology's diagnostic and therapeutic applications are crucial in almost every medical field, giving it a vital role in medical education. However, despite its importance and rapid integration into clinical practice, many curricula still dedicate minimal time to its teaching. Surveys by the European Society of Radiology (ESR) and other studies suggest the need for curriculum reform and increased dedicated teaching hours to better prepare future physicians.1, 2
Numerous studies show that while medical curricula are constantly evolving to meet healthcare demands, radiology is often inconsistently or restrictively taught. In the UK, for instance, only 15% of medical schools offer a dedicated radiology program, and many schools worldwide still teach it informally through clinicians, leading to a lack of structured goals and continuity from preclinical to clinical years.3-5 In contrast, universities with well-established programs, such as the Australian National University and the University of British Columbia, have shown significant improvements in students' diagnostic and interpretive skills.6, 7
A documented educational gap exists, as recent graduates often struggle with selecting and interpreting imaging studies.7, 8 Research suggests that interactive, case-based teaching and e-learning modules can enhance student engagement and critical thinking, improving the quality of radiology education.9, 10
At Northern Border University, radiology is introduced gradually over the six-year medical program. It begins with basic system-based modules in the second and third years, followed by a three-week course in the fourth year that covers technical and clinical aspects. Radiology concepts are then integrated into subsequent clinical rotations, with advanced training in the final year. While our program takes an integrated approach with dedicated faculty, continuous improvement is essential to ensure students develop the skills needed for effective, patient-centred imaging use. This study aims to explore students' perspectives on their radiology course to identify curriculum gaps and suggest ways to improve.
2. METHODOLOGY
This was a mixed-methods study using a structured questionnaire with both quantitative and open-ended questions to evaluate students' radiology teaching experiences and preferences. The study was conducted at the Faculty of Medicine, Northern Border University, Arar, Saudi Arabia, from November 2024 to March 2025 after obtaining ethical approval (17/25/H) from Local Committee of Bio Ethics at Northern Border University.
A convenience sampling approach was used to recruit participants. The calculated sample size was 150 students, which was based on a 50% proportion of the total medical student population with a 95% confidence interval. Students from the 3rd, 4th, 5th, and 6th years who provided consent were included in the study. Data were analyzed using SPSS version 24. Chi-square tests were used to determine associations, and qualitative data were analyzed by grouping responses into different themes.
3. RESULTS
The mean age of the 150 participants was 23.41 ± 2.18 years; 93 (62%) were male and 57 (38%) were female. Of the total participants, 121 (80.6%) reported receiving formal radiology education, while 29 (19.3%) had not. Figure 1 depicts the year’s wise distribution of recruited participants.

Figure 1: Year wide distribution of study participants
When asked about curriculum effectiveness, a majority of students either agreed or strongly agreed (P = 0.001). However, responses were inconsistent regarding the adequacy of the curriculum (P = 0.162). There was limited integration of radiology in preclinical years, but integration in clinical years was considered satisfactory (P = 0.041) (Table 1).
| Table 1: Current status of radiology curriculum (n = 150) | |||||||
| Effectiveness of curriculum | Strongly agree | Agree | Neutral | Disagree | Strongly disagree | P-value | |
| 1 | Do you think that current radiology curriculum is effective? | 36 (24) | 64 (42.67) | 12 (8) | 21 (14) | 17 (11.33) | 0.001* |
| 2 | Does the current radiology curriculum adequately cover imaging fundamentals (e.g., X-rays, CT, MRI, ultrasound)? | 41 (27.33) | 52 (34.67) | 9 (6) | 37 (24.67) | 11 (7.33) | 0.162 |
| 3 | How frequently is radiology integrated into your pre-clinical courses? | 3 (2) | 41 (27.33) | 65 (43.33) | 41 (27.33) | 0 (0) | 0.333 |
| 4 | How frequently is radiology integrated into your clinical courses? | 49 (32.67) | 58 (38.67) | 22 (14.67) | 21 (14) | 0 (0) | 0.041* |
| Data are presented as n (%); P < 0.05 is considered significant | |||||||
A full 100% of students agreed that hands-on training was lacking, with interventional radiology also noted as an underrepresented area.
Hands-on training is the most underrepresented area in the curriculum, with 100% of students agreeing that it's lacking. Interventional radiology was also identified as an underrepresented area. Figure 2 highlights the areas of the radiology curriculum that students feel are lacking.

Figure 2: Underrepresented areas of radiology curriculum
The most popular teaching methods were lectures (145 or 96.7%) and case-based learning (141 or 94%). Only 30 students (20%) reported having hands-on exposure, which they acquired primarily through final-year internships (Figure 3). Study participants found hands-on sessions to be the most effective teaching strategy for the radiology curriculum, followed by case-based and problem-based sessions. Online sessions were reported as the least popular strategy (Table 2). The majority of participants (123 or 82%) felt that hands-on training was insufficient, and they needed more opportunities, while only 19 (12.2%) thought it was sufficient.
| Table 2: Most effective teaching strategy for radiology classes (frequency of responses) | |||||
| Teaching strategy | Very effective | Somewhat effective | Neutral | Ineffective | Very ineffective |
| Lectures | 103 | 23 | 4 | 11 | 9 |
| Case-based discussions | 131 | 11 | 1 | 5 | 2 |
| 138 | 7 | 1 | 3 | 1 | |
| Simulation Labs | 111 | 16 | 7 | 14 | 2 |
| Online sessions | 16 | 28 | 18 | 72 | 16 |
| Problem-based learning | 130 | 14 | 1 | 4 | 1 |
Hands-on/practical sessions Students were highly satisfied with their assessment methods, with 94% satisfied with written exams and 94.67% with Objective Structured Clinical Examinations (OSCEs).

Figure 3. Common teaching strategies used for radiology classes
Regarding curriculum timing, 147 (98%) of students believed radiology should be introduced earlier. A high number of students (140 or 93%) were interested in learning more through various approaches, such as online modules and simulation labs. When asked about confidence in applying radiology knowledge in clinical practice, 103 (68.3%) felt confident, while 38 (25.3%) did not. Furthermore, 110 students (73.3%) felt prepared to interpret radiology findings for patient management, while 40 (26.6%) felt unprepared. A significant majority 146 (96.3%) highlighted that radiology reporting and communication skills needed more emphasis. Figure 4 shows the responses of students regarding emphasis on further implementation.
Qualitative responses showed a strong preference among students to focus on foundational knowledge at the undergraduate level. Comments such as "special attention should be given to basic knowledge of radiology" and "hands-on for the basic procedures should be promoted" highlight the desire to build a solid base in core techniques. Students consistently suggested that subspecialty topics should be reserved for postgraduate studies, where training could be tailored to meet individual career needs.

Figure 4: Aspects of radiology that need emphasis to improve clinical readiness
4. DISCUSSION
The study's findings align with existing literature, showing that most participants had a positive view of their formal radiology education, with 80.6% having received it and most agreeing the curriculum was effective. This supports research that highlights the value of structured radiology instruction in improving students' diagnostic abilities and confidence, especially when integrated well into clinical years.11, 12 However, the inconsistent responses on curriculum adequacy (P = 0.162) echo a broader debate in the literature about whether current curricula provide sufficient depth.
Our finding of minimal integration during early preclinical years is supported by studies that contend many medical schools still offer subpar radiology teaching at this crucial stage, potentially hindering foundational knowledge acquisition.13 Furthermore, the unanimous agreement on the lack of hands-on training is consistent with research highlighting that practical, experiential learning is a major deficit in many curricula, despite being crucial for skill development.14 While some programs have successfully incorporated hands-on modules, these discrepancies likely stem from variations in curriculum design and institutional resources.15, 16
Students' strong preference for case-based learning and traditional lectures is also well-documented in the literature, as these methods are valued for their structured delivery and clinical relevance.17, 18 Our study found that only 12.2% of students considered practical training sufficient, reflecting previous research indicating that this shortfall adversely affects confidence and competence in image interpretation.19 In contrast, some schools using simulation-based workshops offer substantial hands-on experience, which students find highly beneficial.20
Interestingly, participants' strong dissatisfaction with online sessions as a learning strategy contrast with other studies that found well-designed virtual modules to be effective supplements to traditional teaching.21 This difference might be due to variations in implementation quality or student familiarity with digital learning. The high satisfaction with written and OSCE exams aligns with research that values objective assessments for measuring radiological competence.22
The strong student consensus that radiology should be introduced earlier (98%) and their interest in various learning modalities (93%) are consistent with trends supporting early radiological exposure to improve clinical reasoning.23 However, the noted discrepancy between high interest and lower confidence in applying this knowledge highlights a key issue: without sufficient practical experience and clinical integration, students' readiness remains hampered. The emphasis on communication skills by 96.3% of respondents further underscores the need for a curriculum that goes beyond technical interpretation to include professional communication.24, 25
Qualitative feedback, which showed a preference for a strong foundation in core concepts over early sub specialization, aligns with educational frameworks that support a phased approach to training. This ensures students develop a solid diagnostic skill set before moving on to more complex topics, promoting better knowledge retention and clinical usefulness.26,27
5. Strengths
The combination of quantitative data with open-ended responses provided both statistical evidence and richer insights. Focusing on clinical-year medical students with a statistically calculated sample of 150 further strengthened the reliability and relevance of the findings.
6. Limitations
Convenience sampling may have introduced bias, reducing representativeness of the broader student body. In addition, reliance on self-reported data is prone to recall and social desirability bias, which may create discrepancies between reported and actual experiences.
7. CONCLUSION
Medical students underscored the need for a more cohesive radiology curriculum that bridges both preclinical and clinical training, noting that such integration would markedly enhance their confidence and clinical preparedness. They strongly recommended the implementation of case-based learning and hands-on image interpretation sessions to cultivate practical competencies. Furthermore, students emphasized that a structured undergraduate curriculum focused on essential radiology concepts is critical for developing a solid foundation, ultimately supporting informed clinical decision-making and improving patient care outcomes.
- Acknowledgement
- Data availability
- Conflict of interest
- Authors’ contribution
12. REFERENCES
- Chau M, Arruzza E, Spuur K, Ofori-Manteaw B. From classroom to global impact: How radiography education advances the sustainable development goals. Radiography (Lond). 2025 Jan;31(1):224-230. https://doi.org/10.1016/j.radi.2024.11.015
- European Society of Radiology (ESR). Undergraduate education in radiology. A white paper by the European Society of Radiology. Insights Imaging. 2011 Aug;2(4):363-374. https://doi.org/10.1007/s13244-011-0104-5
- Lowitt NR. Assessment of an integrated curriculum in radiology. Acad Med. 2002 Sep;77(9):933. https://doi.org/10.1097/00001888-200209000-00037
- Kelly AM, Mullan PB. Designing a Curriculum for Professionalism and Ethics Within Radiology: Identifying Challenges and Expectations. Acad Radiol. 2018 May;25(5):610-618. https://doi.org/10.1016/j.acra.2018.02.007
- Elendu C, Amaechi DC, Okatta AU, Amaechi EC, Elendu TC, Ezeh CP, et al. The impact of simulation-based training in medical education: A review. Medicine (Baltimore). 2024 Jul 5;103(27):e38813. https://doi.org/10.1097/MD.0000000000038813
- Lee JS, Aldrich JE, Eftekhari A, Nicolaou S, Müller NL. Implementation of a new undergraduate radiology curriculum: experience at the University of British Columbia. Can Assoc Radiol J. 2007 Dec;58(5):272-8.
- Mirsadraee S, Mankad K, McCoubrie P, Roberts T, Kessel D. Radiology curriculum for undergraduate medical studies--a consensus survey. Clin Radiol. 2012 Dec;67(12):1155-61. https://doi.org/10.1016/j.crad.2012.03.017
- Nyhsen CM, Steinberg LJ, O'Connell JE. Undergraduate radiology teaching from the student's perspective. Insights Imaging. 2013 Feb;4(1):103-9. https://doi.org/10.1007/s13244-012-0206-8
- Ochoa JG, Wludyka P. Randomized comparison between traditional and traditional plus interactive Web-based methods for teaching seizure disorders. Teach Learn Med. 2008 Apr-Jun;20(2):114-7. https://doi.org/10.1080/10401330801989513
- Stirrat T, Martin R, Umair M, Waller J. Advancing radiology education for medical students: leveraging digital tools and resources. Pol J Radiol. 2024 Oct 22;89:e508-e516. https://doi.org/10.5114/pjr/193518
- Donkin R, Yule H, Fyfe T. Online case-based learning in medical education: a scoping review. BMC Med Educ. 2023 Aug 9;23(1):564. https://doi.org/10.1186/s12909-023-04520-w
- Chandramohan A, Krothapalli V, Augustin A, Kandagaddala M, Thomas HM, Sudarsanam TD, et al. Teleradiology and technology innovations in radiology: status in India and its role in increasing access to primary health care. Lancet Reg Health Southeast Asia. 2023 Apr 14;23:100195. https://doi.org/10.1016/j.lansea.2023.100195
- Harthoorn, F.S., Scharenborg, S.W.J., Brink, M. et al. Radiology education for medical students: a qualitative exploration of educational topics, teaching methods and future strategies. BMC Med Educ 24, 891 (2024). https://doi.org/10.1186/s12909-024-05879-0
- Wade SWT, Velan GM, Tedla N, Briggs N, Moscova M. What works in radiology education for medical students: a systematic review and meta-analysis. BMC Med Educ. 2024 Jan 10;24(1):51. https://doi.org/10.1186/s12909-023-04981-z
- Uppot RN, Laguna B, McCarthy CJ, De Novi G, Phelps A, Siegel E, et al. Implementing Virtual and Augmented Reality Tools for Radiology Education and Training, Communication, and Clinical Care. Radiology. 2019 Jun;291(3):570-580. https://doi.org/10.1148/radiol.2019182210
- Goldman DT, Peters GL, Fischman AM, Vatakencherry GG, Bream PR Jr, Martin JG, et al. Best Practices From the APDR: Improving Medical Student Exposure to Interventional Radiology. Acad Radiol. 2018 Jun;25(6):789-791. https://doi.org/10.1016/j.acra.2017.11.021
- McLean SF. Case-Based Learning and its Application in Medical and Health-Care Fields: A Review of Worldwide Literature. J Med Educ Curric Dev. 2016 Apr 27;3:JMECD.S20377. https://doi.org/10.4137/JMECD.S20377
- Yang W, Zhang X, Chen X, Lu J, Tian F. Based case based learning and flipped classroom as a means to improve international students' active learning and critical thinking ability. BMC Med Educ. 2024 Jul 15;24(1):759. https://doi.org/10.1186/s12909-024-05758-8
- Jaspan O, Wysocka A, Sanchez C, Schweitzer AD. Improving the Relationship Between Confidence and Competence: Implications for Diagnostic Radiology Training From the Psychology and Medical Literature. Acad Radiol. 2022 Mar;29(3):428-438. https://doi.org/10.1016/j.acra.2020.12.006
- Shetty S, Bhat S, Al Bayatti S, Al Kawas S, Talaat W, El-Kishawi M, et al. The Scope of Virtual Reality Simulators in Radiology Education: Systematic Literature Review. JMIR Med Educ. 2024 May 8;10:e52953. https://doi.org/10.2196/52953
- Upadhyay N, Wadkin JCR. Can training in diagnostic radiology be moved online during the COVID-19 pandemic? UK trainee perceptions of the Radiology-Integrated Training Initiative (R-ITI) e-learning platform. Clin Radiol. 2021 Nov;76(11):854-860. https://doi.org/10.1016/j.crad.2021.06.003
- Topuz AC and Kinshuk. Students’ acceptance of and preferences regarding online exams: a systematic literature review. Education Tech Research Dev 72, 1111–1151 (2024). https://doi.org/10.1007/s11423-023-10333-x
- Branstetter BF 4th, Faix LE, Humphrey AL, Schumann JB. Preclinical medical student training in radiology: the effect of early exposure. AJR Am J Roentgenol. 2007 Jan;188(1):W9-14. https://doi.org/10.2214/AJR.05.2139
- Kumsa MJ, Lemu BN, Nguse TM, Omiyi DO, Akudjedu TN. Clinical placement challenges associated with radiography education in a low-resource setting: A qualitative exploration of the Ethiopian landscape. Radiography (Lond). 2022 Aug;28(3):634-640. https://doi.org/10.1016/j.radi.2022.04.014
- Naeger DM, Webb EM, Zimmerman L, Elicker BM. Strategies for incorporating radiology into early medical school curricula. J Am Coll Radiol. 2014 Jan;11(1):74-9. https://doi.org/10.1016/j.jacr.2013.07.013
- Vanckavičienė A, Macijauskienė J, Blaževičienė A, et al. Assessment of radiographers’ competences from the perspectives of radiographers and radiologists: a cross-sectional survey in Lithuania. BMC Med Educ 17, 25 (2017). https://doi.org/10.1186/s12909-017-0863-x
- Masthoff M, Pawelka F, Zak G, de Leng B, Darici D, Schindler P, et al. Students' perspective on new teaching concepts for medical studies: case- and competency-based learning in radiology. Insights Imaging. 2025 Feb 6;16(1):31. https://doi.org/10.1186/s13244-025-01909-7