Azhar Rehman 1 , Areeba Shams Sarwari 2 , Asma Abdus Salam 3
Authors affiliations:
A 4-year-old child presented to a tertiary care hospital with symptoms of respiratory tract infection. During management, a nasopharyngeal airway (NPA) was inserted for better oxygenation and suctioning. Two hours later, it was observed that the NPA was missing. Investigations led to the eventual finding of the NPA in the stomach which was removed successfully with upper GI endoscopy under general anesthesia.
Abbreviations: NPA: nasopharyngeal airway, PVC: polyvinyl chloride.
Keywords: Nasopharyngeal airway, Endoscopic measures, Complications.
Citation: Rehman A, Sarwari AS, Salam AA. Endoscopic retrieval of nasopharyngeal airway in a pediatric patient: a case report. Anaesth. pain intensive care 2025;29(7):814-816; DOI: 10.35975/apic.v29i7.2978
Received: June 11, 2025; Revised: August 24, 2025; Accepted: September 30, 2025
Nasopharyngeal airway (NPA) is a hollow tubular device made up of flexible soft material, thermoplastic elastomer (like neoprene), Silkolatex, PVC, latex-free is preferred to avoid any allergic reaction. NPA improves oxygenation and ventilation in patients where face mask ventilation is inadequate due to partial airway obstruction.1 Its use is also recommended in patients who are spontaneously breathing with upper airway soft tissue obstruction.2 It is recognized as one of the easiest methods, utilized to maintain upper airway patency, and helps in pulmonary hygiene by providing access to the suction catheter. However, its application is not entirely free of potential complications.3 Patients with diminished airway reflexes due to neurological impairments are more prone to airway device dislodgement. In such high-risk patients, it can present as acute respiratory distress.4 Dislodgement can further potentially present as compromised respiratory function or gastrointestinal issues. NPA dislodgement is a recognized adverse event in the pediatric population as well, often due to a lack of proper fixation, improper sizing of the airway device, or if the flange of the NPA is small and soft, it can be pushed during noninvasive ventilation and suctioning. An investigator even used a safety pin, piercing through the flange of NPA to prevent dislodgement.5
The migration of NPA into the gastrointestinal tract, while rare, can present significant risks, including obstruction and infection. This situation is particularly concerning because the presence of the NPA in the stomach could result in vomiting, gastrointestinal obstruction, mucosal injury, and potential perforation, all of which require prompt intervention. Additionally, there is a heightened risk of aspiration if the NPA migrates back into the esophagus and pharynx, which could potentially lead to respiratory impairment.
This report presents a case of NPA dislodgment in a 4-year-old child. While the patient in this case did not develop a neurological condition, the case highlights the critical significance of monitoring for potential device dislodgement and highlights the importance of rapid intervention, if complications arise.
A 4-year-old male child was admitted to a tertiary care hospital with symptoms of cough, fever, and difficulty in breathing. He was diagnosed with a lower respiratory tract infection with respiratory distress. During management of the case, supplemental oxygen was provided using a nasal cannula and an NPA, size 3.0 mm, inserted through his right nostril. Regular interval suctioning was then performed through the NPA.
Two hours later, nursing staff noted that the NPA was no longer observable. The oral cavity was examined, and bedside was searched for the missing NPA, but it was not found. Finally, it was decided to have chest and abdominal X-rays. Abdominal X-ray film showed migration of NPA into the stomach (Figure 1). After counseling the parents and obtaining consent, the child was shifted to a facility equipped with endoscopic equipment.
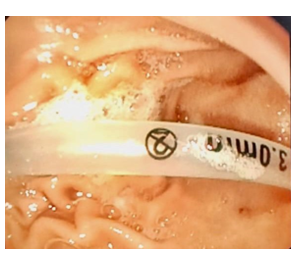
Figure 1: Endoscopic view showing a dislodged nasopharyngeal airway into the stomach.
Under general anesthesia, a rapid sequence induction technique was used, because the patient was considered to be full stomach. Medications used were propofol, suxamethonium, and fentanyl. Patient remained stable perioperatively, and the procedure lasted for 20 minutes. The NPA was safely removed using upper GI endoscope. Throughout the course patient remained stable. Patient was transferred intubated to the Pediatrics ICU after the procedure, as he was primarily having respiratory tract infection. The child was weaned and extubated on fulfilling the extubation criteria, and was discharged after 4 days to home when his respiratory tract infection settled.
Timely appreciation of the dislodged NPA and immediate diagnosis are crucial in detecting the exact location of NPA device and initiating an appropriate intervention. Briggs et al (2020) reported a case of retained NPA in an adult patient, just superior to the larynx, due to which the patient had respiratory distress symptoms, which was then removed almost 4 days after it was inserted.6 The main reason of this incident was, lack of communication. NPA was inserted by an ER team member, but they didn’t document it or inform them while handing over to the ICU team. Other reason was that the flange of NPA was very soft and small, therefore it readily slipped down. In our patient, the NPA that was inserted also had a small and soft flange due to which it slipped down, but luckily it was noticed within an hour, therefore appropriate action was taken immediately.
MU Khan described a case of an 85-year-old male having low GCS and sluggish upper airway reflexes, admitted to the hospital with suspected aspiration pneumonia. When a chest X-ray was done, it showed an NPA inside the trachea, just 2 cm above the carina, which was inserted 5 months back.7 The common thing in all these case reports is the type of NPA used, is a short and soft flange without any tape to secure the NPA.6-8
This case emphasizes the significance of secure fixation and consistent monitoring of airway devices in patients. Measures such as ensuring adequate sizing of the NPA, using securement precautions, and frequently checking the position of the airway can help prevent such situations. Furthermore, training healthcare staff to properly document whenever they use any type of airway, and it is preferred to give a written over to the other team.3
Securing the NPA is very important with the help of tape, but in long run it could cause skin peeling or tissue ischemia. For the prevention of such incidence, we recommend that the type of NPA should be used with a firm, hard rubber or plastic flange, so it won’t slip down the airway or into the esophagus.
Soft, flexible nasopharyngeal airway can be displaced in the trachea or esophagus if unattended or undocumented. It is especially important in the pediatric population and those adults having low GCS or weak airway reflexes. We recommend that the nursing staff attending such patients must be very vigilant and if any airway device is used, should mention in the monitoring chart as well, because it may lead to life life-threatening situation.
5. Conflict of interest
Nil declared by the authors
6. Authors’ contribution
All authors took part in the Concept, management of the case, and manuscript editing
Authors affiliations:
- Azhar Rehman, Department of Anesthesiology. PW, 2nd floor, Aga Khan Hospital, Stadium Road, Karachi, Pakistan; Email: azhar.rehman@aku.edu; {ORCID:0000-0002-0950-5377}
- Areeba Shams Sarwari, Ziauddin University, Clifton Campus. Karachi, Pakistan; Email: areebashams@hotmail.com
- Asma Abdus Salam, Department of Anesthesiology, Ziauddin Hospital, Karachi, Pakistan; Email: asma.salam@zu.edu.pk; {ORCID:0000-0001-6308-7762}
ABSTRACT
A 4-year-old child presented to a tertiary care hospital with symptoms of respiratory tract infection. During management, a nasopharyngeal airway (NPA) was inserted for better oxygenation and suctioning. Two hours later, it was observed that the NPA was missing. Investigations led to the eventual finding of the NPA in the stomach which was removed successfully with upper GI endoscopy under general anesthesia.
Abbreviations: NPA: nasopharyngeal airway, PVC: polyvinyl chloride.
Keywords: Nasopharyngeal airway, Endoscopic measures, Complications.
Citation: Rehman A, Sarwari AS, Salam AA. Endoscopic retrieval of nasopharyngeal airway in a pediatric patient: a case report. Anaesth. pain intensive care 2025;29(7):814-816; DOI: 10.35975/apic.v29i7.2978
Received: June 11, 2025; Revised: August 24, 2025; Accepted: September 30, 2025
1. INTRODUCTION
Nasopharyngeal airway (NPA) is a hollow tubular device made up of flexible soft material, thermoplastic elastomer (like neoprene), Silkolatex, PVC, latex-free is preferred to avoid any allergic reaction. NPA improves oxygenation and ventilation in patients where face mask ventilation is inadequate due to partial airway obstruction.1 Its use is also recommended in patients who are spontaneously breathing with upper airway soft tissue obstruction.2 It is recognized as one of the easiest methods, utilized to maintain upper airway patency, and helps in pulmonary hygiene by providing access to the suction catheter. However, its application is not entirely free of potential complications.3 Patients with diminished airway reflexes due to neurological impairments are more prone to airway device dislodgement. In such high-risk patients, it can present as acute respiratory distress.4 Dislodgement can further potentially present as compromised respiratory function or gastrointestinal issues. NPA dislodgement is a recognized adverse event in the pediatric population as well, often due to a lack of proper fixation, improper sizing of the airway device, or if the flange of the NPA is small and soft, it can be pushed during noninvasive ventilation and suctioning. An investigator even used a safety pin, piercing through the flange of NPA to prevent dislodgement.5
The migration of NPA into the gastrointestinal tract, while rare, can present significant risks, including obstruction and infection. This situation is particularly concerning because the presence of the NPA in the stomach could result in vomiting, gastrointestinal obstruction, mucosal injury, and potential perforation, all of which require prompt intervention. Additionally, there is a heightened risk of aspiration if the NPA migrates back into the esophagus and pharynx, which could potentially lead to respiratory impairment.
This report presents a case of NPA dislodgment in a 4-year-old child. While the patient in this case did not develop a neurological condition, the case highlights the critical significance of monitoring for potential device dislodgement and highlights the importance of rapid intervention, if complications arise.
2. CASE REPORT
A 4-year-old male child was admitted to a tertiary care hospital with symptoms of cough, fever, and difficulty in breathing. He was diagnosed with a lower respiratory tract infection with respiratory distress. During management of the case, supplemental oxygen was provided using a nasal cannula and an NPA, size 3.0 mm, inserted through his right nostril. Regular interval suctioning was then performed through the NPA.
Two hours later, nursing staff noted that the NPA was no longer observable. The oral cavity was examined, and bedside was searched for the missing NPA, but it was not found. Finally, it was decided to have chest and abdominal X-rays. Abdominal X-ray film showed migration of NPA into the stomach (Figure 1). After counseling the parents and obtaining consent, the child was shifted to a facility equipped with endoscopic equipment.

Figure 1: Endoscopic view showing a dislodged nasopharyngeal airway into the stomach.
Under general anesthesia, a rapid sequence induction technique was used, because the patient was considered to be full stomach. Medications used were propofol, suxamethonium, and fentanyl. Patient remained stable perioperatively, and the procedure lasted for 20 minutes. The NPA was safely removed using upper GI endoscope. Throughout the course patient remained stable. Patient was transferred intubated to the Pediatrics ICU after the procedure, as he was primarily having respiratory tract infection. The child was weaned and extubated on fulfilling the extubation criteria, and was discharged after 4 days to home when his respiratory tract infection settled.
3. DISCUSSION
Timely appreciation of the dislodged NPA and immediate diagnosis are crucial in detecting the exact location of NPA device and initiating an appropriate intervention. Briggs et al (2020) reported a case of retained NPA in an adult patient, just superior to the larynx, due to which the patient had respiratory distress symptoms, which was then removed almost 4 days after it was inserted.6 The main reason of this incident was, lack of communication. NPA was inserted by an ER team member, but they didn’t document it or inform them while handing over to the ICU team. Other reason was that the flange of NPA was very soft and small, therefore it readily slipped down. In our patient, the NPA that was inserted also had a small and soft flange due to which it slipped down, but luckily it was noticed within an hour, therefore appropriate action was taken immediately.
MU Khan described a case of an 85-year-old male having low GCS and sluggish upper airway reflexes, admitted to the hospital with suspected aspiration pneumonia. When a chest X-ray was done, it showed an NPA inside the trachea, just 2 cm above the carina, which was inserted 5 months back.7 The common thing in all these case reports is the type of NPA used, is a short and soft flange without any tape to secure the NPA.6-8
This case emphasizes the significance of secure fixation and consistent monitoring of airway devices in patients. Measures such as ensuring adequate sizing of the NPA, using securement precautions, and frequently checking the position of the airway can help prevent such situations. Furthermore, training healthcare staff to properly document whenever they use any type of airway, and it is preferred to give a written over to the other team.3
Securing the NPA is very important with the help of tape, but in long run it could cause skin peeling or tissue ischemia. For the prevention of such incidence, we recommend that the type of NPA should be used with a firm, hard rubber or plastic flange, so it won’t slip down the airway or into the esophagus.
4. CONCLUSION
Soft, flexible nasopharyngeal airway can be displaced in the trachea or esophagus if unattended or undocumented. It is especially important in the pediatric population and those adults having low GCS or weak airway reflexes. We recommend that the nursing staff attending such patients must be very vigilant and if any airway device is used, should mention in the monitoring chart as well, because it may lead to life life-threatening situation.
5. Conflict of interest
Nil declared by the authors
6. Authors’ contribution
All authors took part in the Concept, management of the case, and manuscript editing
7. REFERENCES
- Atanelov Z, Aina T, Smith T, et al. Nasopharyngeal airway [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan– [updated 2024 Jan 30; cited 2025 Aug 18]. Available from URL:https://www.ncbi.nlm.nih.gov/books/NBK513220/
- Royal Children’s Hospital (Melbourne).Nasopharyngeal airway insertion and management [Internet]. Melbourne: Royal Children’s Hospital; cited 2025 Aug 24. Available from URL: https://www.rch.org.au/rchcpg/hospital_clinical_guideline_index/Nasopharyngeal_Airway_Insertion_and_Management
- Roberts K, Whalley H, Bleetman A. The nasopharyngeal airway: dispelling myths and establishing the facts. Emerg Med J. 2005;22(6):394-396. PMCID: PMC1726817 DOI: 1136/emj.2004.021402
- Dua K, Saxena KN, Dua CK. Airway within airway: a case report. Indian J Anaesth. 2004;48:486–487.[ReaearchGate]
- Briggs B, Countryman C, McGinnis HD. One Notable Complication of Nasopharyngeal Airway: A Case Report. Clin Pract Cases Emerg Med. 2020;(4):584-586. PMCID: PMC7676774 DOI: 5811/cpcem.2020.8.48811
- Bajaj Y, Gadepalli C, Knight LC. Securing a nasopharyngeal airway. J Laryngol Otol. 2008;122(7):733-734. DOI: 1017/S0022215107001065
- Khan M, Khalid W, Latif N, Tanveer H. Nasopharyngeal Airway in the Trachea: A Case Report. Cureus 16(5): e60149. PMCID: PMC11166376 DOI: 7759/cureus.60149
- Temsah, M. Accidental Displacement of Nasopharyngeal Airway in a Child on Non-Invasive Ventilation (Case Report). The Egyptian Journal of Hospital Medicine, 2018; 71(6): 3304-3307.