Citra Tanoto 1 , I. Putu Kurniyanta 2 , Tjokorda Gde Agung Senapathi 3
Authors affiliations:
Ludwig’s angina is a deep neck and mouth floor infection that involves the submandibular and sublingual space and could spread inferiorly into the mediastinum. Life-threatening complications of Ludwig’s angina are airway obstruction and septic shock. Here we present a case of a 30-year-old woman who presented at 33 weeks pregnant with Ludwig’s angina, mediastinitis, and an impacted lower second and third molar. The patient underwent four surgeries consecutively, including caesarean delivery, surgical drainage of the submandibular and submental areas, thoracotomy, and odontectomy. On the first postoperative day, the patient had septic shock, and a sepsis bundle was implemented. However, the condition continued to deteriorate, and the patient passed away on the fifth day of care. Disease outcome varies between patients; therefore, the management approach should be individualized. Comprehensive multidisciplinary collaboration between an anesthesiologist, otolaryngologist, cardiothoracic surgeon, obstetrician-gynecologist, and oral-maxillofacial surgeon is crucial to reduce the risk of materno-fetal morbidity and mortality.
Abbreviations: LEMON: Look - Evaluate - Mallampati class - Obstruction - Neck (an acronym for the assessment of the airway’s appearance, identification of any dental issues, evaluation of Mallampati classification, assessment of airway obstruction, and examination of neck mobility), MOANS score: Mask seal - Obesity / Obstruction - Age (>55) - No teeth - Sleep apnea / Stiff lungs
Keywords: Pregnancy, Ludwig’s angina, septic shock, airway management
Citation: Tanoto C, Kurniyanta IP, Senapathi TGA. Four-in-one surgery in a 33-week pregnant patient with pseudo-angina Ludovici and mediastinal extension: a case report. Anaesth. pain intensive care 2025;29(6):646-650; DOI: 10.35975/apic.v29i6.2934
Received: June 16, 2025; Revised: July 07, 2025; Accepted: July 28, 2025
During pregnancy, women experience many physiological changes, including altered saliva secretion and increased oral cavity acidity, which disrupts the mucosal immunity and normal microbial flora. These changes increased the risk of having oral and odontogenic infections in pregnant women. It has been estimated that 25% women had odontogenic diseases during their pregnancy.1 Ludwig’s angina is one of the life-threatening complications of odontogenic infection, especially in second and third molars.2 Ludwig’s angina was introduced by Wilhelm Frederick von Ludwig in 1836 as an infection of neck connective tissue that could spread into the muscles that surrounded the larynx, the base of the oral cavity, and inferiorly into the mediastinum.3 Ludwig’s angina starts as a cellulitis and later progresses into a true abscess in the submandibular space, which increases the risk of airway obstruction and sepsis. The in-hospital mortality rate of septic shock is reported to be 40%.4 A study from one of the main referral hospitals in Indonesia reported 16 cases of Ludwig’s angina in which 11 patients had sepsis or septic shock, and mortality was reported in two patients.5 Difficulty in maintaining airway patency was reported to cause asphyxia and death in 8-10% patients.6 The main treatments of Ludwig’s angina include incision drainage, intravenous antibiotics, corticosteroids, and securing a patent airway.7 Multidisciplinary collaboration between an anesthesiologist, otolaryngologist, cardiothoracic surgeon, obstetrician-gynecologist, and oral-maxillofacial surgeon is crucial to reduce the risk of materno-fetal morbidity and mortality. Here we present a 30-year-old woman who presented at 33 weeks pregnant with Ludwig’s angina, mediastinitis, and impacted lower second and third molars who underwent four different surgeries (caesarean delivery, incision and drainage of the submandibular abscess, thoracotomy, and odontectomy) consecutively.
A 30-year-old woman presented at 33 weeks pregnant with Ludwig’s angina, mediastinitis, and an impacted lower second and third molar. The patient had complaints of painful swelling in her lower jaw and fever for five days, which caused difficulty in talking and opening her mouth. The patient also had shortness of breath in the afternoon before she got admitted to our hospital. The patient had a history of impacted lower second and third molars without any cavities. The patient was on her third pregnancy and had a history of two live births without any abortions. Other complaints, such as cough or runny nose in the past two weeks, were denied. Drug or food allergies were denied. Past illnesses such as hypertension, asthma, or heart disease were denied. A history of smoking or drinking alcohol was denied. The patient was a stay-at-home wife and capable of doing moderate-severe activity without any shortness of breath or chest pain. On admission to our hospital, her respiration rate was elevated (40-50x/min) with oxygen saturation 93% on room air and palpitation (122-143 beats/min). Other vital signs were within normal limits (blood pressure 102/62 mmHg, axillary temperature 36.7 °C). Anthropometric measurements found body weight 74 kg, height 156 cm, and BMI 30.45 kg/m2.
Physical examination revealed severe trismus (one finger), an elevated tongue, and fluctuating bilateral submandibular swelling extending into the thoracic cavity (Figure 1). Around 1 mL of bloody pus was aspirated from the left submandibular swelling. The fetal heart rate was 152/min. LEMON score was 4/10 (incisor distance < 3 fingerbreadths, Mallampati score >3, obstruction, limited neck mobility) and MOANS score 1/5 (obstruction). Laboratory tests revealed leucocytosis (16.89 x 103/µL), normochromic normocytic anemia (10.50 g/dL), and hypoalbuminemia (2.9 g/dL). Chest x-ray showed no abnormalities in the lungs and the heart (Figure 2). The patient was marked as ASA physical status III with sepsis.
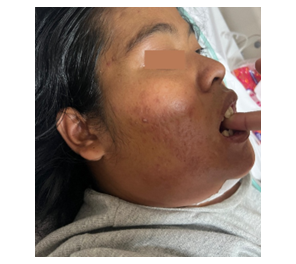
Figure 1: Physical examination revealed severe trismus and fluctuating bilateral submandibular swelling.
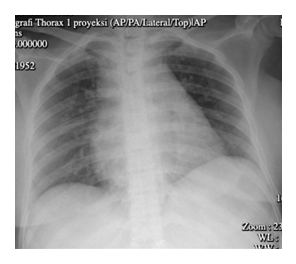
Figure 2: Chest x-ray showed no abnormalities in the lung and heart.
The patient was consulted by the otolaryngologist for surgical drainage, cardiothoracic surgeon for thoracotomy, obstetrician-gynecologist for caesarean delivery, and oral-maxillofacial surgeon for odontectomy. Dexamethasone 12 mg was given intramuscularly every twelve hours for fetal lung maturation prior to surgery.
Upon arrival at the pre-operating room, her vital signs were as follows: blood pressure 120/86 mmHg, heart rate 144/min, respiratory rate 35/min, oxygen saturation 98% on 3 L/min O2 through a nasal cannula. Two intravenous lines (22G on the left hand and 20G on the right hand) were inserted. The patient was nebulized 2% lidocaine, followed by a 10% lidocaine spray into the oral cavity. A flexible intubating scope (FIS) was used to guide the insertion of an endotracheal tube (size 7.0) in an awake patient. Intravenous propofol 50 mg, fentanyl 50 µg, and rocuronium 30 mg were administered for the induction of anesthesia. Anaesthesia was maintained by sevoflurane 1-3 col%, Fentanyl 0.25 µg/kg every 45-60 minutes, rocuronium 0.1 mg/kg every 30-45 minutes, dexmedetomidine 0.4-0.6 µg/kg/hour, and norepinephrine titration to keep MAP > 65 mmHg. Other medications were intravenous paracetamol 1 g, tranexamic acid 1 g, oxytocin 3 IU stat and 20 IU in infusion for 24 hours. A female baby, 1880 g, APGAR score 4-5-6, and no congenital abnormalities was delivered, who cried immediately after birth. The submandibular, submental, and thoracic space abscesses were successfully drained, followed by submental and thoracic drainage catheter placement. The impacted molars were also successfully extracted. Vital signs during the surgery were within normal limits; blood pressure 78-134 / 54-87 mmHg, respiratory rate 16-18x/min, and oxygen saturation 98-100%. Heart rate remained high (120-154 beats/min). The patient remained intubated postoperatively on pressure support ventilation due to impending respiratory failure and was shifted to the ICU. The patient was given fentanyl 300 µg in 500 mL normal saline and paracetamol 1 g every 8 hours as analgesic, broad-spectrum antibiotics, and methylprednisolone.
On the first postoperative day, the patient went into septic shock (SOFA score 8), and a sepsis bundle was implemented immediately. Blood culture revealed no microorganism growth. The patient was given norepinephrine titration (until MAP > 65 mmHg), dual antibiotics (ceftriaxone and metronidazole), and digoxin 0.5 mg IV (if heart rate >100 beats/min).
On the second day, echocardiography revealed mild pericardial effusion. The patient’s condition continued to deteriorate and eventually she passed away on the fifth day of care.
Ludwig’s angina is a deep neck and mouth floor infection that involves the submandibular and sublingual space. The life-threatening complications of Ludwig’s angina are airway obstruction and septic shock. Intubation (via routine orotracheal or fiberoptic nasotracheal) and tracheotomy are the main choices for securing airway.7 Induction of anesthesia poses a risk of complete airway obstruction and difficulty in face mask ventilation; meanwhile, orotracheal intubation may cause abscess rupture and pus aspiration. Orotracheal intubation is also difficult to perform in patients with Ludwig’s angina due to limited neck mobility and limited mouth opening. Therefore, the first choice for airway management is awake fiberoptic intubation with topical anesthesia (spray-as-you-go technique). The advantages of fiberoptic intubation are minimal pain and discomfort in most cases, and it can be done orally or nasally. One of the drawbacks of this procedure is aspiration if the patient vomits or regurgitates after applying topical anesthesia and before securing the airway.8 Fiberoptic intubation is performed in a head-up position (sitting or semi-Fowler) for a better visualization of the airway and control of secretions.7 A successful fiberoptic intubation depends on the operator’s skill; therefore, tracheostomy with local anesthesia is the second choice if intubation fails. A case series reported 25 successful tracheal intubations out of 26 patients with deep neck infection, in which 19 were done nasally and 6 orally. The complications were mild epistaxis in 3 patients and oversedation with transient hypoxemia in 4 patients.8 Another article reported successful airway management with fiberoptic nasotracheal intubation in a patient with Ludwig’s angina. However, the patient passed away due to septic shock on the sixth day of care in the ICU.6 The timing of extubation depends on the severity of infection and the patient’s condition.7
Another life-threatening complication of Ludwig’s angina is sepsis. The mortality rate of cervical necrotizing fasciitis accompanied by mediastinitis is 41% and 64% with sepsis. 9 A retrospective study in a university hospital in China reported that Ludwig’s angina mortality rate in the ICU was 10.34%. During treatment, 8 out of 29 patients developed mediastinitis, and 10 patients had severe sepsis. In the ICU, septic shock was reported in 11 patients, and vasopressors were administered to maintain blood pressure. Ludwig angina patients who developed mediastinitis were reported to have longer ICU length of stay compared to patients without mediastinitis.10 In a case series of 10 pregnant women with Ludwig’s angina, two deliveries were preterm, and two mothers died. One mother died in the hospital after she had had a stillbirth at home, and in the other case, both the mother and the baby died in the hospital.11,12 Another case report presented a 32-week pregnant woman with Ludwig’s angina and superior mediastinitis. The article reported satisfying improvement after the second surgery for superior mediastinum drainage (the first surgeries were caesarean section followed by surgical drainage of the submandibular and submental), and the patient was discharged after 21 days of care.13 A case report of a 34-week pregnant woman with Ludwig’s angina reported intrauterine fetal demise.12
Sepsis bundle, which includes early identification, lactate level measurement, blood culture, antibiotics, fluids, and vasopressor administration, should begin immediately to reduce mortality. The Surviving Sepsis Campaign recommended antibiotic administration within one hour of sepsis recognition. In patients with high risk for multidrug-resistant (MDR) organisms, dual antibiotics against gram-negative is recommended. Fluid resuscitation with crystalloid solution should be given at least 30 cc/kg in 3 hours.14 Norepinephrine is the first-line vasopressor agent for septic shock. The target mean arterial pressure (MAP) is ³65 mmHg to prevent hypotension and decreased tissue perfusion.14,15 A study from one of the main referral hospitals in Indonesia reported 16 cases of Ludwig’s angina in which 11 patients had sepsis or septic shock, and mortality was reported in two patients.5 Two articles reported mortality in a patient with Ludwig’s angina accompanied by septic shock.6,16 In the earlier case report, the infection spreads to the mediastinum, pericardium, and lung. The patient received broad-spectrum antibiotics and surgical drainage. However, the patient developed ventilation-associated pneumonia, septic shock, and eventually passed away.16 The latter article reported death due to septic shock on the sixth day of care. The patient received dual antibiotics (Ampicillin and Gentamicin); however, the authors did not mention the administration of a vasopressor.6 Another article reported good improvement and recovery with the administration of both antibiotics and a vasopressor.17
Procalcitonin tends to increase during inflammation, especially in bacterial infections. A meta-analysis study found that procalcitonin had a sensitivity of 77% and specificity of 79% in diagnosing sepsis in critically ill patients.18 A retrospective study reported that the 28-day mortality of patients with procalcitonin level ³7 ng/mL was 68.5%. Patients with procalcitonin level ³7 ng/mL have 1.55 times higher risk of mortality within 28 days in the ICU than those with procalcitonin level <7 ng/mL.19 A prospective study evaluating the role of serial procalcitonin level found that patients who did not show a procalcitonin decrease of >80% from baseline to day 4 had twice the higher risk of 28-day all-cause mortality.20
Our case report highlights the poor prognosis of Ludwig’s angina with mediastinitis and septic shock. Compared to other case reports, disease outcome varies between patients; therefore, the management approach should be individualized. Comprehensive multidisciplinary collaboration between an anesthesiologist, otolaryngologist, cardiothoracic surgeon, obstetrician-gynecologist, and oral-maxillofacial surgeon is crucial to reduce the risk of materno-fetal morbidity and mortality.
5. Acknowledgement6.
The authors would like to acknowledge all the doctors and health care professionals from the following departments for their contribution in this study: anesthesia and reanimation department; ear, nose, and throat department; cardiothoracic department; obstetrics and gynecology department; and oral-maxillofacial dentistry department.
6. Declaration of consent
The authors have obtained consent from the husband of the patient to report anonymized images and clinical information in the journal, while due effort will be made to conceal their identity.
7. Conflicts of interest
There are no conflicts of interest.
8. Authors’ contributions
All authors took part in the conceptualization, Data collection and analysis, and preparation of the first draft of the manuscript:
All authors approved this manuscript for submission.
Authors affiliations:
- Citra Tanoto. Jl. Diponegoro, Dauh Puri Klod, Kec. Denpasar Bar., Kota Denpasar, Bali 80113, Indonesia; Email; citratanoto@yahoo.co.id
- I Putu Kurniyanta, Jl. Diponegoro, Dauh Puri Klod, Kec. Denpasar Bar., Kota Denpasar, Bali 80113, Indonesia; Email; kurniyantaputu@yahoo.com
- Tjokorda Gde Agung Senapathi, Jl. Diponegoro, Dauh Puri Klod, Kec. Denpasar Bar., Kota Denpasar, Bali 80113, Indonesia; Email; tjoksenapathi@unud.ac.id
ABSTRACT
Ludwig’s angina is a deep neck and mouth floor infection that involves the submandibular and sublingual space and could spread inferiorly into the mediastinum. Life-threatening complications of Ludwig’s angina are airway obstruction and septic shock. Here we present a case of a 30-year-old woman who presented at 33 weeks pregnant with Ludwig’s angina, mediastinitis, and an impacted lower second and third molar. The patient underwent four surgeries consecutively, including caesarean delivery, surgical drainage of the submandibular and submental areas, thoracotomy, and odontectomy. On the first postoperative day, the patient had septic shock, and a sepsis bundle was implemented. However, the condition continued to deteriorate, and the patient passed away on the fifth day of care. Disease outcome varies between patients; therefore, the management approach should be individualized. Comprehensive multidisciplinary collaboration between an anesthesiologist, otolaryngologist, cardiothoracic surgeon, obstetrician-gynecologist, and oral-maxillofacial surgeon is crucial to reduce the risk of materno-fetal morbidity and mortality.
Abbreviations: LEMON: Look - Evaluate - Mallampati class - Obstruction - Neck (an acronym for the assessment of the airway’s appearance, identification of any dental issues, evaluation of Mallampati classification, assessment of airway obstruction, and examination of neck mobility), MOANS score: Mask seal - Obesity / Obstruction - Age (>55) - No teeth - Sleep apnea / Stiff lungs
Keywords: Pregnancy, Ludwig’s angina, septic shock, airway management
Citation: Tanoto C, Kurniyanta IP, Senapathi TGA. Four-in-one surgery in a 33-week pregnant patient with pseudo-angina Ludovici and mediastinal extension: a case report. Anaesth. pain intensive care 2025;29(6):646-650; DOI: 10.35975/apic.v29i6.2934
Received: June 16, 2025; Revised: July 07, 2025; Accepted: July 28, 2025
1. INTRODUCTION
During pregnancy, women experience many physiological changes, including altered saliva secretion and increased oral cavity acidity, which disrupts the mucosal immunity and normal microbial flora. These changes increased the risk of having oral and odontogenic infections in pregnant women. It has been estimated that 25% women had odontogenic diseases during their pregnancy.1 Ludwig’s angina is one of the life-threatening complications of odontogenic infection, especially in second and third molars.2 Ludwig’s angina was introduced by Wilhelm Frederick von Ludwig in 1836 as an infection of neck connective tissue that could spread into the muscles that surrounded the larynx, the base of the oral cavity, and inferiorly into the mediastinum.3 Ludwig’s angina starts as a cellulitis and later progresses into a true abscess in the submandibular space, which increases the risk of airway obstruction and sepsis. The in-hospital mortality rate of septic shock is reported to be 40%.4 A study from one of the main referral hospitals in Indonesia reported 16 cases of Ludwig’s angina in which 11 patients had sepsis or septic shock, and mortality was reported in two patients.5 Difficulty in maintaining airway patency was reported to cause asphyxia and death in 8-10% patients.6 The main treatments of Ludwig’s angina include incision drainage, intravenous antibiotics, corticosteroids, and securing a patent airway.7 Multidisciplinary collaboration between an anesthesiologist, otolaryngologist, cardiothoracic surgeon, obstetrician-gynecologist, and oral-maxillofacial surgeon is crucial to reduce the risk of materno-fetal morbidity and mortality. Here we present a 30-year-old woman who presented at 33 weeks pregnant with Ludwig’s angina, mediastinitis, and impacted lower second and third molars who underwent four different surgeries (caesarean delivery, incision and drainage of the submandibular abscess, thoracotomy, and odontectomy) consecutively.
2. CARE REPORT
A 30-year-old woman presented at 33 weeks pregnant with Ludwig’s angina, mediastinitis, and an impacted lower second and third molar. The patient had complaints of painful swelling in her lower jaw and fever for five days, which caused difficulty in talking and opening her mouth. The patient also had shortness of breath in the afternoon before she got admitted to our hospital. The patient had a history of impacted lower second and third molars without any cavities. The patient was on her third pregnancy and had a history of two live births without any abortions. Other complaints, such as cough or runny nose in the past two weeks, were denied. Drug or food allergies were denied. Past illnesses such as hypertension, asthma, or heart disease were denied. A history of smoking or drinking alcohol was denied. The patient was a stay-at-home wife and capable of doing moderate-severe activity without any shortness of breath or chest pain. On admission to our hospital, her respiration rate was elevated (40-50x/min) with oxygen saturation 93% on room air and palpitation (122-143 beats/min). Other vital signs were within normal limits (blood pressure 102/62 mmHg, axillary temperature 36.7 °C). Anthropometric measurements found body weight 74 kg, height 156 cm, and BMI 30.45 kg/m2.
Physical examination revealed severe trismus (one finger), an elevated tongue, and fluctuating bilateral submandibular swelling extending into the thoracic cavity (Figure 1). Around 1 mL of bloody pus was aspirated from the left submandibular swelling. The fetal heart rate was 152/min. LEMON score was 4/10 (incisor distance < 3 fingerbreadths, Mallampati score >3, obstruction, limited neck mobility) and MOANS score 1/5 (obstruction). Laboratory tests revealed leucocytosis (16.89 x 103/µL), normochromic normocytic anemia (10.50 g/dL), and hypoalbuminemia (2.9 g/dL). Chest x-ray showed no abnormalities in the lungs and the heart (Figure 2). The patient was marked as ASA physical status III with sepsis.

Figure 1: Physical examination revealed severe trismus and fluctuating bilateral submandibular swelling.

Figure 2: Chest x-ray showed no abnormalities in the lung and heart.
The patient was consulted by the otolaryngologist for surgical drainage, cardiothoracic surgeon for thoracotomy, obstetrician-gynecologist for caesarean delivery, and oral-maxillofacial surgeon for odontectomy. Dexamethasone 12 mg was given intramuscularly every twelve hours for fetal lung maturation prior to surgery.
Upon arrival at the pre-operating room, her vital signs were as follows: blood pressure 120/86 mmHg, heart rate 144/min, respiratory rate 35/min, oxygen saturation 98% on 3 L/min O2 through a nasal cannula. Two intravenous lines (22G on the left hand and 20G on the right hand) were inserted. The patient was nebulized 2% lidocaine, followed by a 10% lidocaine spray into the oral cavity. A flexible intubating scope (FIS) was used to guide the insertion of an endotracheal tube (size 7.0) in an awake patient. Intravenous propofol 50 mg, fentanyl 50 µg, and rocuronium 30 mg were administered for the induction of anesthesia. Anaesthesia was maintained by sevoflurane 1-3 col%, Fentanyl 0.25 µg/kg every 45-60 minutes, rocuronium 0.1 mg/kg every 30-45 minutes, dexmedetomidine 0.4-0.6 µg/kg/hour, and norepinephrine titration to keep MAP > 65 mmHg. Other medications were intravenous paracetamol 1 g, tranexamic acid 1 g, oxytocin 3 IU stat and 20 IU in infusion for 24 hours. A female baby, 1880 g, APGAR score 4-5-6, and no congenital abnormalities was delivered, who cried immediately after birth. The submandibular, submental, and thoracic space abscesses were successfully drained, followed by submental and thoracic drainage catheter placement. The impacted molars were also successfully extracted. Vital signs during the surgery were within normal limits; blood pressure 78-134 / 54-87 mmHg, respiratory rate 16-18x/min, and oxygen saturation 98-100%. Heart rate remained high (120-154 beats/min). The patient remained intubated postoperatively on pressure support ventilation due to impending respiratory failure and was shifted to the ICU. The patient was given fentanyl 300 µg in 500 mL normal saline and paracetamol 1 g every 8 hours as analgesic, broad-spectrum antibiotics, and methylprednisolone.
On the first postoperative day, the patient went into septic shock (SOFA score 8), and a sepsis bundle was implemented immediately. Blood culture revealed no microorganism growth. The patient was given norepinephrine titration (until MAP > 65 mmHg), dual antibiotics (ceftriaxone and metronidazole), and digoxin 0.5 mg IV (if heart rate >100 beats/min).
On the second day, echocardiography revealed mild pericardial effusion. The patient’s condition continued to deteriorate and eventually she passed away on the fifth day of care.
3. DISCUSSION
Ludwig’s angina is a deep neck and mouth floor infection that involves the submandibular and sublingual space. The life-threatening complications of Ludwig’s angina are airway obstruction and septic shock. Intubation (via routine orotracheal or fiberoptic nasotracheal) and tracheotomy are the main choices for securing airway.7 Induction of anesthesia poses a risk of complete airway obstruction and difficulty in face mask ventilation; meanwhile, orotracheal intubation may cause abscess rupture and pus aspiration. Orotracheal intubation is also difficult to perform in patients with Ludwig’s angina due to limited neck mobility and limited mouth opening. Therefore, the first choice for airway management is awake fiberoptic intubation with topical anesthesia (spray-as-you-go technique). The advantages of fiberoptic intubation are minimal pain and discomfort in most cases, and it can be done orally or nasally. One of the drawbacks of this procedure is aspiration if the patient vomits or regurgitates after applying topical anesthesia and before securing the airway.8 Fiberoptic intubation is performed in a head-up position (sitting or semi-Fowler) for a better visualization of the airway and control of secretions.7 A successful fiberoptic intubation depends on the operator’s skill; therefore, tracheostomy with local anesthesia is the second choice if intubation fails. A case series reported 25 successful tracheal intubations out of 26 patients with deep neck infection, in which 19 were done nasally and 6 orally. The complications were mild epistaxis in 3 patients and oversedation with transient hypoxemia in 4 patients.8 Another article reported successful airway management with fiberoptic nasotracheal intubation in a patient with Ludwig’s angina. However, the patient passed away due to septic shock on the sixth day of care in the ICU.6 The timing of extubation depends on the severity of infection and the patient’s condition.7
Another life-threatening complication of Ludwig’s angina is sepsis. The mortality rate of cervical necrotizing fasciitis accompanied by mediastinitis is 41% and 64% with sepsis. 9 A retrospective study in a university hospital in China reported that Ludwig’s angina mortality rate in the ICU was 10.34%. During treatment, 8 out of 29 patients developed mediastinitis, and 10 patients had severe sepsis. In the ICU, septic shock was reported in 11 patients, and vasopressors were administered to maintain blood pressure. Ludwig angina patients who developed mediastinitis were reported to have longer ICU length of stay compared to patients without mediastinitis.10 In a case series of 10 pregnant women with Ludwig’s angina, two deliveries were preterm, and two mothers died. One mother died in the hospital after she had had a stillbirth at home, and in the other case, both the mother and the baby died in the hospital.11,12 Another case report presented a 32-week pregnant woman with Ludwig’s angina and superior mediastinitis. The article reported satisfying improvement after the second surgery for superior mediastinum drainage (the first surgeries were caesarean section followed by surgical drainage of the submandibular and submental), and the patient was discharged after 21 days of care.13 A case report of a 34-week pregnant woman with Ludwig’s angina reported intrauterine fetal demise.12
Sepsis bundle, which includes early identification, lactate level measurement, blood culture, antibiotics, fluids, and vasopressor administration, should begin immediately to reduce mortality. The Surviving Sepsis Campaign recommended antibiotic administration within one hour of sepsis recognition. In patients with high risk for multidrug-resistant (MDR) organisms, dual antibiotics against gram-negative is recommended. Fluid resuscitation with crystalloid solution should be given at least 30 cc/kg in 3 hours.14 Norepinephrine is the first-line vasopressor agent for septic shock. The target mean arterial pressure (MAP) is ³65 mmHg to prevent hypotension and decreased tissue perfusion.14,15 A study from one of the main referral hospitals in Indonesia reported 16 cases of Ludwig’s angina in which 11 patients had sepsis or septic shock, and mortality was reported in two patients.5 Two articles reported mortality in a patient with Ludwig’s angina accompanied by septic shock.6,16 In the earlier case report, the infection spreads to the mediastinum, pericardium, and lung. The patient received broad-spectrum antibiotics and surgical drainage. However, the patient developed ventilation-associated pneumonia, septic shock, and eventually passed away.16 The latter article reported death due to septic shock on the sixth day of care. The patient received dual antibiotics (Ampicillin and Gentamicin); however, the authors did not mention the administration of a vasopressor.6 Another article reported good improvement and recovery with the administration of both antibiotics and a vasopressor.17
Procalcitonin tends to increase during inflammation, especially in bacterial infections. A meta-analysis study found that procalcitonin had a sensitivity of 77% and specificity of 79% in diagnosing sepsis in critically ill patients.18 A retrospective study reported that the 28-day mortality of patients with procalcitonin level ³7 ng/mL was 68.5%. Patients with procalcitonin level ³7 ng/mL have 1.55 times higher risk of mortality within 28 days in the ICU than those with procalcitonin level <7 ng/mL.19 A prospective study evaluating the role of serial procalcitonin level found that patients who did not show a procalcitonin decrease of >80% from baseline to day 4 had twice the higher risk of 28-day all-cause mortality.20
4. CONCLUSION
Our case report highlights the poor prognosis of Ludwig’s angina with mediastinitis and septic shock. Compared to other case reports, disease outcome varies between patients; therefore, the management approach should be individualized. Comprehensive multidisciplinary collaboration between an anesthesiologist, otolaryngologist, cardiothoracic surgeon, obstetrician-gynecologist, and oral-maxillofacial surgeon is crucial to reduce the risk of materno-fetal morbidity and mortality.
5. Acknowledgement6.
The authors would like to acknowledge all the doctors and health care professionals from the following departments for their contribution in this study: anesthesia and reanimation department; ear, nose, and throat department; cardiothoracic department; obstetrics and gynecology department; and oral-maxillofacial dentistry department.
6. Declaration of consent
The authors have obtained consent from the husband of the patient to report anonymized images and clinical information in the journal, while due effort will be made to conceal their identity.
7. Conflicts of interest
There are no conflicts of interest.
8. Authors’ contributions
All authors took part in the conceptualization, Data collection and analysis, and preparation of the first draft of the manuscript:
All authors approved this manuscript for submission.
9. REFERENCES
- Balaji VCR, Vani K. Ludwig’s Angina During Pregnancy-A Case Report. Indian Journal of Dental Research. 2024 Jan;35(1):104–6.
- Quinn FB. Ludwig angina. Arch Otolaryngol Head Neck Surg. 1999 May;125(5):599.
- Marple BF. Ludwig Angina. Arch Otolaryngol Head Neck Surg. 1999 May 1;125(5):596.
- Keeley A, Hine P, Nsutebu E. The recognition and management of sepsis and septic shock: a guide for non-intensivists. Postgrad Med J. 2017 Oct 1;93(1104):626–34.
- Muharty A, Nurwiadh A, Sjamsudin E, Adiantoro S, Nusjirwan R. Ludwig’s angina: an analysis of sixteen cases at Hasan Sadikin Hospital, Bandung, Indonesia. Int J Oral Maxillofac Surg. 2017 Mar;46:147.
- Fellini RT, Volquind D, Schnor OH, Angeletti MG, Souza OE de. Airway management in Ludwig’s angina – a challenge: case report. Brazilian Journal of Anesthesiology (English Edition). 2017 Nov;67(6):637–40.
- Shockley WW. Ludwig Angina. Arch Otolaryngol Head Neck Surg. 1999 May 1;125(5):600.
- Ovassapian A, Tuncbilek M, Weitzel EK, Joshi CW. Airway Management in Adult Patients with Deep Neck Infections: A Case Series and Review of the Literature. Anesth Analg. 2005 Feb;100(2):585–9.
- Sarna T, Sengupta T, Miloro M, Kolokythas A. Cervical Necrotizing Fasciitis With Descending Mediastinitis: Literature Review and Case Report. Journal of Oral and Maxillofacial Surgery. 2012 Jun;70(6):1342–50.
- Lin Q-L, Du H-L, Xiong H-Y, Li B, Liu J, Xing X-H. Characteristics and outcomes of Ludwig’s angina in patients admitted to the intensive care unit: A 6-year retrospective study of 29 patients. J Dent Sci. 2020 Dec;15(4):445–50.
- Osunde O, Bassey G, Ver-Or N. Management of Ludwig’s Angina in Pregnancy: A Review of 10 Cases. Ann Med Health Sci Res. 2014 May;4(3):361–4.
- Mukherjee S, Sharma S, Maru L. Poor dental hygiene in pregnancy leading to submandibular cellulitis and intrauterine fetal demise: case report and literature review. Int J Prev Med. 2013 May;4(5):603–6.
- Kamath A, Bhagania M, Balakrishna R, Sevagur G, Amar R. Ludwig’s Angina in Pregnancy Necessitating Pre Mature Delivery. J Maxillofac Oral Surg. 2015 Mar;14(Suppl 1):186–9.
- Evans L, Rhodes A, Alhazzani W, Antonelli M, Coopersmith C, French C, et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock 2021. Crit Care Med. 2021 Nov 14;49(11):e1063–143.
- De Backer D, Aldecoa C, Njimi H, Vincent J-L. Dopamine versus norepinephrine in the treatment of septic shock. Crit Care Med. 2012 Mar;40(3):725–30.
- Chequetto T, Serafini F, Ruivo G, Carvalho L, Guida M, Falopa V. Septic Shock Secondary to Mediastinitis Due to Ludwig Angina after Dental Abscess: A Case Report. Int Arch Otorhinolaryngol. 2014 Sep 4;18(S 01):2335.
- Sjamsudin E, Manurung B, Arumsari A, Maulina T. The management of septic shock and Ludwig’s angina: A case report of a life-threatening condition. SAGE Open Med Case Rep. 2020;8:2050313X20930909.
- Wacker C, Prkno A, Brunkhorst FM, Schlattmann P. Procalcitonin as a diagnostic marker for sepsis: a systematic review and meta-analysis. Lancet Infect Dis. 2013 May;13(5):426–35.
- Suranadi IW, Sinardja CD, Suryadi IA. Role of Procalcitonin in Predicting Mortality and Organ Dysfunction at Intensive Care Admission. Int J Gen Med. 2022;15:4917–23.
- Schuetz P, Birkhahn R, Sherwin R, Jones AE, Singer A, Kline JA, et al. Serial Procalcitonin Predicts Mortality in Severe Sepsis Patients: Results From the Multicenter Procalcitonin MOnitoring SEpsis (MOSES) Study. Crit Care Med. 2017 May;45(5):781–9.