Bhavini Shah 1 , Pragya Pramanik 2
Authors affiliations:
1. Bhavini Shah, Dr. D. Y. Patil Medical College Hospital & Research Centre. Pune, Maharashtra, India; Email: drbhavinishah71@gmail.co
2. Pragya Pramanik, Dr. D. Y. Patil Medical College Hospital & Research Centre. Pune, Maharashtra, India; Email: pramanik.pragya124@gmail.com
Correspondence: Pragya Pramanik, Email: pramanik.pragya124@gmail.com
Hirayama disease is a rare cervical myelopathy characterized by dynamic compression of the spinal cord during neck flexion, presenting unique challenges for anesthetic management. This case report describes the successful use of a supraclavicular brachial plexus block for tendon transfer surgery in a patient with Hirayama disease (HD).
A 34-year-old male with a 10-year history of progressive left hand weakness and atrophy, diagnosed with HD, was scheduled for tendon transfer surgery to improve hand function. Given concerns about cervical spine manipulation and potential cord compression with general anesthesia, a supraclavicular brachial plexus block was selected as the primary anesthetic technique. Ultrasound-guided block was performed using a combination of 0.75% ropivacaine 15mL and 2% lidocaine 10 mL, and 8mg of dexamethasone given achieving complete sensory and motor blockade within 12 min. The patient maintained a comfortable neutral neck position throughout the procedure. Surgery proceeded uneventfully with excellent surgical conditions and hemodynamic stability. Postoperatively, the patient reported minimal pain (VAS score 2/10) requiring only acetaminophen for the first 24 hours, expressed high satisfaction with the anesthetic technique, and was discharged on the second postoperative day without complications.
Conclusion: Supraclavicular brachial plexus block represents an effective and safe anesthetic technique for patients with HD undergoing upper limb procedures, avoiding risks associated with neck manipulation during general anesthesia while providing excellent surgical conditions and postoperative pain control. This approach should be considered as a primary option for appropriate surgeries in this patient population.
Abbreviations: BMI: Body Mass Index, HD: Hirayama Disease, VAS: Visual Analog Scale,
Keywords: Hirayama Disease; USG Guided; Supraclavicular Brachial Plexus Block; Tendon Transfer
Citation: Shah B, Pramanik P. Anesthetic management for tendon transfer in a patient with monomelic amyotrophy (Hirayama Disease): A case report. Anaesth. pain intensive care 2025;29(5):428-432. DOI: 10.35975/apic.v29i5.2864
Received: April 10, 2025; Revised: May 07, 2025; Accepted: May 09, 2025
Hirayama disease (HD), also known as juvenile muscular atrophy of the distal upper extremity, is a rare, self-limiting cervical myelopathy characterized by asymmetric weakness and wasting of muscles innervated by the C7, C8, and T1 nerve roots, predominantly affecting young males.1,2 First described by Hirayama in 1959, the condition typically manifests in the second or third decade of life with insidious onset of unilateral or bilateral distal upper limb weakness and atrophy, often affecting the hand and forearm musculature.3
The pathophysiology is associated with dynamic cord compression during neck flexion due to forward displacement of the posterior dural sac and compression of the cervical cord against vertebral bodies.4 This unique pathology presents distinct challenges in perioperative management, particularly concerning positioning and airway management during anesthesia.5
Tendon transfer procedures are commonly performed to improve hand function in patients with HD who have residual muscle weakness despite disease stabilization.6 These reconstructive surgeries aim to restore functional balance by transferring functioning tendons to replace the action of paralyzed muscles.7
The anesthetic management of patients with HD requires careful consideration due to potential cervical spine instability and the risk of exacerbating cord compression during manipulation of the neck.8 Regional anesthesia techniques, particularly peripheral nerve blocks, offer considerable advantages in such cases by avoiding airway manipulation and providing excellent postoperative analgesia.9
The supraclavicular brachial plexus block represents an effective anesthetic approach for upper limb surgeries, providing dense and reliable anesthesia with rapid onset. This technique may be particularly beneficial in patients with HD undergoing tendon transfer procedures, as it circumvents the need for neck manipulation associated with general anesthesia (GA) and neuraxial techniques.10
This case report describes the successful anesthetic management using a USG guided supraclavicular block for tendon transfer surgery in a patient with HD, highlighting the considerations, techniques, and outcomes relevant to anesthetic practice in this rare neurological condition.
A 34-year-old male presented to our tertiary care hospital with progressive weakness and wasting of the left hand musculature, particularly affecting the intrinsic muscles, that had gradually worsened over the past decade. Despite multiple consultations and parallel therapies including physiotherapy and neurological rehabilitation, the patient experienced minimal improvement in his condition. He reported increasing difficulty with fine motor tasks such as buttoning shirts, typing, and gripping objects, significantly impacting his professional life as a software engineer.
The patient's medical history was remarkable for an initial misdiagnosis of cervical radiculopathy at a local clinic, which delayed appropriate treatment for several years. Upon comprehensive neurological evaluation at our institution two years prior, electromyography studies revealed denervation patterns in the C7-T1 distribution, predominantly affecting the left hand. Subsequent dynamic MRI of the cervical spine in flexion demonstrated the characteristic forward displacement of the posterior dural sac with flattening of the cervical cord against the vertebral bodies, confirming the diagnosis of HD.
Interestingly, the patient had noticed that his symptoms worsened during cold weather and after prolonged periods of neck flexion while working on his computer. He had independently developed adaptive strategies, including using voice recognition software and specialized ergonomic equipment, to continue his work. The patient was psychologically resilient but increasingly frustrated by the functional limitations imposed by his condition.
Upon preoperative assessment, the patient was classified as ASA physical status II with a metabolic equivalent of task (METs) score greater than 4, indicating good functional capacity. His preoperative bedside pfts and neurological status were normal. His power was 5/5 in both upper and lower limbs. His vital signs were within normal limits: blood pressure 118/76 mmHg, heart rate 72 beats / min, respiratory rate 14 breaths / min, and oxygen saturation 99% on room air. His height was 175 cm tall and weighing 60 kg (BMI 19.6 kg/m²), the patient appeared slightly underweight but well-nourished. Laboratory investigations, including complete hemogram, liver function tests, renal function tests, serum electrolytes, and coagulation profile (bleeding time and clotting time were within normal ranges. Chest X-ray revealed increased bronchovascular markings and ECG revealed normal sinus rhythm.
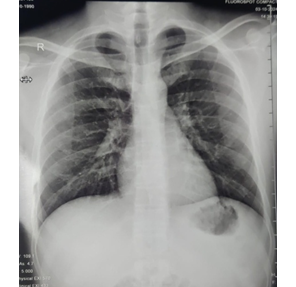
Figure 1: Increased vascular markings in the hilums
Airway examination revealed a Mallampati class II airway with normal thyromental distance and adequate mouth opening. Notably, the patient demonstrated limited cervical spine mobility, particularly during flexion, which he attributed to a conscious effort to avoid positions that exacerbated his symptoms. This finding was particularly significant for anesthetic planning, as it raised concerns about potential difficulties with conventional laryngoscopy and intubation if GA was to be employed.
After comprehensive multidisciplinary discussion involving the hand surgeon, neurologist, and anesthesia team, the patient was scheduled for tendon transfer surgery to improve hand function by redistributing the activity of functioning muscles to restore the actions of paralyzed ones. The planned procedure involved transfer of the pronator teres to extensor carpi radialis brevis, and flexor carpi radialis to finger extensors.
Given the patient's diagnosis, concerns regarding cervical spine manipulation, and the nature of the procedure, the anesthesia team proposed a supraclavicular brachial plexus block as the primary anesthetic technique. The patient, initially apprehensive about remaining awake during the procedure, was educated about the benefits of regional anesthesia in his specific case and the option for conscious sedation if needed. After thorough discussion and addressing his concerns, he provided informed consent for the proposed anesthetic plan.
Patient was instructed to remain nil by mouth from midnight prior to surgery. On arrival in the preoperative room, baseline vital parameters including pulse rate, non-invasive blood pressure, ECG and oxygen saturation were recorded. Peripheral venous access was established and intravenous fluid administration was initiated.
In the operation theatre, standard monitoring including electrocardiography, non-invasive blood pressure, and pulse oximetry were attached, baseline parameters including heart rate, systolic blood pressure, diastolic blood pressure, mean arterial pressure, and oxygen saturation were recorded. The patient was put on Hudson mask on 4 litres of oxygen and inj midazolam 0.02 mg/kg and inj fentanyl 2 µg/kg was administered to alleviate anxiety and for smooth conduction of the procedure.
The supraclavicular brachial plexus block was performed under ultrasound guidance using a Hitachi Arietta S70 machine with a linear probe. The patient was positioned supine with a small bolster under the shoulder, and the head turned 45 degrees to the contralateral side. After aseptic preparation, the supraclavicular fossa was scanned to identify key anatomical structures including the subclavian artery, first rib, pleura, and brachial plexus cluster. Local skin infiltration was administered before advancing a 22G long needle from lateral to medial axis under ultrasound guidance. A 22 1.5G hypodermic needle was inserted using an in-plane technique and half of 15 mL of 0.75% ropivacaine and 10 mL of 2% lignocaine with adrenaline was given and 8mg of dexamethasone was administered to potentiate the action and prolong the duration of the drug and then the needle was repositioned cranially towards the neural cluster for administration of the remaining volume, maintaining careful aspiration technique throughout the procedure.
Sensory block was evaluated using pinprick sensation, while motor block was assessed using a modified Bromage scale with the following criteria: * Score 0: Ability to raise extended arm to 90° for 2 seconds.
* Score 1: Ability to flex elbow and move fingers, unable to raise extended arm.
* Score 2: Unable to flex elbow but able to move fingers.
* Score 3: Complete motor block of arm, elbow, and finger.
Postoperative assessment of sensory block was evaluated by pinprick sensation and motor function was again assessed by modified Bromage scale.
The successful anesthetic management of our patient with HD using a supraclavicular brachial plexus block for tendon transfer surgery highlights several important considerations in the perioperative care of patients with this rare neurological condition. This case demonstrates the efficacy and advantages of regional anesthesia techniques in patients where GA might present significant risks.
HD, characterized by its unique pathophysiology involving dynamic compression of the cervical spinal cord during neck flexion, presents specific challenges for anesthesiologists.11 The forward displacement of the posterior dural sac during neck flexion can potentially compromise the spinal cord, making airway management under GA particularly concerning.12 Our approach avoided this risk entirely by utilizing regional anesthesia.
The choice of supraclavicular brachial plexus block in our patient was supported by several factors. First, this technique provides excellent anesthesia for procedures involving the entire upper extremity, including the shoulder.13 Vermeylen et al. demonstrated in their comparative study that supraclavicular blocks offer a more consistent spread to all trunks of the brachial plexus compared to other approaches, making it ideal for complex hand procedures such as tendon transfers.14 Second, the avoidance of neck manipulation during block placement is particularly advantageous in patients with HD.
Ultrasound guidance played a crucial role in our block performance. Perlas et al. found that ultrasound-guided supraclavicular blocks are associated with higher success rates (97.2%) and lower complication rates compared to landmark-based techniques.15 In our patient, ultrasound visualization allowed precise needle placement, minimizing the risk of complications such as pneumothorax or vascular puncture, which are especially important considerations in patients with neuromuscular disorders who may have altered anatomy or compromised respiratory function.
The anesthetic drug selection and dosing in our case merit discussion. We utilized a combination of ropivacaine 0.75% 15 mL and lidocaine 2% with adrenaline to balance onset time with duration of effect and 8mg of dexamethasone to prolong the duration of action .Casati et al. demonstrated that 0.75% ropivacaine provides effective surgical anesthesia lasting 8-12 hours, suitable for prolonged procedures such as tendon transfers.16 The addition of lidocaine accelerated the onset of sensory and motor blockade, as shown by Cuvillon et al., who reported a reduction in onset time from 15 min to 10 min with such combinations.17 Our experience aligned with these findings, as complete sensory blockade was achieved within 12 min.
The multimodal analgesia approach employed in our case, combining regional anesthesia with non-opioid analgesics, is supported by evidence from Zhao et al. (2021), who demonstrated superior pain control and reduced opioid consumption in upper extremity surgeries managed with brachial plexus blocks versus GA.18 This approach is particularly beneficial in avoiding opioid-related side effects such as respiratory depression, which could be problematic in patients with neuromuscular disorders.
Postoperative follow-up revealed excellent pain control and patient satisfaction, consistent with findings from Liu et al., who reported significantly higher satisfaction scores with regional versus GA for upper limb procedures (95% vs. 73%).19 Our patient reported minimal pain (VAS score 2/10) in the immediate postoperative period and required only acetaminophen for pain management during the first 24 hours.
A limitation in our case was the patient's initial anxiety about remaining awake during surgery, which required additional preoperative counselling and education. This highlights the importance of thorough psychological preparation when planning regional anesthesia.
This case report highlights the successful implementation of a supraclavicular brachial plexus block as the primary anesthetic technique for tendon transfer surgery in a patient with HD. Our experience demonstrates that regional anesthesia may be considered as a viable alternative in selected patients with HD undergoing upper limb surgeries as it offers significant advantages in this patient population by avoiding neck manipulation and its associated risks of cervical cord compression, providing excellent surgical conditions, ensuring hemodynamic stability, and delivering superior postoperative pain control. The ultrasound-guided supraclavicular approach allowed precise needle placement, minimizing potential complications while achieving complete sensory and motor blockade. The patient's ability to maintain a comfortable neck position throughout the procedure and the continuous neurological monitoring afforded by his awake status provided additional safety benefits. This case underscores the importance of tailored anesthetic planning for patients with rare neurological disorders and supports the consideration of regional anesthesia techniques as primary options for appropriate surgeries in patients with Hirayama disease.
5. Conflict of interest
All authors declare that there was no conflict of interest.
6. Ethical issues
The study utilized the hospital resources only, and no external or industry funding was involved. Patient’s written consent was obtained to use his pictures and the disease history for the academic interest.
7. Authors’ contribution
Both authors contributed in data accumulation and preparation of this manuscript.
Authors affiliations:
1. Bhavini Shah, Dr. D. Y. Patil Medical College Hospital & Research Centre. Pune, Maharashtra, India; Email: drbhavinishah71@gmail.co
2. Pragya Pramanik, Dr. D. Y. Patil Medical College Hospital & Research Centre. Pune, Maharashtra, India; Email: pramanik.pragya124@gmail.com
Correspondence: Pragya Pramanik, Email: pramanik.pragya124@gmail.com
ABSTRACT
Hirayama disease is a rare cervical myelopathy characterized by dynamic compression of the spinal cord during neck flexion, presenting unique challenges for anesthetic management. This case report describes the successful use of a supraclavicular brachial plexus block for tendon transfer surgery in a patient with Hirayama disease (HD).
A 34-year-old male with a 10-year history of progressive left hand weakness and atrophy, diagnosed with HD, was scheduled for tendon transfer surgery to improve hand function. Given concerns about cervical spine manipulation and potential cord compression with general anesthesia, a supraclavicular brachial plexus block was selected as the primary anesthetic technique. Ultrasound-guided block was performed using a combination of 0.75% ropivacaine 15mL and 2% lidocaine 10 mL, and 8mg of dexamethasone given achieving complete sensory and motor blockade within 12 min. The patient maintained a comfortable neutral neck position throughout the procedure. Surgery proceeded uneventfully with excellent surgical conditions and hemodynamic stability. Postoperatively, the patient reported minimal pain (VAS score 2/10) requiring only acetaminophen for the first 24 hours, expressed high satisfaction with the anesthetic technique, and was discharged on the second postoperative day without complications.
Conclusion: Supraclavicular brachial plexus block represents an effective and safe anesthetic technique for patients with HD undergoing upper limb procedures, avoiding risks associated with neck manipulation during general anesthesia while providing excellent surgical conditions and postoperative pain control. This approach should be considered as a primary option for appropriate surgeries in this patient population.
Abbreviations: BMI: Body Mass Index, HD: Hirayama Disease, VAS: Visual Analog Scale,
Keywords: Hirayama Disease; USG Guided; Supraclavicular Brachial Plexus Block; Tendon Transfer
Citation: Shah B, Pramanik P. Anesthetic management for tendon transfer in a patient with monomelic amyotrophy (Hirayama Disease): A case report. Anaesth. pain intensive care 2025;29(5):428-432. DOI: 10.35975/apic.v29i5.2864
Received: April 10, 2025; Revised: May 07, 2025; Accepted: May 09, 2025
1. INTRODUCTION
Hirayama disease (HD), also known as juvenile muscular atrophy of the distal upper extremity, is a rare, self-limiting cervical myelopathy characterized by asymmetric weakness and wasting of muscles innervated by the C7, C8, and T1 nerve roots, predominantly affecting young males.1,2 First described by Hirayama in 1959, the condition typically manifests in the second or third decade of life with insidious onset of unilateral or bilateral distal upper limb weakness and atrophy, often affecting the hand and forearm musculature.3
The pathophysiology is associated with dynamic cord compression during neck flexion due to forward displacement of the posterior dural sac and compression of the cervical cord against vertebral bodies.4 This unique pathology presents distinct challenges in perioperative management, particularly concerning positioning and airway management during anesthesia.5
Tendon transfer procedures are commonly performed to improve hand function in patients with HD who have residual muscle weakness despite disease stabilization.6 These reconstructive surgeries aim to restore functional balance by transferring functioning tendons to replace the action of paralyzed muscles.7
The anesthetic management of patients with HD requires careful consideration due to potential cervical spine instability and the risk of exacerbating cord compression during manipulation of the neck.8 Regional anesthesia techniques, particularly peripheral nerve blocks, offer considerable advantages in such cases by avoiding airway manipulation and providing excellent postoperative analgesia.9
The supraclavicular brachial plexus block represents an effective anesthetic approach for upper limb surgeries, providing dense and reliable anesthesia with rapid onset. This technique may be particularly beneficial in patients with HD undergoing tendon transfer procedures, as it circumvents the need for neck manipulation associated with general anesthesia (GA) and neuraxial techniques.10
This case report describes the successful anesthetic management using a USG guided supraclavicular block for tendon transfer surgery in a patient with HD, highlighting the considerations, techniques, and outcomes relevant to anesthetic practice in this rare neurological condition.
2. CASE REPORT
A 34-year-old male presented to our tertiary care hospital with progressive weakness and wasting of the left hand musculature, particularly affecting the intrinsic muscles, that had gradually worsened over the past decade. Despite multiple consultations and parallel therapies including physiotherapy and neurological rehabilitation, the patient experienced minimal improvement in his condition. He reported increasing difficulty with fine motor tasks such as buttoning shirts, typing, and gripping objects, significantly impacting his professional life as a software engineer.
The patient's medical history was remarkable for an initial misdiagnosis of cervical radiculopathy at a local clinic, which delayed appropriate treatment for several years. Upon comprehensive neurological evaluation at our institution two years prior, electromyography studies revealed denervation patterns in the C7-T1 distribution, predominantly affecting the left hand. Subsequent dynamic MRI of the cervical spine in flexion demonstrated the characteristic forward displacement of the posterior dural sac with flattening of the cervical cord against the vertebral bodies, confirming the diagnosis of HD.
Interestingly, the patient had noticed that his symptoms worsened during cold weather and after prolonged periods of neck flexion while working on his computer. He had independently developed adaptive strategies, including using voice recognition software and specialized ergonomic equipment, to continue his work. The patient was psychologically resilient but increasingly frustrated by the functional limitations imposed by his condition.
Upon preoperative assessment, the patient was classified as ASA physical status II with a metabolic equivalent of task (METs) score greater than 4, indicating good functional capacity. His preoperative bedside pfts and neurological status were normal. His power was 5/5 in both upper and lower limbs. His vital signs were within normal limits: blood pressure 118/76 mmHg, heart rate 72 beats / min, respiratory rate 14 breaths / min, and oxygen saturation 99% on room air. His height was 175 cm tall and weighing 60 kg (BMI 19.6 kg/m²), the patient appeared slightly underweight but well-nourished. Laboratory investigations, including complete hemogram, liver function tests, renal function tests, serum electrolytes, and coagulation profile (bleeding time and clotting time were within normal ranges. Chest X-ray revealed increased bronchovascular markings and ECG revealed normal sinus rhythm.

Figure 1: Increased vascular markings in the hilums
Airway examination revealed a Mallampati class II airway with normal thyromental distance and adequate mouth opening. Notably, the patient demonstrated limited cervical spine mobility, particularly during flexion, which he attributed to a conscious effort to avoid positions that exacerbated his symptoms. This finding was particularly significant for anesthetic planning, as it raised concerns about potential difficulties with conventional laryngoscopy and intubation if GA was to be employed.
After comprehensive multidisciplinary discussion involving the hand surgeon, neurologist, and anesthesia team, the patient was scheduled for tendon transfer surgery to improve hand function by redistributing the activity of functioning muscles to restore the actions of paralyzed ones. The planned procedure involved transfer of the pronator teres to extensor carpi radialis brevis, and flexor carpi radialis to finger extensors.
Given the patient's diagnosis, concerns regarding cervical spine manipulation, and the nature of the procedure, the anesthesia team proposed a supraclavicular brachial plexus block as the primary anesthetic technique. The patient, initially apprehensive about remaining awake during the procedure, was educated about the benefits of regional anesthesia in his specific case and the option for conscious sedation if needed. After thorough discussion and addressing his concerns, he provided informed consent for the proposed anesthetic plan.
Patient was instructed to remain nil by mouth from midnight prior to surgery. On arrival in the preoperative room, baseline vital parameters including pulse rate, non-invasive blood pressure, ECG and oxygen saturation were recorded. Peripheral venous access was established and intravenous fluid administration was initiated.
In the operation theatre, standard monitoring including electrocardiography, non-invasive blood pressure, and pulse oximetry were attached, baseline parameters including heart rate, systolic blood pressure, diastolic blood pressure, mean arterial pressure, and oxygen saturation were recorded. The patient was put on Hudson mask on 4 litres of oxygen and inj midazolam 0.02 mg/kg and inj fentanyl 2 µg/kg was administered to alleviate anxiety and for smooth conduction of the procedure.
The supraclavicular brachial plexus block was performed under ultrasound guidance using a Hitachi Arietta S70 machine with a linear probe. The patient was positioned supine with a small bolster under the shoulder, and the head turned 45 degrees to the contralateral side. After aseptic preparation, the supraclavicular fossa was scanned to identify key anatomical structures including the subclavian artery, first rib, pleura, and brachial plexus cluster. Local skin infiltration was administered before advancing a 22G long needle from lateral to medial axis under ultrasound guidance. A 22 1.5G hypodermic needle was inserted using an in-plane technique and half of 15 mL of 0.75% ropivacaine and 10 mL of 2% lignocaine with adrenaline was given and 8mg of dexamethasone was administered to potentiate the action and prolong the duration of the drug and then the needle was repositioned cranially towards the neural cluster for administration of the remaining volume, maintaining careful aspiration technique throughout the procedure.
Sensory block was evaluated using pinprick sensation, while motor block was assessed using a modified Bromage scale with the following criteria: * Score 0: Ability to raise extended arm to 90° for 2 seconds.
* Score 1: Ability to flex elbow and move fingers, unable to raise extended arm.
* Score 2: Unable to flex elbow but able to move fingers.
* Score 3: Complete motor block of arm, elbow, and finger.
Postoperative assessment of sensory block was evaluated by pinprick sensation and motor function was again assessed by modified Bromage scale.
3. DISCUSSION
The successful anesthetic management of our patient with HD using a supraclavicular brachial plexus block for tendon transfer surgery highlights several important considerations in the perioperative care of patients with this rare neurological condition. This case demonstrates the efficacy and advantages of regional anesthesia techniques in patients where GA might present significant risks.
HD, characterized by its unique pathophysiology involving dynamic compression of the cervical spinal cord during neck flexion, presents specific challenges for anesthesiologists.11 The forward displacement of the posterior dural sac during neck flexion can potentially compromise the spinal cord, making airway management under GA particularly concerning.12 Our approach avoided this risk entirely by utilizing regional anesthesia.
The choice of supraclavicular brachial plexus block in our patient was supported by several factors. First, this technique provides excellent anesthesia for procedures involving the entire upper extremity, including the shoulder.13 Vermeylen et al. demonstrated in their comparative study that supraclavicular blocks offer a more consistent spread to all trunks of the brachial plexus compared to other approaches, making it ideal for complex hand procedures such as tendon transfers.14 Second, the avoidance of neck manipulation during block placement is particularly advantageous in patients with HD.
Ultrasound guidance played a crucial role in our block performance. Perlas et al. found that ultrasound-guided supraclavicular blocks are associated with higher success rates (97.2%) and lower complication rates compared to landmark-based techniques.15 In our patient, ultrasound visualization allowed precise needle placement, minimizing the risk of complications such as pneumothorax or vascular puncture, which are especially important considerations in patients with neuromuscular disorders who may have altered anatomy or compromised respiratory function.
The anesthetic drug selection and dosing in our case merit discussion. We utilized a combination of ropivacaine 0.75% 15 mL and lidocaine 2% with adrenaline to balance onset time with duration of effect and 8mg of dexamethasone to prolong the duration of action .Casati et al. demonstrated that 0.75% ropivacaine provides effective surgical anesthesia lasting 8-12 hours, suitable for prolonged procedures such as tendon transfers.16 The addition of lidocaine accelerated the onset of sensory and motor blockade, as shown by Cuvillon et al., who reported a reduction in onset time from 15 min to 10 min with such combinations.17 Our experience aligned with these findings, as complete sensory blockade was achieved within 12 min.
The multimodal analgesia approach employed in our case, combining regional anesthesia with non-opioid analgesics, is supported by evidence from Zhao et al. (2021), who demonstrated superior pain control and reduced opioid consumption in upper extremity surgeries managed with brachial plexus blocks versus GA.18 This approach is particularly beneficial in avoiding opioid-related side effects such as respiratory depression, which could be problematic in patients with neuromuscular disorders.
Postoperative follow-up revealed excellent pain control and patient satisfaction, consistent with findings from Liu et al., who reported significantly higher satisfaction scores with regional versus GA for upper limb procedures (95% vs. 73%).19 Our patient reported minimal pain (VAS score 2/10) in the immediate postoperative period and required only acetaminophen for pain management during the first 24 hours.
A limitation in our case was the patient's initial anxiety about remaining awake during surgery, which required additional preoperative counselling and education. This highlights the importance of thorough psychological preparation when planning regional anesthesia.
4. CONCLUSION
This case report highlights the successful implementation of a supraclavicular brachial plexus block as the primary anesthetic technique for tendon transfer surgery in a patient with HD. Our experience demonstrates that regional anesthesia may be considered as a viable alternative in selected patients with HD undergoing upper limb surgeries as it offers significant advantages in this patient population by avoiding neck manipulation and its associated risks of cervical cord compression, providing excellent surgical conditions, ensuring hemodynamic stability, and delivering superior postoperative pain control. The ultrasound-guided supraclavicular approach allowed precise needle placement, minimizing potential complications while achieving complete sensory and motor blockade. The patient's ability to maintain a comfortable neck position throughout the procedure and the continuous neurological monitoring afforded by his awake status provided additional safety benefits. This case underscores the importance of tailored anesthetic planning for patients with rare neurological disorders and supports the consideration of regional anesthesia techniques as primary options for appropriate surgeries in patients with Hirayama disease.
5. Conflict of interest
All authors declare that there was no conflict of interest.
6. Ethical issues
The study utilized the hospital resources only, and no external or industry funding was involved. Patient’s written consent was obtained to use his pictures and the disease history for the academic interest.
7. Authors’ contribution
Both authors contributed in data accumulation and preparation of this manuscript.
8. REFERENCES
- Hirayama K, Tomonaga M, Kitano K, Yamada T, Kojima S, Arai K. Focal cervical poliopathy causing juvenile muscular atrophy of distal upper extremity: a pathological study. J Neurol Neurosurg Psychiatry. 2018;58(1):56–64. [PubMed] DOI: 1136/jnnp.50.3.285
- Zhou B, Chen L, Fan D, Zhou D. Clinical features of Hirayama disease in mainland China. Amyotroph Lateral Scler. 2020;11(1-2):133–9. [PubMed] DOI: 3109/17482960902912407
- Hirayama K. Juvenile muscular atrophy of distal upper extremity (Hirayama disease). Intern Med. 2019;39(4):283–90. [PubMed] DOI: 2169/internalmedicine.39.283
- Huang YL, Chen CJ. Hirayama disease. Neuroimaging Clin N Am. 2011;21:939–50. [PubMed] DOI: 1016/j.nic.2011.07.009
- Hashimoto O, Asada M, Ohta M, Kuroiwa Y. Clinical observations of juvenile non-progressive muscular atrophy localized in hand and forearm. J Neurol. 2018;225(1):33–42. [PubMed] DOI: 1007/BF00313354
- Hua C, Bhai S, Cheng J, Hinojosa J, Wilson L, Lubinus M, et al. Tendon transfers to improve grip and pinch in patients with sporadic inclusion body myositis. Plast Reconstr Surg Glob Open. 2023;11(11):e5418. [PubMed] DOI: 1097/GOX.0000000000005418
- Fitoussi F, Bachy M. Tendon lengthening and transfer. Orthop Traumatol Surg Res. 2015;101:S149–57. [PubMed] DOI: 1016/j.otsr.2014.07.033
- Reddy A, Varma P, Barik AK, Narayan V. Anesthetic challenges in a patient with Hirayama disease with quadriparesis and autonomic dysfunction undergoing cervical spine surgery. J Neurosci Rural Pract. 2024;15(1):137–9. [PubMed] DOI: 25259/JNRP_224_2023
- Lee LA, Posner KL, Domino KB, Caplan RA, Cheney FW. Injuries associated with regional anesthesia in the 1980s and 1990s: a closed claims analysis. Anesthesiology. 2019;101(1):143–52. [PubMed] DOI: 1097/00000542-200407000-00023
- Jeon DG, Kim WI. Cases series: ultrasound-guided supraclavicular block in 105 patients. Korean J Anesthesiol. 2010 Mar;58(3):267-71. [PubMed] DOI: 4097/kjae.2010.58.3.267
- Hirayama K. Juvenile muscular atrophy of distal upper extremity (Hirayama disease): focal cervical ischemic poliomyelopathy. Neuropathology. 2020;40(1):181–90. [PubMed] DOI: 1046/j.1440-1789.2000.00305.x
- Xu X, Han H, Gao H, Hou C, Fan D, Fu Y, et al. The increased range of cervical flexed motion detected by radiographs in Hirayama disease. Eur J Radiol. 2011;78(1):82-6. [PubMed] DOI: 1016/j.ejrad.2010.08.012
- Neal JM, Gerancher JC, Hebl JR, Ilfeld BM, McCartney CJ, Franco CD, et al. Upper extremity regional anesthesia: essentials of our current understanding. Reg Anesth Pain Med. 2020;34(2):134–70. [PubMed] DOI: 1097/AAP.0b013e31819624eb
- Vermeylen K, Engelen S, Sermeus L, Soetens F, Van de Velde M. Supraclavicular brachial plexus blocks: review and current practice. Acta Anaesthesiol Belg. 2019;63(1):15–21. [PubMed]
- Perlas A, Lobo G, Lo N, Brull R, Chan VW, Karkhanis R. Ultrasound-guided supraclavicular block: outcome of 510 consecutive cases. Reg Anesth Pain Med. 2020;34(2):171–6. [PubMed] DOI: 1097/AAP.0b013e31819a3f81
- Casati A, Fanelli G, Albertin A, Deni F, Anelati D, Antonino FA, et al. Interscalene brachial plexus anesthesia with either 0.5% ropivacaine or 0.5% bupivacaine. Minerva Anestesiol. 2019;66(1-2):39–44. [PubMed] DOI: 1097/AAP.0b013e31819a3f81
- Cuvillon P, Nouvellon E, Ripart J, Boyer JC, Dehour L, Mahamat A, et al. A comparison of the pharmacodynamics and pharmacokinetics of bupivacaine, ropivacaine (with epinephrine) and their equal volume mixtures with lidocaine used for femoral and sciatic nerve blocks. Anesth Analg. 2019;109(5):1518–23. [PubMed]DOI: 1213/ane.0b013e31819237f8
- Zhao SZ, Chung F, Hanna DB, Raymundo AL, Cheung RY, Chen C. Dose-response relationship between opioid use and adverse effects after ambulatory surgery. J Pain Symptom Manage. 2021;38(3):422–30. [PubMed] DOI: 1016/j.jpainsymman.2003.11.001
- Liu SS, Strodtbeck WM, Richman JM, Wu CL. A comparison of regional versus general anesthesia for ambulatory anesthesia: a meta-analysis of randomized controlled trials. Anesth Analg. 2018;101(6):1634–42. [PubMed] DOI: 1213/01.ANE.0000180829.70036.4F