Liaquat Ali 1, Umer Ali 2, Sana Nasir 3, Noor Fatima 4, Ali Ahmed Qureshi 5
Authors affiliations:
This case report presents the first documented use of a Bier block (intravenous regional anesthesia) for lower limb surgery in Pakistan, detailing its application in a 39-year-old male undergoing the removal of a dynamic compression plate from his left tibia. The procedure utilized a total of 50 mL of lignocaine, achieving effective analgesia throughout the surgery, with the patient reporting minimal discomfort. This case underscores the efficacy and safety of the Bier block as a viable alternative to general anesthesia for orthopedic procedures, addressing a significant gap in the literature regarding its use in lower limb surgeries. The successful outcome highlights the potential for improved postoperative pain management and sets a precedent for further research and clinical practice in this area.
Abbreviations: IVRA: intravenous regional anesthesia, MET score: Metabolic Equivalent of Task score, PACU: Post-Anesthesia Care Unit, VAS: Visual Analog Scale
Keywords: Lower Extremity; Orthopedic Procedures; Tourniquets; Compartment Syndromes; IVRA
Citation: Ali L, Ali U, Qureshi AA, Nasir S, Fatima N. An uncommon approach of Bier block for tibial surgery; A case report. Anaesth. pain intensive care 2025;29(3):695-698. DOI: 10.35975/apic.v29i3.2780
Received: October 23, 2024; Revised: February 05, 2025; Accepted: March 23, 2025
While many institutions may have used similar methods, there is a notable lack of published case reports or studies on the use of Bier block in lower limb surgeries, particularly tibial surgery, within Pakistani medical literature. Additionally, there is very limited data available in the international literature on this subject as well. This case report presents the first documented use of a Bier block for a lower limb surgery in Pakistan.
In the recent years, regional anesthesia techniques have evolved to enhance patient comfort and surgical outcomes, particularly in orthopedic procedures. One such technique is the Bier block, or intravenous regional anesthesia (IVRA), which has been effectively used in various upper and lower limb surgeries.1,2 Bier block offers anesthesia to a limb, distal to the tourniquet, without requiring direct injection at the surgical site.3 IVRA remains widely used in many countries today, particularly in emergency rooms for outpatients and for high-risk patients who cannot undergo general anesthesia. It provides a good balance of risks and benefits, is cost-effective, ensures adequate muscle relaxation, and has a quick onset and recovery. Advancements in monitoring techniques, specialized personnel, and enhanced emergency equipment have further increased the safety of IVRA. As an uncomplicated and visually appealing technique that requires minimal extra equipment, it has gained global acceptance. Its ability to create a bloodless surgical field with the use of a tourniquet, along with shorter recovery times in the post-anesthesia care unit (PACU) and a lower risk of nausea, makes it especially valuable for outpatient anesthesia.4 However, it has some adverse effects too; anesthesia and pain relief are effective only while the tourniquet is inflated, once the cuff is deflated, patients experience a loss of anesthesia and significant postoperative pain.5
We present the case of a 39-year-old male, who attended the pre-anesthesia clinic for evaluation before the removal of a dynamic compression plate from his left tibia. The plate had been inserted approximately five years earlier following a road traffic accident. The patient had no known comorbidities, and his functional status was Metabolic Equivalent of Task (MET) score > 4. He was classified as Mallampati grade 1. All of his laboratory results were within normal limits. His systemic examination was unremarkable, and there was no history of any drug allergies. The patient was assessed as ASA 1, and the plan was to proceed with the surgery under a Bier block.
The patient was counseled about the procedure, including its potential risks and benefits, and he consented to proceed. Standard ASA monitoring was applied, and an 18G IV line was secured in the right arm. Another 18G IV line was placed on the dorsal aspect of the left foot, with patency confirmed via a normal saline flush. Two pneumatic tourniquets were placed on the left thigh, well above the surgical site, and their functionality was tested (Figure 1).
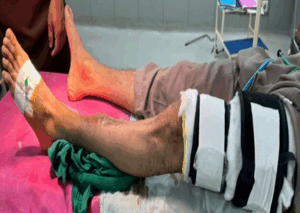
Figure 1: Two pneumatic tourniquets placed on the left thigh of the patient
According to protocol, an Esmarch bandage was applied from distal to proximal, ensuring adequate exsanguination of the limb. The proximal tourniquet cuff was then inflated to above the patient's systolic blood pressure. After lowering the limb, the Esmarch bandage was removed. Tourniquet functionality was confirmed by the absence of distal pulses and the pale appearance of the limb compared to the contralateral side.
An initial dose of 30 mL of 0.5% plain lignocaine was administered in the cannula on the foot. Adequate analgesia was achieved and confirmed by a pinprick test on the lower leg. After 10 min, an additional 20 mL of 1% lignocaine was administered to complete the required dose and volume.
The procedure proceeded smoothly for the first 20 min, after which the patient reported pain at the tourniquet site with a Visual Analog Scale (VAS) score of 3/10. At this point, the distal tourniquet was inflated, and its functionality was confirmed, followed by the slow deflation of the proximal cuff. The patient was also sedated with 1 mg of midazolam.
The total surgical time was approximately 80 min, during which the patient experienced no further pain (VAS 0/10). At the conclusion of the surgery, the distal tourniquet was deflated for 10 sec, then re-inflated for another 2 min to prevent any risk of local anesthetic systemic toxicity. After confirming there were no signs of toxicity, the cuff was fully deflated. There were no signs and symptoms of compartment syndrome during the intraoperative and postoperative period. The patient was monitored in the PACU for one hour. His VAS remained at 0/10, and he was able to move his leg immediately postoperatively.
Despite numerous advancements, literature on the use of Bayer block in the lower limb surgery remains limited worldwide, with a striking absence in Pakistani medical literature, where no case reports or studies have been published to date on this subject. This case emphasizes the necessity for more extensive studies to evaluate the effectiveness and safety of Bier blocks in lower limb surgeries across diverse healthcare settings. By addressing this gap, future research can enhance the application and outcomes of regional anesthesia techniques in orthopedic practice, ultimately benefiting patient care on a global scale.
The Bier block, or IVRA was first described by August Bier in 1908.6 It is a reliable alternative to general anesthesia for short-duration surgeries on the extremities, particularly for lower limb procedures. It may be used for various lower extremity procedures, but it requires larger volumes of local anesthetic solutions due to the size disparity between the upper and lower extremities.7
While IVRA has been associated with an increased incidence of compartment syndrome when treating tibial shaft fractures, studies show that in atraumatic limbs simulated IVRA does not significantly increase tissue pressure, indicating its potential safety in carefully selected cases.7 This is in accordance with our case involving the Bier block for tibial plate removal, where there were no signs of compartment syndrome during either the intraoperative or postoperative periods.
Adjuncts to local anesthetics for IVRA include opioids (e.g., fentanyl 100-200 μg, Tramadol 100 mg) for pain relief; clonidine to enhance analgesia; and muscle relaxants (e.g., atracurium 3 mg) for fracture reduction. NSAIDs (e.g., ketorolac 0.3 mg/kg) improve postoperative analgesia and prolong tourniquet tolerance, while sodium bicarbonate enhances local anesthetic effectiveness. The addition of potassium and temperature alterations may also improve analgesia. These adjuncts contribute to better postoperative outcomes during IVRA.7,8 Additionally, it can be used to treat complex regional pain syndromes.9
Yari et al. (2020) highlighted the benefits of the Bier block, including minimized distortion of soft tissue planes and a reduced requirement for general anesthesia.10 Our case effectively demonstrates these advantages, as patient remained pain free (VAS 0/10) throughout the surgery, eliminating the need for both the general as well as other forms of regional anesthesia. It also confirms the Bier block's applicability for tibial surgery, paving the way for further exploration in lower limb applications.
Khanduri (2008) discusses a broad spectrum of regional anesthesia techniques utilized in orthopedic surgeries, asserting that regional anesthesia can achieve high success rates and patient satisfaction when administered skillfully.11 Our findings reinforce this perspective, as our patient remained exceptionally comfortable and pain-free throughout the procedure, requiring no additional analgesia. This highlights the Bier block's capability to provide effective anesthesia and postoperative pain relief for lower limb surgeries, in alignment with existing studies demonstrating its reliability and patient comfort.
The successful implementation of the Bier block for tibial surgery in this case, supports its efficacy and safety as a regional anesthesia technique for lower limb procedures. The current literature and recent advancements in regional anesthesia highlight the importance of continued research and refinement. Bier blocks in lower limb surgeries offers patient satisfaction, reduced PACU and hospital stay and improved surgical outcomes.
5. Conflict of interest
All authors declare that there was no conflict of interest.
6. Consent for publ ication
Not applicable.
7. Authors’ contribution
All authors took part in the literature search, conduct of the case and drafting the manuscript.
Authors affiliations:
- Liaquat Ali, Professor & Head, Department of Anesthesiology, Intensive Care & Pain Management, Fauji Foundation Hospital, Rawalpindi / Foundation University, Islamabad, Pakistan; Email: liaquatanaes@gmail.com
- Umer Ali, Assistant Professor, Department of Anesthesiology, Intensive Care & Pain Management, Fauji Foundation Hospital, Rawalpindi / Foundation University, Islamabad, Pakistan; Email: umer6oct@gmail.com
- Sana Nasir, Department of Anesthesiology, Intensive Care & Pain Management, Fauji Foundation Hospital, Rawalpindi / Foundation University, Islamabad, Pakistan; Email: sananasir1418@gmail.com
- Noor Fatima, Department of Anesthesiology, Intensive Care & Pain Management, Fauji Foundation Hospital, Rawalpindi / Foundation University, Islamabad, Pakistan; Email: noorfatima78651@gmail.com
- Ali Ahmed Qureshi, Department of Anesthesiology, Intensive Care & Pain Management, Fauji Foundation Hospital, Rawalpindi / Foundation University, Islamabad, Pakistan; Email: aliahmed.moq@gmail.com
ABSTRACT
This case report presents the first documented use of a Bier block (intravenous regional anesthesia) for lower limb surgery in Pakistan, detailing its application in a 39-year-old male undergoing the removal of a dynamic compression plate from his left tibia. The procedure utilized a total of 50 mL of lignocaine, achieving effective analgesia throughout the surgery, with the patient reporting minimal discomfort. This case underscores the efficacy and safety of the Bier block as a viable alternative to general anesthesia for orthopedic procedures, addressing a significant gap in the literature regarding its use in lower limb surgeries. The successful outcome highlights the potential for improved postoperative pain management and sets a precedent for further research and clinical practice in this area.
Abbreviations: IVRA: intravenous regional anesthesia, MET score: Metabolic Equivalent of Task score, PACU: Post-Anesthesia Care Unit, VAS: Visual Analog Scale
Keywords: Lower Extremity; Orthopedic Procedures; Tourniquets; Compartment Syndromes; IVRA
Citation: Ali L, Ali U, Qureshi AA, Nasir S, Fatima N. An uncommon approach of Bier block for tibial surgery; A case report. Anaesth. pain intensive care 2025;29(3):695-698. DOI: 10.35975/apic.v29i3.2780
Received: October 23, 2024; Revised: February 05, 2025; Accepted: March 23, 2025
1. INTRODUCTION
While many institutions may have used similar methods, there is a notable lack of published case reports or studies on the use of Bier block in lower limb surgeries, particularly tibial surgery, within Pakistani medical literature. Additionally, there is very limited data available in the international literature on this subject as well. This case report presents the first documented use of a Bier block for a lower limb surgery in Pakistan.
In the recent years, regional anesthesia techniques have evolved to enhance patient comfort and surgical outcomes, particularly in orthopedic procedures. One such technique is the Bier block, or intravenous regional anesthesia (IVRA), which has been effectively used in various upper and lower limb surgeries.1,2 Bier block offers anesthesia to a limb, distal to the tourniquet, without requiring direct injection at the surgical site.3 IVRA remains widely used in many countries today, particularly in emergency rooms for outpatients and for high-risk patients who cannot undergo general anesthesia. It provides a good balance of risks and benefits, is cost-effective, ensures adequate muscle relaxation, and has a quick onset and recovery. Advancements in monitoring techniques, specialized personnel, and enhanced emergency equipment have further increased the safety of IVRA. As an uncomplicated and visually appealing technique that requires minimal extra equipment, it has gained global acceptance. Its ability to create a bloodless surgical field with the use of a tourniquet, along with shorter recovery times in the post-anesthesia care unit (PACU) and a lower risk of nausea, makes it especially valuable for outpatient anesthesia.4 However, it has some adverse effects too; anesthesia and pain relief are effective only while the tourniquet is inflated, once the cuff is deflated, patients experience a loss of anesthesia and significant postoperative pain.5
2. CASE REPORT
We present the case of a 39-year-old male, who attended the pre-anesthesia clinic for evaluation before the removal of a dynamic compression plate from his left tibia. The plate had been inserted approximately five years earlier following a road traffic accident. The patient had no known comorbidities, and his functional status was Metabolic Equivalent of Task (MET) score > 4. He was classified as Mallampati grade 1. All of his laboratory results were within normal limits. His systemic examination was unremarkable, and there was no history of any drug allergies. The patient was assessed as ASA 1, and the plan was to proceed with the surgery under a Bier block.
The patient was counseled about the procedure, including its potential risks and benefits, and he consented to proceed. Standard ASA monitoring was applied, and an 18G IV line was secured in the right arm. Another 18G IV line was placed on the dorsal aspect of the left foot, with patency confirmed via a normal saline flush. Two pneumatic tourniquets were placed on the left thigh, well above the surgical site, and their functionality was tested (Figure 1).

Figure 1: Two pneumatic tourniquets placed on the left thigh of the patient
According to protocol, an Esmarch bandage was applied from distal to proximal, ensuring adequate exsanguination of the limb. The proximal tourniquet cuff was then inflated to above the patient's systolic blood pressure. After lowering the limb, the Esmarch bandage was removed. Tourniquet functionality was confirmed by the absence of distal pulses and the pale appearance of the limb compared to the contralateral side.
An initial dose of 30 mL of 0.5% plain lignocaine was administered in the cannula on the foot. Adequate analgesia was achieved and confirmed by a pinprick test on the lower leg. After 10 min, an additional 20 mL of 1% lignocaine was administered to complete the required dose and volume.
The procedure proceeded smoothly for the first 20 min, after which the patient reported pain at the tourniquet site with a Visual Analog Scale (VAS) score of 3/10. At this point, the distal tourniquet was inflated, and its functionality was confirmed, followed by the slow deflation of the proximal cuff. The patient was also sedated with 1 mg of midazolam.
The total surgical time was approximately 80 min, during which the patient experienced no further pain (VAS 0/10). At the conclusion of the surgery, the distal tourniquet was deflated for 10 sec, then re-inflated for another 2 min to prevent any risk of local anesthetic systemic toxicity. After confirming there were no signs of toxicity, the cuff was fully deflated. There were no signs and symptoms of compartment syndrome during the intraoperative and postoperative period. The patient was monitored in the PACU for one hour. His VAS remained at 0/10, and he was able to move his leg immediately postoperatively.
3. DISCUSSION
Despite numerous advancements, literature on the use of Bayer block in the lower limb surgery remains limited worldwide, with a striking absence in Pakistani medical literature, where no case reports or studies have been published to date on this subject. This case emphasizes the necessity for more extensive studies to evaluate the effectiveness and safety of Bier blocks in lower limb surgeries across diverse healthcare settings. By addressing this gap, future research can enhance the application and outcomes of regional anesthesia techniques in orthopedic practice, ultimately benefiting patient care on a global scale.
The Bier block, or IVRA was first described by August Bier in 1908.6 It is a reliable alternative to general anesthesia for short-duration surgeries on the extremities, particularly for lower limb procedures. It may be used for various lower extremity procedures, but it requires larger volumes of local anesthetic solutions due to the size disparity between the upper and lower extremities.7
While IVRA has been associated with an increased incidence of compartment syndrome when treating tibial shaft fractures, studies show that in atraumatic limbs simulated IVRA does not significantly increase tissue pressure, indicating its potential safety in carefully selected cases.7 This is in accordance with our case involving the Bier block for tibial plate removal, where there were no signs of compartment syndrome during either the intraoperative or postoperative periods.
Adjuncts to local anesthetics for IVRA include opioids (e.g., fentanyl 100-200 μg, Tramadol 100 mg) for pain relief; clonidine to enhance analgesia; and muscle relaxants (e.g., atracurium 3 mg) for fracture reduction. NSAIDs (e.g., ketorolac 0.3 mg/kg) improve postoperative analgesia and prolong tourniquet tolerance, while sodium bicarbonate enhances local anesthetic effectiveness. The addition of potassium and temperature alterations may also improve analgesia. These adjuncts contribute to better postoperative outcomes during IVRA.7,8 Additionally, it can be used to treat complex regional pain syndromes.9
Yari et al. (2020) highlighted the benefits of the Bier block, including minimized distortion of soft tissue planes and a reduced requirement for general anesthesia.10 Our case effectively demonstrates these advantages, as patient remained pain free (VAS 0/10) throughout the surgery, eliminating the need for both the general as well as other forms of regional anesthesia. It also confirms the Bier block's applicability for tibial surgery, paving the way for further exploration in lower limb applications.
Khanduri (2008) discusses a broad spectrum of regional anesthesia techniques utilized in orthopedic surgeries, asserting that regional anesthesia can achieve high success rates and patient satisfaction when administered skillfully.11 Our findings reinforce this perspective, as our patient remained exceptionally comfortable and pain-free throughout the procedure, requiring no additional analgesia. This highlights the Bier block's capability to provide effective anesthesia and postoperative pain relief for lower limb surgeries, in alignment with existing studies demonstrating its reliability and patient comfort.
4. CONCLUSION
The successful implementation of the Bier block for tibial surgery in this case, supports its efficacy and safety as a regional anesthesia technique for lower limb procedures. The current literature and recent advancements in regional anesthesia highlight the importance of continued research and refinement. Bier blocks in lower limb surgeries offers patient satisfaction, reduced PACU and hospital stay and improved surgical outcomes.
5. Conflict of interest
All authors declare that there was no conflict of interest.
6. Consent for publ ication
Not applicable.
7. Authors’ contribution
All authors took part in the literature search, conduct of the case and drafting the manuscript.
8. REFERENCES
- Bou-Merhi JS, Gagnon AR, Laurent JYS, Bissonnette M, Chollet AA. Intravenous regional anesthesia administered by the operating plastic surgeon: is it safe and efficient? Experience of a medical center. Plast Reconstr Surg. 2007;120(6):1591–7. PubMed DOI: 1097/01.prs.0000282105.02623.38
- Broux V. An upper arm Bier block versus a forearm mini-Bier block: a randomized controlled trial in patients undergoing hand surgery. In: Faculty of Medicine and Life Sciences,School for Life Sciences, Master of Biomedical Sciences, Master's thesis; 2019. Available from: https://documentserver.uhasselt.be/bitstream/1942/29292/1/d11c33b6-ed55-425c-a5b8-5d868f1104e0.pdf
- Vaughn N, Rajan N, Darowish M. Intravenous regional anesthesia using a forearm tourniquet: a safe and effective technique for outpatient hand procedures. Hand (N Y). 2020;15(3):353–9. PubMed DOI: 1177/1558944718812190
- Prem A, Anand S. General topics: Bier block. In: Banik RK, editor. Anesthesiology In-Training Exam Review: Regional Anesthesia and Chronic Pain. Cham: Springer Int Publ; 2022. p. 41–4. DOI: 1007/978-3-030-87266-3_8
- Abdelraheem Mohamed M, Soliman FI, Elsayed HMA. Comparative study between using lidocaine alone versus using lidocaine combined with either ketamine, nitroglycerine or paracetamol for Bier block in upper limb surgeries distal to the elbow: a prospective double-blind randomized clinical trial. Egypt J Hosp Med. 2023;92(1):6642-9. DOI: 21608/ejhm.2023.316922
- Aslam S, Ahmed H, Rauf M. Comparison of ketamine, nelbuphin, and ondansetron as adjuncts in Bier’s block. Prof Med J. 2022;29(11). DOI: 29309/TPMJ/2022.29.11.7172
- Candido KD, Tharian AR, Winnie AP. Intravenous regional block for upper and lower extremity surgery. In: Hadzic A, editor. Hadzic’s Textbook of Regional Anesthesia and Acute Pain Management. 2nd ed. New York: McGraw-Hill Educ; 2017.
- Ghaderi K, Rahmani K, Rahmanpanah N, Shami S, Zahedi F, Nasseri K. Comparison of lidocaine–dexmedetomidine and lidocaine–saline on the characteristics of the modified forearm bier block: a clinical trial. J Anaesthesiol Clin Pharmacol. 2021;37(4):610. PubMed DOI: 4103/joacp.JOACP_54_20
- Löser B, Petzoldt M, Löser A, Bacon DR, Goerig M. Intravenous regional anesthesia: a historical overview and clinical review. J Anesth Hist. 2019;5(3):99–108. PubMed DOI: 1016/j.janh.2018.10.007
- Yari SS, Hafkin J, Khan J, Netscher D. A modern approach to the Bier block technique. SN Compr Clin Med. 2020;2(10):1890–9.
- Khanduri K. Regional anaesthesia techniques for orthopaedic surgery. Med J Armed Forces India. 2008;64(2):108–10. PubMed DOI: 1016/S0377-1237(08)80048-2