Barak Waris 1, Nauman Ismat Butt 2, Ayman Bashir 3, Imania Khizar 4, Ayesha Afzal 5
Authors affiliations:
Phone: +92 345 4651049
We present the case of a 17-year-old female who developed Janeway lesions as a cutaneous manifestation of infective endocarditis caused by Staphylococcus aureus. The patient presented with a 7-day history of high-grade fever, chills, body aches, palpitations, and exertional shortness of breath. Physical examination revealed multiple purplish-red, non-itchy macules on both hands and left foot, consistent with Janeway lesions. Cardiovascular examination demonstrated a grade 4 pan-systolic murmur at the mitral area and a grade 4 early diastolic murmur at the aortic areaBlood cultures identified Staphylococcus aureus, sensitive to vancomycin and gentamycin. Transthoracic echocardiography revealed vegetations on the mitral valve and moderate-to-severe mitral regurgitation. Fundoscopy did not reveal Roth’s spots, and tests for ANA, HBV, HCV and HIV were negative. The patient was diagnosed with infective endocarditis and started on intravenous vancomycin and gentamycin, showing clinical improvement. She was discharged on vancomycin to complete a 6-week course of treatment. This case underscores the importance of recognizing cutaneous signs, such as Janeway lesions, which can aid in the early diagnosis of infective endocarditis and guide appropriate treatment.
Abbreviations: ANA: Antinuclear Antibody, CRP: C-reactive protein, ESR: erythrocyte sedimentation rate, LFTs: liver function tests, PML: posterior mitral leaflet, RFTs: renal function tests, TLC: total leukocyte count,
Keywords: Janeway Lesions; Infective Endocarditis; Septic Embolism; Staphylococcus Aureus; Vancomycin
Citation: Waris B, Butt NI, Bashir A, Khizar I, Afzal A. Janeway lesions in infective endocarditis: an old clinical sign revisited. Anaesth. pain intensive care 2025;29(4):442-445. DOI: 10.35975/apic.v29i4.2684
Received: February 14, 2025; Revised: June 12, 2025; Accepted: June 25, 2025
Janeway lesions and Osler nodes are skin manifestations of infective endocarditis, typically due to bacterial or fungal infections of the heart.1 First described by Dr. William Osler in 1893 and Dr. Edward Janeway in 1899, these lesions help diagnose infective endocarditis. Janeway lesions are seen in acute cases often caused by Staphylococcus aureus, while Osler nodes are associated with subacute endocarditis.2,3 Risk factors include prosthetic heart valves, structural heart diseases and intravenous drug use.4 Janeway lesions are non-tender, erythematous or hemorrhagic macules or papules, commonly on the palms and soles, lasting days to weeks.2,3 Pain helps differentiate them from Osler nodes, as Janeway lesions are painless. Osler nodes are tender, purple-pink nodules (1-1.5 mm) with a pale center, typically found on the fingers and toes. They are painful before developing and resolve in hours to days. Both lesions result from micro-emboli that lodge in different areas of the body, leading to dermal micro-abscesses.3,4 Osler nodes are linked to emboli in the glomus apparatus, while Janeway lesions result from vascular emboli. Bacteria may not always be seen on histology, requiring tissue culture for diagnosis. Differentiating Osler nodes and Janeway lesions is important as they resemble other conditions like palpable purpura in vasculitides or disseminated infections.4,5 Other possible causes of purple lesions include drug eruptions, sun exposure and rarely calciphylaxis.5,6
Herein we report the case of a young, otherwise healthy female who presented with Janeway lesions due to infective endocarditis caused by staphylococcus aureus. This case highlights the importance of recognizing cutaneous signs like Janeway lesions, which can serve as key indicators of underlying systemic infections such as infective endocarditis. Early identification and treatment can prevent complications, emphasizing the need for clinicians to consider infective endocarditis even in atypical presentations. Additionally, it underscores the role of thorough diagnostic workup, including blood cultures and echocardiography, in confirming the diagnosis and guiding effective management.
A 17-year-old female presented with a high-grade fever for 7 days, reaching up to 102°F, accompanied by chills and generalized body aches, which were somewhat alleviated by taking paracetamol. She also experienced palpitations and shortness of breath on exertion, which improved with rest. Over time, she developed multiple painless, purplish-red, non-itchy skin lesions on both hands. She denied having a history of sore throat, joint pain, gastrointestinal symptoms, urinary issues, hemiplegia, dental problems or previous rheumatic fever. She is unmarried and has no history of sexual activity. Additionally, she does not smoke, consume alcohol or use illicit drugs.
Upon examination, the patient appeared pale and had a temperature of 101°F. Notable findings included multiple flat, painless, purplish-red macules on the dorsum and palm of both hands (Figures 1 and 2) as well as on the 3rd and 4th toe of the left foot (Figure 3), which were identified as Janeway lesions. Cardiovascular examination revealed an ill-sustained, heaving apex beat at the 5th intercostal space in the mid-clavicular line, along with a grade 4 pan-systolic murmur heard at the mitral area, which was intensified during expiration. Additionally, a grade 4 early diastolic murmur was present at the aortic area, also exacerbated by expiration and when the patient was sitting up and leaning forward. No other significant findings were noted during the rest of the examination.
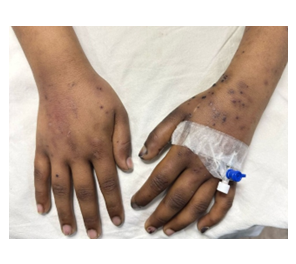
Figure 1: Multiple flat, painless, purplish-red macules of Janeway lesions over dorsum of hands bilaterally

Figure 2: Multiple flat, painless, purplish-red macules of Janeway lesions over palm of hands bilaterally

Figure 3: Janeway lesions on 3rd and 4th toe of left foot
On investigation, the patient’s hemoglobin level was 8.9 g/dl, with a normal total leukocyte count (TLC) and platelet count. Her renal function tests (RFTs), liver function tests (LFTs) and urinalysis were all within normal limits. However, both the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) were elevated, with values of 80 mm/1st hour and 113.3 mg/L, respectively. The ASO titer was negative. Blood cultures identified gram-positive Staphylococcus aureus, which was sensitive to vancomycin and gentamycin. Transthoracic echocardiography revealed vegetations on the anterior mitral leaflet (AML) and the posterior mitral leaflet (PML) along with moderate-to-severe mitral regurgitation in addition to moderate aortic regurgitation. Fundoscopy performed by an ophthalmologist did not show any Roth’s spots, and the fundus examination was otherwise normal. The tests for Antinuclear Antibody (ANA), hepatitis B virus (HBsAg), hepatitis C virus (Anti-HCV) and Human Immunodeficiency Virus (Anti-HIV) were all negative. An arterial Doppler of both the upper and lower limbs showed normal blood flow.
The patient was diagnosed with infective endocarditis complicated by Janeway lesions, caused by Staphylococcus aureus. She was treated with injectable vancomycin (30mg/kg body weight/24 hours) and gentamycin (3mg/kg body weight/24 hours for 5 days) in addition to symptomatic supportive therapy, and showed clinical improvement during the hospital stay. She was discharged on vancomycin to complete a 6-week course of treatment. A plan was made for regular outpatient follow-up, with repeat echocardiograms every two weeks to monitor the resolution of the vegetations.
This case presents a young, otherwise healthy female with Janeway lesions resulting from infective endocarditis caused by Staphylococcus aureus, underscoring the significance of identifying skin signs for early detection. Early diagnosis and comprehensive testing, including blood cultures and echocardiography, are essential for proper treatment and avoiding complications. Infective Endocarditis is a rare but serious condition that can cause severe complications, including cardiac failure, septic embolism, and high mortality if not treated early.7 Valvular disease and other structural heart issues increase the risk of infection by bacteria and fungi.8 Delayed diagnosis of Infective Endocarditis can lead to increased vegetation size and septic embolism, highlighting the importance of early diagnosis to assess the size, location of vegetations, and infection extent.7,8
The highest incidence of IE occurs in those aged >70 years, with risk factors including prosthetic valves, intracardiac devices, diabetes, hemodialysis, and intravenous drug use.9,10 Our patient, however, was young and had no apparent risk factors for infective endocarditis. Therefore, the presence of Janeway lesions aided in establishing the diagnosis timely. Staphylococcus aureus is the most common pathogen in IE, responsible for over half of cases.11 In this case, the pathogen was Staphylococcus aureus, sensitive to vancomycin and gentamycin. Our patient improved after treatment, and repeat echocardiography was scheduled for monitoring. Surgical intervention is usually indicated for severe valve dysfunction, heart failure, prosthetic valve infection, large mobile vegetations, recurrent embolism, or persistent sepsis despite adequate antibiotics.5,12 Since our patient did not face these complications and responded well to antibiotics, surgery was not necessary.
In conclusion, recognizing cutaneous signs such as Janeway lesions is essential for the early detection of infective endocarditis, enabling timely intervention. This case highlights the importance of a thorough diagnostic workup and vigilant clinical evaluation in managing atypical presentations of the condition.
5. Ethical considerations
Detailed informed consent was taken from the patient and her parents prior to data collection and manuscript writing. Anonymity of the patient has been concealed.
6. Conflict of interest
None declared by the authors. No external or industry funding was involved.
7. Authors contribution
This study was conceived and designed by BW, NIB and MSAG. BW, NIB, MSAG and IK did the initial literature research.
BW, AB, IK and AA did the data collection, patient assembly and patient assessment.
BW, IK and AB were involved in manuscript writing.
NIB, MSAG and AA did the final critical review and corrections. NIB is the corresponding author on behalf of all other authors.
Authors affiliations:
- Barak Waris, House Physician, Department of Cardiology, Chaudhary Muhammad Akram Teaching & Research Hospital, Azra Naheed Medial College, Lahore, Pakistan; Email: barakwaris23@gmail.com
- Nauman Ismat Butt, Nauman Ismat Butt, MBBS, CHPE, CHR, FCPS Medicine, FCPS Rheumatology, Assistant Professor of Medicine & Allied, Azra Naheed Medial College, Lahore, Pakistan; Email: nauman_ib@yahoo.com;
- Ayman Bashir, House Physician, Department of Cardiology, Chaudhary Muhammad Akram Teaching & Research Hospital, Azra Naheed Medial College, Lahore, Pakistan; Email: ayman_is_bashir@hotmail.com
- Imania Khizar, House Physician, Department of Medicine & Allied, Chaudhary Muhammad Akram Teaching & Research Hospital, Azra Naheed Medial College, Lahore, Pakistan; Email: imaniakhizar18@gmail.com
- Ayesha Afzal, House Physician, Department of Medicine & Allied, Chaudhary Muhammad Akram Teaching & Research Hospital, Azra Naheed Medial College, Lahore, Pakistan; ayesha.afzal0652@gmail.com
Phone: +92 345 4651049
ABSTRACT
We present the case of a 17-year-old female who developed Janeway lesions as a cutaneous manifestation of infective endocarditis caused by Staphylococcus aureus. The patient presented with a 7-day history of high-grade fever, chills, body aches, palpitations, and exertional shortness of breath. Physical examination revealed multiple purplish-red, non-itchy macules on both hands and left foot, consistent with Janeway lesions. Cardiovascular examination demonstrated a grade 4 pan-systolic murmur at the mitral area and a grade 4 early diastolic murmur at the aortic areaBlood cultures identified Staphylococcus aureus, sensitive to vancomycin and gentamycin. Transthoracic echocardiography revealed vegetations on the mitral valve and moderate-to-severe mitral regurgitation. Fundoscopy did not reveal Roth’s spots, and tests for ANA, HBV, HCV and HIV were negative. The patient was diagnosed with infective endocarditis and started on intravenous vancomycin and gentamycin, showing clinical improvement. She was discharged on vancomycin to complete a 6-week course of treatment. This case underscores the importance of recognizing cutaneous signs, such as Janeway lesions, which can aid in the early diagnosis of infective endocarditis and guide appropriate treatment.
Abbreviations: ANA: Antinuclear Antibody, CRP: C-reactive protein, ESR: erythrocyte sedimentation rate, LFTs: liver function tests, PML: posterior mitral leaflet, RFTs: renal function tests, TLC: total leukocyte count,
Keywords: Janeway Lesions; Infective Endocarditis; Septic Embolism; Staphylococcus Aureus; Vancomycin
Citation: Waris B, Butt NI, Bashir A, Khizar I, Afzal A. Janeway lesions in infective endocarditis: an old clinical sign revisited. Anaesth. pain intensive care 2025;29(4):442-445. DOI: 10.35975/apic.v29i4.2684
Received: February 14, 2025; Revised: June 12, 2025; Accepted: June 25, 2025
1. INTRODUCTION
Janeway lesions and Osler nodes are skin manifestations of infective endocarditis, typically due to bacterial or fungal infections of the heart.1 First described by Dr. William Osler in 1893 and Dr. Edward Janeway in 1899, these lesions help diagnose infective endocarditis. Janeway lesions are seen in acute cases often caused by Staphylococcus aureus, while Osler nodes are associated with subacute endocarditis.2,3 Risk factors include prosthetic heart valves, structural heart diseases and intravenous drug use.4 Janeway lesions are non-tender, erythematous or hemorrhagic macules or papules, commonly on the palms and soles, lasting days to weeks.2,3 Pain helps differentiate them from Osler nodes, as Janeway lesions are painless. Osler nodes are tender, purple-pink nodules (1-1.5 mm) with a pale center, typically found on the fingers and toes. They are painful before developing and resolve in hours to days. Both lesions result from micro-emboli that lodge in different areas of the body, leading to dermal micro-abscesses.3,4 Osler nodes are linked to emboli in the glomus apparatus, while Janeway lesions result from vascular emboli. Bacteria may not always be seen on histology, requiring tissue culture for diagnosis. Differentiating Osler nodes and Janeway lesions is important as they resemble other conditions like palpable purpura in vasculitides or disseminated infections.4,5 Other possible causes of purple lesions include drug eruptions, sun exposure and rarely calciphylaxis.5,6
Herein we report the case of a young, otherwise healthy female who presented with Janeway lesions due to infective endocarditis caused by staphylococcus aureus. This case highlights the importance of recognizing cutaneous signs like Janeway lesions, which can serve as key indicators of underlying systemic infections such as infective endocarditis. Early identification and treatment can prevent complications, emphasizing the need for clinicians to consider infective endocarditis even in atypical presentations. Additionally, it underscores the role of thorough diagnostic workup, including blood cultures and echocardiography, in confirming the diagnosis and guiding effective management.
2. CASE REPORT
A 17-year-old female presented with a high-grade fever for 7 days, reaching up to 102°F, accompanied by chills and generalized body aches, which were somewhat alleviated by taking paracetamol. She also experienced palpitations and shortness of breath on exertion, which improved with rest. Over time, she developed multiple painless, purplish-red, non-itchy skin lesions on both hands. She denied having a history of sore throat, joint pain, gastrointestinal symptoms, urinary issues, hemiplegia, dental problems or previous rheumatic fever. She is unmarried and has no history of sexual activity. Additionally, she does not smoke, consume alcohol or use illicit drugs.
Upon examination, the patient appeared pale and had a temperature of 101°F. Notable findings included multiple flat, painless, purplish-red macules on the dorsum and palm of both hands (Figures 1 and 2) as well as on the 3rd and 4th toe of the left foot (Figure 3), which were identified as Janeway lesions. Cardiovascular examination revealed an ill-sustained, heaving apex beat at the 5th intercostal space in the mid-clavicular line, along with a grade 4 pan-systolic murmur heard at the mitral area, which was intensified during expiration. Additionally, a grade 4 early diastolic murmur was present at the aortic area, also exacerbated by expiration and when the patient was sitting up and leaning forward. No other significant findings were noted during the rest of the examination.

Figure 1: Multiple flat, painless, purplish-red macules of Janeway lesions over dorsum of hands bilaterally

Figure 2: Multiple flat, painless, purplish-red macules of Janeway lesions over palm of hands bilaterally

Figure 3: Janeway lesions on 3rd and 4th toe of left foot
On investigation, the patient’s hemoglobin level was 8.9 g/dl, with a normal total leukocyte count (TLC) and platelet count. Her renal function tests (RFTs), liver function tests (LFTs) and urinalysis were all within normal limits. However, both the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) were elevated, with values of 80 mm/1st hour and 113.3 mg/L, respectively. The ASO titer was negative. Blood cultures identified gram-positive Staphylococcus aureus, which was sensitive to vancomycin and gentamycin. Transthoracic echocardiography revealed vegetations on the anterior mitral leaflet (AML) and the posterior mitral leaflet (PML) along with moderate-to-severe mitral regurgitation in addition to moderate aortic regurgitation. Fundoscopy performed by an ophthalmologist did not show any Roth’s spots, and the fundus examination was otherwise normal. The tests for Antinuclear Antibody (ANA), hepatitis B virus (HBsAg), hepatitis C virus (Anti-HCV) and Human Immunodeficiency Virus (Anti-HIV) were all negative. An arterial Doppler of both the upper and lower limbs showed normal blood flow.
The patient was diagnosed with infective endocarditis complicated by Janeway lesions, caused by Staphylococcus aureus. She was treated with injectable vancomycin (30mg/kg body weight/24 hours) and gentamycin (3mg/kg body weight/24 hours for 5 days) in addition to symptomatic supportive therapy, and showed clinical improvement during the hospital stay. She was discharged on vancomycin to complete a 6-week course of treatment. A plan was made for regular outpatient follow-up, with repeat echocardiograms every two weeks to monitor the resolution of the vegetations.
3. DISCUSSION
This case presents a young, otherwise healthy female with Janeway lesions resulting from infective endocarditis caused by Staphylococcus aureus, underscoring the significance of identifying skin signs for early detection. Early diagnosis and comprehensive testing, including blood cultures and echocardiography, are essential for proper treatment and avoiding complications. Infective Endocarditis is a rare but serious condition that can cause severe complications, including cardiac failure, septic embolism, and high mortality if not treated early.7 Valvular disease and other structural heart issues increase the risk of infection by bacteria and fungi.8 Delayed diagnosis of Infective Endocarditis can lead to increased vegetation size and septic embolism, highlighting the importance of early diagnosis to assess the size, location of vegetations, and infection extent.7,8
The highest incidence of IE occurs in those aged >70 years, with risk factors including prosthetic valves, intracardiac devices, diabetes, hemodialysis, and intravenous drug use.9,10 Our patient, however, was young and had no apparent risk factors for infective endocarditis. Therefore, the presence of Janeway lesions aided in establishing the diagnosis timely. Staphylococcus aureus is the most common pathogen in IE, responsible for over half of cases.11 In this case, the pathogen was Staphylococcus aureus, sensitive to vancomycin and gentamycin. Our patient improved after treatment, and repeat echocardiography was scheduled for monitoring. Surgical intervention is usually indicated for severe valve dysfunction, heart failure, prosthetic valve infection, large mobile vegetations, recurrent embolism, or persistent sepsis despite adequate antibiotics.5,12 Since our patient did not face these complications and responded well to antibiotics, surgery was not necessary.
4. CONCLUSION
In conclusion, recognizing cutaneous signs such as Janeway lesions is essential for the early detection of infective endocarditis, enabling timely intervention. This case highlights the importance of a thorough diagnostic workup and vigilant clinical evaluation in managing atypical presentations of the condition.
5. Ethical considerations
Detailed informed consent was taken from the patient and her parents prior to data collection and manuscript writing. Anonymity of the patient has been concealed.
6. Conflict of interest
None declared by the authors. No external or industry funding was involved.
7. Authors contribution
This study was conceived and designed by BW, NIB and MSAG. BW, NIB, MSAG and IK did the initial literature research.
BW, AB, IK and AA did the data collection, patient assembly and patient assessment.
BW, IK and AB were involved in manuscript writing.
NIB, MSAG and AA did the final critical review and corrections. NIB is the corresponding author on behalf of all other authors.
8. REFERENCES
- Parashar K, Daveluy S. Osler node and Janeway lesions. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557621/
- VanderWielen B, Bose S. Janeway lesions and Osler's nodes: an indication for prompt transesophageal echocardiography. Can J Anaesth. 2017;64(5):542–3. PubMed DOI: 1007/s12630-017-0832-1
- Kaye AD, Islam RK, Tong VT, McKee E, Gonzales JJ, Rais MS, et al. Cutaneous dermatologic manifestations of cardiovascular diseases: a narrative review. Cureus. 2024;16(10):e72336. PubMed DOI: 7759/cureus.72336
- Shen YC, Chang KC, Su JJ. Cutaneous manifestations of infective endocarditis as presenting signs of left atrial myxoma in a patient with acute ischemic stroke: a case report. Medicine (Baltimore). 2024;103(36):e39088. PubMed DOI: 1097/MD.0000000000039088
- Arish M, Butt NI, Iqbal M, Ghoauri MSA, Tariq A, Uddin N. A case study: left atrial mural vegetations in a patient with infective endocarditis complicated by septic embolism. Proc Szmc. 2024;38(3):244–7. DOI: 47489/szmc.v38i3.537
- Castrichini M, Haemmerle RJ, Tosh PK. Cutaneous stigmata of bacterial endocarditis. JAMA Dermatol. 2024;160(5):564. PubMed DOI: 1001/jamadermatol.2024.0481
- Hosokawa S, Okayama H, Hiasa G, Kawamura G, Shigematsu T, Takahashi T, et al. Isolated left atrial infective mural endocarditis. Intern Med. 2018;57(7):957–60. PubMed DOI: 2169/internalmedicine.9559-17
- Matsumura MN, Horiuchi K, Domae K, Higuchi Y. Refractory left atrial mural endocarditis secondary to a mitral valve jet lesion requiring thoracotomy: a case report. Eur Heart J Case Rep. 2023;7(5):ytad235. PubMed DOI: 1093/ehjcr/ytad235
- Malas W, Ikram M, Ruge M, Mehta PK, Chen S. Left atrial mural endocarditis in the absence of significant structural heart disease. Am Heart J Plus. 2021;2:100009. PubMed DOI: 1016/j.ahjo.2021.100009
- Butt NI, Ashfaq F, Aftab S, Mahmood K, Anwar A. Cortical venous thrombosis in a patient with rheumatic heart disease and metallic prosthetic valves on warfarin: a case report. Prof Med J. 2022;29(8):1439–43. DOI: 29309/TPMJ/2022.29.09.7046
- Safia O, Asma J, Hana H, Sarra J, Aymen Z, Mouna J, et al. Infective endocarditis: in-hospital mortality predictive factors. Ann Cardiol Angeiol (Paris). 2024;73(2):101740. PubMed DOI: 1016/j.ancard.2024.101740
- Hou BC, Huang JT, Chen CY, Chang FC, Cheng YT, Wu VC, et al. Validation of insurance claims data on aetiology, surgical type and prosthesis for isolated valve surgery: a retrospective observational study. BMJ Open. 2025;15(2):e084197. PubMed DOI: 1136/bmjopen-2024-084197