Ahmed Maamoun Soliman 1, Sameh S. Taha 2, Ashraf E. El Agamy 3,
Mohamed I. El Seidy 4, Ahmed M. Youssef 5
Authors affiliations:
Background & objective: Obesity has been termed as an epidemic in the developed countries, although it can also be seen in poor countries. With more and more obese surgical patients, anesthetic protocols have to be evolved. Ventilation of obese patients during surgery is seen to be a prime concern. The objective of this study was to evaluate the efficacy of Pressure Controlled Ventilation-Volume Guaranteed (PCV-VG) in comparison to volume-controlled ventilation (VCV) modes in obese patients undergoing laparoscopic assisted surgery in the Trendelenburg position, with a focus on their lung compliance and oxygenation index (OI).
Methodology: This randomized controlled clinical trial involved 64 obese patients of both sexes, all with a Body Mass Index (BMI) of ≥ 30 kg/m², and classified as ASA class I or II. The participants were randomly assigned to two equal groups: the study group (Group P) using PCV-VG and the control group (Group V) using VCV.
Results: The arterial oxygen partial pressure (PaO2) and lung compliance were significantly higher in Group P compared to Group V (P < 0.05). Conversely, the peak pressure (P peak) and plateau pressure (Pplat) along with the mean pressure (P mean) as well as the oxygenation index were significantly lower in Group P compared to Group V (P < 0.05).
Conclusions: PCV-VG significantly improves lung compliance and oxygenation while maintaining lower peak and plateau pressures, with comparable hemodynamic stability and PaCO2 levels.
Abbreviations: ASA: American Society of Anesthesiologists, BMI: Body Mass Index, EtCO2: end-tidal carbon dioxide, OI: oxygenation index, PCV-VG: Pressure Controlled Ventilation-Volume Guaranteed, PIP: Peak Inspiratory Pressure, PaO2: arterial oxygen partial pressure, P peak: peak pressure, Pplat: plateau pressure, PRVC: pressure-regulated volume-controlled, VCV: volume-controlled ventilation,
Keywords: Airway Pressure; Obesity; Oxygenation index; Pressure-Controlled Ventilation-Volume-Guaranteed; Trendelenburg position; Ventilation; Volume-Controlled Ventilation
Citation: Soliman AM, El Seidy MI, Taha SS, El Agamy AES, Youssef AM. Comparative study between the effects of volume-controlled ventilation and pressure-controlled - volume guaranteed ventilation in patients with obesity during laparoscopic surgery. Anaesth. pain intensive care 2025;29(3):548-555.
DOI: 10.35975/apic.v29i3.2629
Received: May 09, 2024; Revised: October 26, 2024; Accepted: January 01, 2025
Obesity is characterized by elevated resistance to airflow, difficulty in breathing and reduced respiratory system compliance, with a Body Mass Index (BMI) exceeding 30 kg/m2.1
The combination of Carbon dioxide pneumoperitoneum with or without precipitous Trendelenburg positioning is typically necessary for assisted laparoscopic surgery to achieve an optimal surgical perspective. However, this approach can result in heightened airway pressure and adverse impacts on gas exchange.2
Elevated atelectasis and cranial displacement of the diaphragm are consequences of carbon dioxide pneumoperitoneum in conjunction with steep Trendelenburg positioning. This condition leads to a reduction in total lung volume, decreased lung compliance, and decreased functional residual capacity. Therefore, the primary objectives of anesthetic management during laparoscopic-assisted surgery are to mitigate elevated airway pressures, enhance oxygenation, and facilitate the removal of carbon dioxide.3
In the context of laparoscopic assisted surgery, elevation of intra-abdominal pressure due to CO2 pneumoperitoneum can lead to various complications, including deterioration in oxygenation, increase in airway pressure, reduction in lung volume and compliance, and elevated risk of atelectasis. Consequently, these factors can contribute to the development of hypercapnia, acidosis, and impaired oxygenation.4
Volume-Controlled Ventilation (VCV) is the optimal method during general anesthesia. This mode of ventilation guarantees sufficient minute ventilation and delivers a target tidal volume (VT) through a constant flow. However, this approach can result in increased airway pressure during laparoscopic assisted surgery.5
To obtain the optimal VT, the ventilator regulates the Peak Inspiratory Pressure (PIP) in Pressure Controlled Ventilation-Volume Guaranteed (PCV-VG) mode. The ventilator parameters are consistently modified without altering the airway pressure to achieve the desired volume. Therefore, PCV-VG offers the benefits of both VCV and Pressure Controlled Ventilation (PCV) in that it minimizes the occurrence of barotrauma, while maintaining the target minute ventilation.6
PCV-VG is a type of controlled ventilation mode that integrates the characteristics of both PCV and VCV. This mode functions as a pressure-regulated volume-controlled (PRVC) system employing autoflow ventilation. The design allows for a reduction in inspiratory pressure; which, in turn, minimizes the risk of barotrauma.3
PCV-VG is a secure ventilation method without related problems or any inferiority in maximal airway pressure, plateau pressure, and dynamic compliance, with the potential to offer advantages in terms of enhanced airway dynamics compared with VCV.7
Objectives
This study aimed to evaluate the efficacy of PCV-VG and VCV modes in obese patients, who underwent laparoscopic aided surgery in the Trendelenburg position with respect to lung compliance and oxygenation index (OI).
This investigation was registered as an investigational study with registration number NCT06117748. It was a randomized controlled trial, which included 64 obese patients, 21-60 years old, of both sexes, with BMI ≥ 30 kg/m2, ASA class I/ II and undergoing laparoscopic assisted surgery. The research was conducted over a span of one year following approval from our institutional ethics committee under reference number FMASU MD 280/2022. Written informed consent was obtained from all patients.
The criteria for exclusion were as follows: ASA III or IV, intraoperative hemodynamic instability, obese patients on home oxygen therapy, pneumoperitoneum with carbon dioxide with intra-abdominal pressure exceeding 14 mmHg, anti-Trendelenburg position, asthmatic patients, patients with [advanced renal, liver disease, pulmonary hypertension and advanced malignancy], and pregnancy.
The patients were divided into two equal groups: Group P (PCV-VG), representing the study group; and Group V (VCV), representing the control group. The use of a random number table and a closed envelope technique were used to randomly assign patients to one of the two groups.
Prior to surgery, a detailed medical history was obtained from each patient, followed by a comprehensive clinical examination. All pertinent investigations were reviewed, including complete blood count (CBC), coagulation profile, liver enzyme levels, kidney function tests, electrocardiogram (ECG), echocardiography (ECHO), pulmonary function tests, and arterial blood gas analysis (ABG). Subsequently, each patient was administered premedication comprising ondansetron 8 mg, a prokinetic agent, delivered intravenously, in addition to famotidine 20 mg IV, an H2 blocker, after the establishment of a 20G peripheral venous access. After sterilizing the skin with an alcohol swab, a local anesthetic was applied. Monitoring of ECG, noninvasive blood pressure monitoring, and pulse oximetry, was started. Following a preoxygenation period of 3-5 min, anesthesia was administered via fentanyl 1-2 µg/kg and propofol 2 mg/kg IV over 15 seconds, and atracurium 0.5 mg/kg. Tracheal intubation was performed using a direct laryngoscope. After confirming the ETT position through capnography, an arterial line was successfully inserted into the left radial artery using a 3-Fr Vygon catheter, following the performance of a modified Allen test.
The respiratory parameters were set as follows: actual VT 8 mL/kg, respiratory rate 12 breaths/min, PEEP 5 mmHg, oxygen flow 4 L/min, FiO2 0.6, and I:E ratio of 1:2. Anesthesia was maintained using 1.5-2.5 vol% end-tidal sevoflurane to regulate hemodynamic responses during the surgical procedure, keeping within a 20% range of the preoperative values.
The respiratory parameters were consistently monitored and maintained at a stable level when the EtCO2 remained below 45 mmHg. In cases where EtCO2 exceeded 45 mmHg, adjustments were made to either the respiratory rate or tidal volume to ensure that EtCO2 levels remained below this threshold. The patient was positioned supine, and pneumoperitoneum was executed with CO2 at an intraabdominal pressure of 14 mmHg. The operative table was then inclined to achieve a 30° Trendelenburg position. Lactated Ringer’s solution was administered continuously at a rate of 6-8 mL/kg/hr throughout the study period.
Data collection:
Hemodynamic parameters: mean arterial blood pressure (MAP) and heart rate were monitored for 10 min prior to anesthesia administration (T0), immediately following the onset of pneumoperitoneum, each 10 min within the initial hour, and at the conclusion of surgery. The ABGs were examined using a blood gas analyzer at T0 (the baseline ABG done in preoperative investigations) and approximately every 10 min during the initial one hour. Lung mechanics including peak airway pressure (P peak), plateau pressure (Pplat), mean airway pressure (P mean), and compliance of the respiratory system were recorded following ETT insertion (T0) and every 10 min in the first hour.
Primary outcome: OI (computed as mean airway pressure × FiO2 × 100/ PaO2).
Secondary outcomes: MAP, HR, SpO2, PaCO2, and lung compliance
Sample Size Calculation:
At least 32 cases per category comprise the sample – a total of 64 cases – achieves a power of 80% to detect an effect size of 0.3 within as well as between the groups using repeated measure ANOVA with in-between factor with level of significance of 0.05. A correlation of at most 0.5 was assumed between the repeated measures and 20% excess cases were added to compensate for the potential of drop-outs.8
Statistical analysis:
All statistical analyses were performed using SPSS v26 (IBM Inc., Chicago, IL, USA). The mean and standard deviation (SD) of quantitative variables, are presented. and compared between the two groups using an unpaired Student’s t-test. Frequency and percentage (%) were employed to represent qualitative variables. and analyzed using the Chi-square test. P < 0.05 was considered significant.
In this investigation, eligibility assessments were conducted for 81 patients, 12 patients did not satisfy the criteria, and 5 patients declined to participate in the investigation. The others were randomly assigned into two equal groups (32 patients in each). The statistical analysis and follow-up of all allocated patients were conducted (Figure 1).
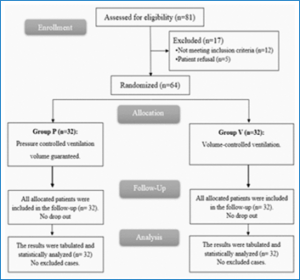
Figure 1: CONSORT flowchart of the study population
There were no significant differences between the two groups with respect to demographic data and surgical duration (Table 1).
HR, MAP, PaO2 at 10 min and at the end of surgery, PaCO2, and P peak after intubation and at 10 min, were insignificantly different between both groups. PaO2 at 20, 30, 40, 50 and 60 min was significantly higher in Group P than in group V (P < 0.05). P peak at 20, 30, 40, 50 and 60 min and at the end of surgery was significantly lower in Group P than in Group V (P < 0.05) (Table 2).
Pplat at T0 and 10 min, P mean after intubation, lung compliance after intubation, and oxygenation index after intubation, at 10 min and at the end of surgery, were not significantly different between both groups. Lung compliance at 10, 20, 30, 40, 50 and 60 min and at the end of surgery were significantly higher in Group P than in Group V (P < 0.05). Pplat, P mean and oxygenation index at 10, 20, 30, 40, 50 and 60 min and at the end of surgery were significantly lower in Group P than in Group V (P < 0.05) (Table 3).
HR and MAP immediately after pneumoperitoneum were not significantly different between the two groups (Table 4).
CO2 pneumoperitoneum is frequently used in conjunction with the Trendelenburg position during laparoscopic interventions to ensure appropriate surgical viewing and space.9 These methods significantly affect cardiovascular and pulmonary systems. These conditions lead to increased mean arterial pressure, higher P peak, reduced pulmonary compliance, and increased risk of barotrauma or atelectasis.14
The objective minute ventilation can be ensured through the application of VCV in anesthesia; Nevertheless, a constant flow rate may lead to a greater PIP, which can exacerbate the risk of barotrauma and cause an imbalanced distribution of pulmonary gases.6 In our study, the MAP was not significantly different at T0, 10 min, 20 min, 30 min, 40 min, 50 min, 60 min, and the end of surgery between both groups.Consistent with our results, Civraz et al.10 exhibited that there was no significant difference in MAP between VCV and PCV-VG in patients undergoing laparoscopic cholecystectomy.
In the present study, PaO2 was insignificantly different at 10 min and at the end of surgery between both groups and was significantly higher at 20, 30, 40, 50, and 60 min in Group P than in group V (P < 0.05). Nevertheless, Civraz et al.10 showed no significant difference between VCV and PCV-VG in cases undergoing laparoscopic cholecystectomy regarding PaO2 at all measurement intervals. This finding may be attributable to the positional disparity and the timeframe of the arterial blood gas analysis in the two investigations.
Toker et al.5 found a significantly greater PaO2 in the PCV-VG mode employed in the Trendelenburg position in obese patients. In the current investigation, the P peak was insignificantly different after intubation and 10 min between both groups and was significantly lower at 20, 30, 40, 50, and 60 min and the end of surgery in Group P than in group V (P < 0.05). Ahmed et al.11 also showed that there was a significantly higher P peak in the VCV group in contrast to PCV-VG at T1 (prior to pneumoperitoneum), T2 (fifteen minutes following pneumoperitoneum), and T3 (Five minutes following desufflation).
In our study, Pplat was insignificantly different at T0 and 10 min between the two groups and was significantly lower at 20, 30, 40, 50, 60 min, and the end of surgery in Group P than in group V (P < 0.001). In this context, Civraz et al.10 demonstrated that the Pplat results were significantly higher in the VCV group than in the PCV-VG group in patients undergoing laparoscopic cholecystectomy. In our study, Lung compliance was insignificantly different after intubation between the two groups and was significantly higher at 10 min, 20 min, 30 min, 40 min, 50 min, 60 min, and the end of surgery in Group P than in group V (P < 0.05). Consistent with our findings, Civraz et al.10 found that compliance measures were significantly lower. in the VCV group than in the PCV-VG group (p < 0.05). Moreover, it was noticed the pre-pneumoperitoneum measurement was 15% lower in the volts group than in the P group.
Recently, a meta-analysis by Schick et al.7 comparing VCV and PCV-VG showed higher dynamic compliance of the lung in PCV-VG mode. In our study, the Oxygenation index was insignificantly different after intubation, 10 min, and the end of surgery between both groups and was significantly lower at 20, 30, 40, 50, and 60 min in Group P than in group V (P < 0.05). In line with our results, Toker et al.5 compared the VCV and PCV-VG modes in laparoscopic gynecologic surgery. In this study, Toker et al.5 observed an increase in oxygenation in addition to the PCV-VG ventilation parameters. Some studies12,13 have noted a significantly high oxygenation (high PaO2) as well as improved ventilation with PCV mode; in contrast, other researchers did not observe any significant difference in relation to oxygenation and ventilation.
The limitations of this investigation were the relatively small sample size and the single-center investigation.
PCV-VG is a superior strategy for ventilation compared with VCV in obese patients who undergo laparoscopic surgery in the Trendelenburg position. PCV-VG significantly enhances lung compliance and oxygenation while maintaining lower peak and plateau pressures with comparable hemodynamic stability and PaCO2.
7. Data availability
The numerical data generated during this research is available with the authors.
8. Conflict of interest
All authors declare that there was no conflict of interest.
9. Funding
The study utilized the hospital resources only, and no external or industry funding was involved.
10. Authors’ contribution
AM: conduction of the study work
MES: manuscript editing
ST, AY: literature search
AEA: statistical analysis and review
AY: literature search
Mohamed I. El Seidy 4, Ahmed M. Youssef 5
Authors affiliations:
- Ahmed Maamoun Soliman, Assistant Lecturer of Anesthesia ,ICU and Pain Faculty of Medicine Ain Shams University, Cairo, Egypt; Email: ahmedmaamounmaamoun2013@gmail.com ; {ORCID:0000-0002-4402-9118}
- Mohamed Ismail El Seidy, Professor of Anesthesia ,ICU and Pain Faculty of Medicine Ain Shams Shams University, Cairo, Egypt; Email: drmohamed_abdelfatah@med.asu.edu.eg ; {ORCID:0009-0001-9010-3710}
- Sameh Salem Taha, Professor of Anesthesia, ICU and Pain Faculty of Medicine Ain Shams Shams University, Cairo, Egypt; Email: drsamehtaha@med.asu.edu.eg ; {ORCID:0000-0002-4761-0530}
- Ashraf El Sayed El Agamy, Professor of Anesthesia, ICU and Pain Faculty of Medicine Ain Shams Shams University, Cairo, Egypt; Email: elagamy_ashraf@yahoo.com ; {ORCID:0000-0001-6896-7662}
- Ahmed Monier Youssef, Lecturer of Anesthesia, ICU and Pain Faculty of Medicine Ain Shams Shams University, Cairo, Egypt; Email: ahmedmonier@med.asu.edu.eg ; {ORCID:0000-0002-1354-4854}
ABSTRACT
Background & objective: Obesity has been termed as an epidemic in the developed countries, although it can also be seen in poor countries. With more and more obese surgical patients, anesthetic protocols have to be evolved. Ventilation of obese patients during surgery is seen to be a prime concern. The objective of this study was to evaluate the efficacy of Pressure Controlled Ventilation-Volume Guaranteed (PCV-VG) in comparison to volume-controlled ventilation (VCV) modes in obese patients undergoing laparoscopic assisted surgery in the Trendelenburg position, with a focus on their lung compliance and oxygenation index (OI).
Methodology: This randomized controlled clinical trial involved 64 obese patients of both sexes, all with a Body Mass Index (BMI) of ≥ 30 kg/m², and classified as ASA class I or II. The participants were randomly assigned to two equal groups: the study group (Group P) using PCV-VG and the control group (Group V) using VCV.
Results: The arterial oxygen partial pressure (PaO2) and lung compliance were significantly higher in Group P compared to Group V (P < 0.05). Conversely, the peak pressure (P peak) and plateau pressure (Pplat) along with the mean pressure (P mean) as well as the oxygenation index were significantly lower in Group P compared to Group V (P < 0.05).
Conclusions: PCV-VG significantly improves lung compliance and oxygenation while maintaining lower peak and plateau pressures, with comparable hemodynamic stability and PaCO2 levels.
Abbreviations: ASA: American Society of Anesthesiologists, BMI: Body Mass Index, EtCO2: end-tidal carbon dioxide, OI: oxygenation index, PCV-VG: Pressure Controlled Ventilation-Volume Guaranteed, PIP: Peak Inspiratory Pressure, PaO2: arterial oxygen partial pressure, P peak: peak pressure, Pplat: plateau pressure, PRVC: pressure-regulated volume-controlled, VCV: volume-controlled ventilation,
Keywords: Airway Pressure; Obesity; Oxygenation index; Pressure-Controlled Ventilation-Volume-Guaranteed; Trendelenburg position; Ventilation; Volume-Controlled Ventilation
Citation: Soliman AM, El Seidy MI, Taha SS, El Agamy AES, Youssef AM. Comparative study between the effects of volume-controlled ventilation and pressure-controlled - volume guaranteed ventilation in patients with obesity during laparoscopic surgery. Anaesth. pain intensive care 2025;29(3):548-555.
DOI: 10.35975/apic.v29i3.2629
Received: May 09, 2024; Revised: October 26, 2024; Accepted: January 01, 2025
1. INTRODUCTION
Obesity is characterized by elevated resistance to airflow, difficulty in breathing and reduced respiratory system compliance, with a Body Mass Index (BMI) exceeding 30 kg/m2.1
The combination of Carbon dioxide pneumoperitoneum with or without precipitous Trendelenburg positioning is typically necessary for assisted laparoscopic surgery to achieve an optimal surgical perspective. However, this approach can result in heightened airway pressure and adverse impacts on gas exchange.2
Elevated atelectasis and cranial displacement of the diaphragm are consequences of carbon dioxide pneumoperitoneum in conjunction with steep Trendelenburg positioning. This condition leads to a reduction in total lung volume, decreased lung compliance, and decreased functional residual capacity. Therefore, the primary objectives of anesthetic management during laparoscopic-assisted surgery are to mitigate elevated airway pressures, enhance oxygenation, and facilitate the removal of carbon dioxide.3
In the context of laparoscopic assisted surgery, elevation of intra-abdominal pressure due to CO2 pneumoperitoneum can lead to various complications, including deterioration in oxygenation, increase in airway pressure, reduction in lung volume and compliance, and elevated risk of atelectasis. Consequently, these factors can contribute to the development of hypercapnia, acidosis, and impaired oxygenation.4
Volume-Controlled Ventilation (VCV) is the optimal method during general anesthesia. This mode of ventilation guarantees sufficient minute ventilation and delivers a target tidal volume (VT) through a constant flow. However, this approach can result in increased airway pressure during laparoscopic assisted surgery.5
To obtain the optimal VT, the ventilator regulates the Peak Inspiratory Pressure (PIP) in Pressure Controlled Ventilation-Volume Guaranteed (PCV-VG) mode. The ventilator parameters are consistently modified without altering the airway pressure to achieve the desired volume. Therefore, PCV-VG offers the benefits of both VCV and Pressure Controlled Ventilation (PCV) in that it minimizes the occurrence of barotrauma, while maintaining the target minute ventilation.6
PCV-VG is a type of controlled ventilation mode that integrates the characteristics of both PCV and VCV. This mode functions as a pressure-regulated volume-controlled (PRVC) system employing autoflow ventilation. The design allows for a reduction in inspiratory pressure; which, in turn, minimizes the risk of barotrauma.3
PCV-VG is a secure ventilation method without related problems or any inferiority in maximal airway pressure, plateau pressure, and dynamic compliance, with the potential to offer advantages in terms of enhanced airway dynamics compared with VCV.7
Objectives
This study aimed to evaluate the efficacy of PCV-VG and VCV modes in obese patients, who underwent laparoscopic aided surgery in the Trendelenburg position with respect to lung compliance and oxygenation index (OI).
2. METHODOLOGY
This investigation was registered as an investigational study with registration number NCT06117748. It was a randomized controlled trial, which included 64 obese patients, 21-60 years old, of both sexes, with BMI ≥ 30 kg/m2, ASA class I/ II and undergoing laparoscopic assisted surgery. The research was conducted over a span of one year following approval from our institutional ethics committee under reference number FMASU MD 280/2022. Written informed consent was obtained from all patients.
The criteria for exclusion were as follows: ASA III or IV, intraoperative hemodynamic instability, obese patients on home oxygen therapy, pneumoperitoneum with carbon dioxide with intra-abdominal pressure exceeding 14 mmHg, anti-Trendelenburg position, asthmatic patients, patients with [advanced renal, liver disease, pulmonary hypertension and advanced malignancy], and pregnancy.
The patients were divided into two equal groups: Group P (PCV-VG), representing the study group; and Group V (VCV), representing the control group. The use of a random number table and a closed envelope technique were used to randomly assign patients to one of the two groups.
Prior to surgery, a detailed medical history was obtained from each patient, followed by a comprehensive clinical examination. All pertinent investigations were reviewed, including complete blood count (CBC), coagulation profile, liver enzyme levels, kidney function tests, electrocardiogram (ECG), echocardiography (ECHO), pulmonary function tests, and arterial blood gas analysis (ABG). Subsequently, each patient was administered premedication comprising ondansetron 8 mg, a prokinetic agent, delivered intravenously, in addition to famotidine 20 mg IV, an H2 blocker, after the establishment of a 20G peripheral venous access. After sterilizing the skin with an alcohol swab, a local anesthetic was applied. Monitoring of ECG, noninvasive blood pressure monitoring, and pulse oximetry, was started. Following a preoxygenation period of 3-5 min, anesthesia was administered via fentanyl 1-2 µg/kg and propofol 2 mg/kg IV over 15 seconds, and atracurium 0.5 mg/kg. Tracheal intubation was performed using a direct laryngoscope. After confirming the ETT position through capnography, an arterial line was successfully inserted into the left radial artery using a 3-Fr Vygon catheter, following the performance of a modified Allen test.
The respiratory parameters were set as follows: actual VT 8 mL/kg, respiratory rate 12 breaths/min, PEEP 5 mmHg, oxygen flow 4 L/min, FiO2 0.6, and I:E ratio of 1:2. Anesthesia was maintained using 1.5-2.5 vol% end-tidal sevoflurane to regulate hemodynamic responses during the surgical procedure, keeping within a 20% range of the preoperative values.
The respiratory parameters were consistently monitored and maintained at a stable level when the EtCO2 remained below 45 mmHg. In cases where EtCO2 exceeded 45 mmHg, adjustments were made to either the respiratory rate or tidal volume to ensure that EtCO2 levels remained below this threshold. The patient was positioned supine, and pneumoperitoneum was executed with CO2 at an intraabdominal pressure of 14 mmHg. The operative table was then inclined to achieve a 30° Trendelenburg position. Lactated Ringer’s solution was administered continuously at a rate of 6-8 mL/kg/hr throughout the study period.
Data collection:
Hemodynamic parameters: mean arterial blood pressure (MAP) and heart rate were monitored for 10 min prior to anesthesia administration (T0), immediately following the onset of pneumoperitoneum, each 10 min within the initial hour, and at the conclusion of surgery. The ABGs were examined using a blood gas analyzer at T0 (the baseline ABG done in preoperative investigations) and approximately every 10 min during the initial one hour. Lung mechanics including peak airway pressure (P peak), plateau pressure (Pplat), mean airway pressure (P mean), and compliance of the respiratory system were recorded following ETT insertion (T0) and every 10 min in the first hour.
Primary outcome: OI (computed as mean airway pressure × FiO2 × 100/ PaO2).
Secondary outcomes: MAP, HR, SpO2, PaCO2, and lung compliance
Sample Size Calculation:
At least 32 cases per category comprise the sample – a total of 64 cases – achieves a power of 80% to detect an effect size of 0.3 within as well as between the groups using repeated measure ANOVA with in-between factor with level of significance of 0.05. A correlation of at most 0.5 was assumed between the repeated measures and 20% excess cases were added to compensate for the potential of drop-outs.8
Statistical analysis:
All statistical analyses were performed using SPSS v26 (IBM Inc., Chicago, IL, USA). The mean and standard deviation (SD) of quantitative variables, are presented. and compared between the two groups using an unpaired Student’s t-test. Frequency and percentage (%) were employed to represent qualitative variables. and analyzed using the Chi-square test. P < 0.05 was considered significant.
3. RESULTS
In this investigation, eligibility assessments were conducted for 81 patients, 12 patients did not satisfy the criteria, and 5 patients declined to participate in the investigation. The others were randomly assigned into two equal groups (32 patients in each). The statistical analysis and follow-up of all allocated patients were conducted (Figure 1).

Figure 1: CONSORT flowchart of the study population
There were no significant differences between the two groups with respect to demographic data and surgical duration (Table 1).
| Table 1: Demographic data and surgery duration in the studied groups | ||||
| Parameter | Group P
(n = 32) |
Group V
(n = 32) |
P value | |
| Age (years) | 42.38 ± 10.64 | 45.5 ± 11.29 | 0.259 | |
| Gender | Male | 15 (46.88) | 11 (34.38) | 0.309 |
| Female | 17 (53.13) | 21 (65.63) | ||
| Weight (kg) | 98.97 ± 14.63 | 104.09 ± 10.6 | 0.114 | |
| Height (cm) | 164.34 ± 6.3 | 166.97 ± 5.23 | 0.074 | |
| BMI (kg/m2) | 36.65 ± 5.1 | 37.47 ± 4.7 | 0.508 | |
| ASA physical status | I | 20 (62.5) | 22 (68.75) | 0.599 |
| II | 12 (37.5) | 10 (31.25) | ||
| Duration of surgery (min) | 55.31 ± 16.99 | 59.69 ± 16.65 | 0.302 | |
| Data presented as mean ± SD or frequency (%). BMI: Body mass index, ASA: The American Society of Anesthesiologists. | ||||
HR, MAP, PaO2 at 10 min and at the end of surgery, PaCO2, and P peak after intubation and at 10 min, were insignificantly different between both groups. PaO2 at 20, 30, 40, 50 and 60 min was significantly higher in Group P than in group V (P < 0.05). P peak at 20, 30, 40, 50 and 60 min and at the end of surgery was significantly lower in Group P than in Group V (P < 0.05) (Table 2).
| Table 2: Comparative hemodynamic and P peak data of the studied groups | ||||
| Parameter | Time | Group P
(n = 32) |
Group V
(n = 32) |
P value |
| HR (bpm) | Before induction (T0) | 77.09 ± 9.72 | 79.38 ± 8.54 | 0.323 |
| 10 min | 75.03 ± 9.65 | 77.91 ± 8.61 | 0.213 | |
| 20 min | 73.69 ± 9.82 | 76.81 ± 8.62 | 0.181 | |
| 30 min | 71.81 ± 9.78 | 75.34 ± 8.63 | 0.131 | |
| 40 min | 73.59 ± 10.03 | 72.66 ± 8.83 | 0.693 | |
| 50 min | 71.47 ± 9.76 | 75.44 ± 8.56 | 0.089 | |
| 60 min | 70.66 ± 9.48 | 74.31 ± 8.48 | 0.109 | |
| End of surgery | 72.56 ± 9.64 | 75.78 ± 8.85 | 0.169 | |
| MAP (mmHg) | Before induction (T0) | 93.5 ± 12.33 | 93.78 ± 10.96 | 0.923 |
| 10 min | 89.34 ± 12.49 | 92.13 ± 10.92 | 0.347 | |
| 20 min | 87.97 ± 12.28 | 91.41 ± 10.81 | 0.239 | |
| 30 min | 89.44 ± 12.39 | 87.66 ± 11.09 | 0.547 | |
| 40 min | 86.13 ± 12.44 | 89.41 ± 11.07 | 0.269 | |
| 50 min | 86.44 ± 12.91 | 89.78 ± 10.91 | 0.267 | |
| 60 min | 84.94 ± 12.46 | 88.66 ± 10.81 | 0.207 | |
| End of surgery | 87.19 ± 12.12 | 90.25 ± 11.33 | 0.300 | |
| PaO2 (mmHg) | 10 min | 181.75 ± 18.44 | 177.13 ± 18.92 | 0.326 |
| 20 min | 181.25 ± 18.66 | 166 ± 19.28 | 0.002* | |
| 30 min | 176.59 ± 18.97 | 163.75 ± 19.87 | 0.010* | |
| 40 min | 173.28 ± 18.82 | 160.47 ± 20.2 | 0.011* | |
| 50 min | 177.88 ± 18.41 | 168.09 ± 18.89 | 0.040* | |
| 60 min | 181.13 ± 18.56 | 170.81 ± 19.16 | 0.033* | |
| End of surgery | 182.06 ± 18.64 | 174.28 ± 19.62 | 0.109 | |
| PaCO2 (mmHg) | 10 min | 35.84 ± 4.33 | 36.69 ± 4.43 | 0.444 |
| 20 min | 35.88 ± 4.27 | 36.59 ± 4.32 | 0.506 | |
| 30 min | 35.03 ± 4.45 | 36.03 ± 4.4 | 0.369 | |
| 40 min | 36.78 ± 4.3 | 37.91 ± 4.28 | 0.298 | |
| 50 min | 37.28 ± 4.56 | 38 ± 4.43 | 0.525 | |
| 60 min | 38.31 ± 4.23 | 39.97 ± 4.75 | 0.146 | |
| End of surgery | 39.19 ± 4.4 | 40.31 ± 4.34 | 0.307 | |
| P peak (cmH2O) | After intubation (T0) | 15.38 ± 3.52 | 16.91 ± 4.31 | 0.124 |
| 10 min | 17.72 ± 3.4 | 18.84 ± 4.3 | 0.250 | |
| 20 min | 21.63 ± 4.01 | 24.56 ± 4.13 | 0.005* | |
| 30 min | 23.84 ± 4.21 | 27.06 ± 4.6 | 0.005* | |
| 40 min | 24.91 ± 3.4 | 28.13 ± 4.34 | 0.002* | |
| 50 min | 24.28 ± 3.67 | 27.56 ± 4.34 | 0.002* | |
| 60 min | 24.75 ± 3.95 | 29.06 ± 4.92 | < 0.001* | |
| End of surgery | 23.59 ± 3.26 | 26.81 ± 4.5 | 0.002* | |
| Data are presented as mean ± SD, PaO2: partial oxygen pressure. MAP: Mean arterial blood pressure. HR: heart rate *Significant as P ≤ 0.05. | ||||
Pplat at T0 and 10 min, P mean after intubation, lung compliance after intubation, and oxygenation index after intubation, at 10 min and at the end of surgery, were not significantly different between both groups. Lung compliance at 10, 20, 30, 40, 50 and 60 min and at the end of surgery were significantly higher in Group P than in Group V (P < 0.05). Pplat, P mean and oxygenation index at 10, 20, 30, 40, 50 and 60 min and at the end of surgery were significantly lower in Group P than in Group V (P < 0.05) (Table 3).
| Table 3: Comparative respiratory indices of the study groups | ||||
| Parameter | Time | Group P
(n = 32) |
Group V
(n = 32) |
P value |
| P plateau (cmH2O) | After intubation (T0) | 15.25 ± 3.39 | 13.91 ± 4.31 | 0.170 |
| 10 min | 17.53 ± 3.41 | 15.84 ± 4.3 | 0.087 | |
| 20 min | 21.38 ± 4 | 23.56 ± 4.13 | 0.035* | |
| 30 min | 23.72 ± 3.98 | 26.06 ± 4.6 | 0.033* | |
| 40 min | 24.88 ± 3.46 | 27.16 ± 5.02 | 0.038* | |
| 50 min | 24.13 ± 3.37 | 26.91 ± 4.79 | 0.009* | |
| 60 min | 24.56 ± 3.96 | 28.06 ± 4.63 | 0.002* | |
| End of surgery | 23.41 ± 3.39 | 25.94 ± 4.89 | 0.019* | |
| Mean P value (cmH2O) | After intubation (T0) | 8.19 ± 1.38 | 8.91 ± 2.1 | 0.111 |
| 10 min | 8.56 ± 1.54 | 10.47 ± 2.24 | < 0.001* | |
| 20 min | 9.81 ± 1.57 | 11.53 ± 2.26 | 0.001* | |
| 30 min | 9.69 ± 1.49 | 11.22 ± 2.2 | 0.002* | |
| 40 min | 9.78 ± 1.5 | 11.28 ± 2.26 | 0.003* | |
| 50 min | 9.63 ± 1.45 | 11.38 ± 2.12 | < 0.001* | |
| 60minP | 9.97 ± 1.67 | 11.78 ± 2.14 | < 0.001* | |
| End of surgery | 10.69 ± 1.35 | 12.53 ± 2.08 | < 0.001* | |
| Lung Compliance (mL/cmH2O) | After intubation (T0) | 42.72 ± 6.69 | 40.5 ± 8.2 | 0.240 |
| 10 min | 37.75 ± 7.22 | 30.75 ± 8.61 | 0.001* | |
| 20 min | 32.22 ± 7.16 | 27.53 ± 8.89 | 0.023* | |
| 30 min | 27.69 ± 6.78 | 23.69 ± 8.71 | 0.045* | |
| 40 min | 25.84 ± 6.65 | 21.94 ± 8.31 | 0.042* | |
| 50 min | 24.41 ± 6.63 | 17.16 ± 8.25 | < 0.001* | |
| 60 min | 22.06 ± 7.09 | 17.38 ± 8.51 | 0.020* | |
| End of surgery | 21.38 ± 7.38 | 17 ± 8.46 | 0.031* | |
| Oxygenation index | After intubation (T0) | 18.16 ± 1.27 | 18.38 ± 1.52 | 0.535 |
| 10 min | 13.31 ± 3.27 | 14.69 ± 2.9 | 0.080 | |
| 20 min | 13.66 ± 2.77 | 15.38 ± 2.54 | 0.012* | |
| 30 min | 12.94 ± 2.56 | 14.94 ± 2.65 | 0.003* | |
| 40 min | 13 ± 2.49 | 14.94 ± 2.35 | 0.002* | |
| 50 min | 13.13 ± 2.18 | 14.59 ± 2.84 | 0.024* | |
| 60 min | 13.81 ± 2.64 | 15.38 ± 2.46 | 0.017* | |
| End of surgery | 13.81 ± 2.68 | 15.06 ± 2.71 | 0.068 | |
| Data are presented as mean ± SD, *Significant as P ≤ 0.05. | ||||
HR and MAP immediately after pneumoperitoneum were not significantly different between the two groups (Table 4).
| Table 4: Comparative hemodynamic data immediately after pneumoperitoneum | |||
| Parameter | Group P
(n = 32) |
Group V
(n = 32) |
P value |
| Heart rate immediately after pneumoperitoneum (beat/min) | 74.63 ± 9.69 | 77.72 ± 9.09 | 0.193 |
| MAP immediately after pneumoperitoneum (mmHg) | 89.19 ± 12.24 | 92.03 ± 11.61 | 0.344 |
| Data are presented as mean ± SD. MAP: Mean arterial blood pressure.
|
|||
4. DISCUSSION
CO2 pneumoperitoneum is frequently used in conjunction with the Trendelenburg position during laparoscopic interventions to ensure appropriate surgical viewing and space.9 These methods significantly affect cardiovascular and pulmonary systems. These conditions lead to increased mean arterial pressure, higher P peak, reduced pulmonary compliance, and increased risk of barotrauma or atelectasis.14
The objective minute ventilation can be ensured through the application of VCV in anesthesia; Nevertheless, a constant flow rate may lead to a greater PIP, which can exacerbate the risk of barotrauma and cause an imbalanced distribution of pulmonary gases.6 In our study, the MAP was not significantly different at T0, 10 min, 20 min, 30 min, 40 min, 50 min, 60 min, and the end of surgery between both groups.Consistent with our results, Civraz et al.10 exhibited that there was no significant difference in MAP between VCV and PCV-VG in patients undergoing laparoscopic cholecystectomy.
In the present study, PaO2 was insignificantly different at 10 min and at the end of surgery between both groups and was significantly higher at 20, 30, 40, 50, and 60 min in Group P than in group V (P < 0.05). Nevertheless, Civraz et al.10 showed no significant difference between VCV and PCV-VG in cases undergoing laparoscopic cholecystectomy regarding PaO2 at all measurement intervals. This finding may be attributable to the positional disparity and the timeframe of the arterial blood gas analysis in the two investigations.
Toker et al.5 found a significantly greater PaO2 in the PCV-VG mode employed in the Trendelenburg position in obese patients. In the current investigation, the P peak was insignificantly different after intubation and 10 min between both groups and was significantly lower at 20, 30, 40, 50, and 60 min and the end of surgery in Group P than in group V (P < 0.05). Ahmed et al.11 also showed that there was a significantly higher P peak in the VCV group in contrast to PCV-VG at T1 (prior to pneumoperitoneum), T2 (fifteen minutes following pneumoperitoneum), and T3 (Five minutes following desufflation).
In our study, Pplat was insignificantly different at T0 and 10 min between the two groups and was significantly lower at 20, 30, 40, 50, 60 min, and the end of surgery in Group P than in group V (P < 0.001). In this context, Civraz et al.10 demonstrated that the Pplat results were significantly higher in the VCV group than in the PCV-VG group in patients undergoing laparoscopic cholecystectomy. In our study, Lung compliance was insignificantly different after intubation between the two groups and was significantly higher at 10 min, 20 min, 30 min, 40 min, 50 min, 60 min, and the end of surgery in Group P than in group V (P < 0.05). Consistent with our findings, Civraz et al.10 found that compliance measures were significantly lower. in the VCV group than in the PCV-VG group (p < 0.05). Moreover, it was noticed the pre-pneumoperitoneum measurement was 15% lower in the volts group than in the P group.
Recently, a meta-analysis by Schick et al.7 comparing VCV and PCV-VG showed higher dynamic compliance of the lung in PCV-VG mode. In our study, the Oxygenation index was insignificantly different after intubation, 10 min, and the end of surgery between both groups and was significantly lower at 20, 30, 40, 50, and 60 min in Group P than in group V (P < 0.05). In line with our results, Toker et al.5 compared the VCV and PCV-VG modes in laparoscopic gynecologic surgery. In this study, Toker et al.5 observed an increase in oxygenation in addition to the PCV-VG ventilation parameters. Some studies12,13 have noted a significantly high oxygenation (high PaO2) as well as improved ventilation with PCV mode; in contrast, other researchers did not observe any significant difference in relation to oxygenation and ventilation.
5. LIMITATIONS
The limitations of this investigation were the relatively small sample size and the single-center investigation.
6. CONCLUSION
PCV-VG is a superior strategy for ventilation compared with VCV in obese patients who undergo laparoscopic surgery in the Trendelenburg position. PCV-VG significantly enhances lung compliance and oxygenation while maintaining lower peak and plateau pressures with comparable hemodynamic stability and PaCO2.
7. Data availability
The numerical data generated during this research is available with the authors.
8. Conflict of interest
All authors declare that there was no conflict of interest.
9. Funding
The study utilized the hospital resources only, and no external or industry funding was involved.
10. Authors’ contribution
AM: conduction of the study work
MES: manuscript editing
ST, AY: literature search
AEA: statistical analysis and review
AY: literature search
11. REFERENCES
- Shah U, Wong J, Wong DT, Chung F. Preoxygenation and intraoperative ventilation strategies in obese patients: a comprehensive review. Curr Opin Anaesthesiol. 2016;29:109-18. PubMed DOI: 1097/ACO.0000000000000267
- Choi EM, Na S, Choi SH, An J, Rha KH, Oh YJ. Comparison of volume-controlled and pressure-controlled ventilation in the Trendelenburg position for robot-assisted laparoscopic radical prostatectomy. J Clin Anesth. 2011;23:183-8. PubMed DOI: 1016/j.jclinane.2010.08.006
- Kim MS, Bai SJ, Lee JR, Choi YD, Kim YJ, Choi SH. Increase in intracranial pressure during carbon dioxide pneumoperitoneum with steep Trendenburg positioning as proven by ultrasonographic measurement of the optic nerve sheath diameter. J Endourol. 2014;28:801-6. PubMed DOI: 1089/end.2014.0019
- Kim WH, Hahm TS, Kim JA, Sim WS, Choi DH, Lee EK, et al. Prolonged inspiratory time improves gas exchange in patients undergoing laparoscopic surgery: A randomized trial. Acta Anaesthesiol Scand. 2013;57:613-22. PubMed DOI: 1111/aas.12104
- Toker MK, Altıparmak B, Uysal A, Demirbilek SG. [Comparison of pressure-controlled volume-guaranteed ventilation and volume-controlled ventilation in obese patients during gynecologic laparoscopic surgery in the Trendelenburg position]. Braz J Anesthesiol. 2019;69:553-60. PubMed DOI: 1016/j.bjan.2019.09.003
- Pu J, Liu Z, Yang L, Wang Y, Jiang J. Application of pressure-controlled ventilation volume during one-lung ventilation in thoracic surgery. Int J Clin Exp Med. 2014;7:1094-8. PubMed
- Schick V, Dusse F, Eckardt R, Kerkhoff S, Commotio S, Hinkelbein J, et al. Comparison of volume-guaranteed vs. targeted, pressure-controlled ventilation with volume-controlled ventilation during elective surgery: A systematic review and meta-analysis. J Clin Med. 2021;10:1276. PubMed DOI: 3390/jcm10061276
- Faul F, Erdfelder E, Lang AG, Buchner A. G*Power III: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods. 2007;39:175-91. PubMed DOI: 3758/bf03193146
- Li J, Ma S, Chang X, Ju S, Zhang M, Yu D, et al. Effect of pressure-controlled ventilation-volume guaranteed mode combined with individualized positive end-expiratory pressure on respiratory mechanics, oxygenation,, and lung injury in patients undergoing laparoscopic surgery in Trendelenburg position. J Clin Monit Comput. 2022;36:1155-64. PubMed DOI: 1007/s10877-021-00750-9
- Turan Civraz AZ, Saracoglu A, Saracoglu KT. Evaluation of the effect of pressure-controlled ventilation-volume guaranteed mode vs. Volume-controlled ventilation on atelectasis in patients undergoing laparoscopic surgery: A randomized controlled clinical trial. Medicina (Kaunas). 2023;59. PubMed DOI: 3390/medicina59101783
- Ahmed MH, Ismael MM, Salem AM. Effect of volume, pressure, and pressure control-volume guaranteed ventilation on cardiovascular parameters and pulmonary mechanics in obese patients undergoing laparoscopic sleeve gastrectomy. Al-Azhar Intern Med J. 2022;51:1199-208. DOI: 21608/amj.2022.230482
- Gupta SD, Kundu SB, Ghose T, Maji S, Mitra K, Mukherjee M, et al. A comparison between volume-controlled ventilation and pressure-controlled ventilation for providing better oxygenation in obese patients undergoing laparoscopic cholecystectomy. Indian J Anaesth. 2012;56:276-82. PubMed DOI: 4103/0019-5049.98777
- Movassagi R, Montazer M, Mahmoodpoor A, Fattahi V, Iranpour A, Sanaie South Comparison of pressure vs volume controlled ventilation on oxygenation parameters of obese patients undergoing laparoscopic cholecystectomy. Pak J Med Sci. 2017;33:1117-22. PubMed DOI: 12669/pjms.335.13316
- Arvizo C, Mehta ST, Yunker A. Adverse events related to Trendelenburg position during laparoscopic surgery: recommendations and review of the literature. Curr Opin Obstet Gynecol. 2018;30(4):272-278. PubMed DOI: 1097/GCO.0000000000000471